Use 'Print preview' to check the number of pages and printer settings.
Print functionality varies between browsers.
Printable page generated Sunday, 5 April 2026, 9:41 AM
Hygiene and Environmental Health Module: 1. Introduction to the Principles and Concepts of Hygiene and Environmental Health
Study Session 1 Introduction to the Principles and Concepts of Hygiene and Environmental Health
Introduction
This first study session in the Module serves to introduce you to the important concepts and key terms that are used in environmental health and hygiene. Starting with a brief description of the historical importance of hygiene and sanitation, we will explain the scope of environmental health and describe the links between hygiene, sanitation and human health. We will describe the steps in environmental health planning and give you an overview of your role in the management of hygiene and environmental health at community level. This session will help you better understand subsequent sessions in this Module.
Learning Outcomes for Study Session 1
When you have studied this session, you should be able to:
1.1 Define and use correctly each of the key words printed in bold. (SAQ 1.1)
1.2 Briefly describe the history of hygiene and environmental health and its development in Ethiopia. (SAQ 1.2)
1.3 Describe the significance of environmental health at community level. (SAQs 1.1 and 1.3)
1.4 List the environmental risk factors involved in the transmission of communicable diseases. (SAQ 1.4)
1.5 Describe the interactions between development and environment that affect human health. (SAQ 1.5)
1.6 Explain the basic components and purpose of environmental health planning. (SAQ 1.6)
1.1 Historical perspectives on hygiene and environmental health
Hygiene and sanitation have a long history at various levels of human civilisation. We can roughly divide the historical events into two periods: the ancient and the modern.
1.1.1 Prehistoric and ancient civilisation
Religious laws, such as Moses’ Law, writings in the Old and New Testaments and laws in the Koran, played major roles in the lives of ancient peoples. These laws mainly concentrated on the provision of personal hygiene. Dead bodies and contaminated surfaces were known to be unclean or unhygienic to touch. The importance of burying human faeces was also strongly indicated. The importance of body cleanliness before praying was a motive for maintaining the integrity of hygiene with a religious practice.
The importance of hygiene and sanitation flourished at the times of Greek, Roman and Egyptian civilisation. The use of private and public baths and latrines, cleaning of the body, shaving the head for protection from lice infestation, and the construction of water pipelines and sewage ditches were widely observed. The transmission of schistosomiasis (bilharzia) was linked to bathing and swimming in the Nile River. In these civilisations, the focus was on personal hygiene (hygiene) and human waste management (sanitation).
1.1.2 Modern times
A number of discoveries in the 19th century were important events for the understanding of communicable diseases. For example, the link between contaminated water and cholera was discovered by John Snow in 1854; the importance of hygienic handwashing before attending delivery of a baby was noted by Dr. Semmelweis in 1845; and the discovery that microorganisms (very small organisms only visible under a microscope) cause disease was made by Louis Pasteur around this time.
The period following the industrial revolution in Europe in the 19th century showed that improvements in sanitation, water supply and housing significantly reduced the occurrence of communicable diseases. The term ‘environmental health’ is used to describe human health in relation to environmental factors such as these. Environmental health can be defined as the control of all the factors in a person’s physical environment that have, or can have, a damaging effect on their physical, mental or social wellbeing. The issue of environmental health is now a global matter under the guidance of the United Nations (UN) through the World Health Organization.
Although hygiene and infection are vital factors in environmental health, it is also good to be aware of emerging issues such as global warming and the links between medical conditions such as cardio-vascular disease and our environment and lifestyles. Our environment is everything that surrounds us. It includes all the external influences and conditions that can affect our health, life and growth. These influences are constantly changing and the effects on our health may not be easily foreseen.
1.1.3 Hygiene and environmental health development in Ethiopia
Historical information about hygiene practice among the Ethiopian population is sparse. We will note only the organisational aspects, as follows.
- a.A formal health service was organised in the Ministry of the Interior in 1908. Hygiene and sanitation in public health was a single service.
- b.The Ministry of the Interior had a Proclamation and Legal Notices to exercise sanitation (urine handling, refuse and excreta management, street sweeping) in 1942–1943.
- c.The Ministry of Public Health was created in 1947. It organised Municipal and Provincial Public Health services to run both curative and public health. Hygiene and sanitation were the focus of these organisations.
- d.Late in the 1970s, safe water supply and sanitation became components of primary healthcare.
- e.In the 1990s, the new Constitution in 1995 and a new Health Policy in 1993 were designed to reflect the social and health needs of the Ethiopian population. Hygiene, sanitation and environmental matters are stated aims.
- f.In early 2000 the Health Extension Programme was designed and integrated into the Health Sector Development Programme as a tool to enhance hygiene and sanitation in rural and urban areas.
1.2 Definitions
1.2.1 Hygiene and sanitation
What do hygiene and sanitation mean to you from your brief reading of the historical perspectives?
Hygiene is related to personal cleanliness, such as personal hygiene (body, clothing). Sanitation refers to waste management, particularly management of human waste.
Hygiene generally refers to the set of practices associated with the preservation of health and healthy living. The focus is mainly on personal hygiene that looks at cleanliness of the hair, body, hands, fingers, feet and clothing, and menstrual hygiene.
Improvements in personal knowledge, skill and practice that modify an individual’s behaviour towards healthy practice are the focus of hygiene promotion. Safe hygiene practice includes a broad range of healthy behaviours, such as handwashing before eating and after cleaning a child’s bottom, and safe faeces disposal. When you carry out hygiene education and promotion the aim is to transfer knowledge and understanding of hygiene and associated health risks in order to help people change their behaviour to use better hygiene practices.
Sanitation means the prevention of human contact with wastes, for hygienic purposes. It also means promoting health through the prevention of human contact with the hazards associated with the lack of healthy food, clean water and healthful housing, the control of vectors (living organisms that transmit diseases), and a clean environment. It focuses on management of waste produced by human activities.
There are different types of sanitation relating to particular situations, such as:
- Basic sanitation: refers to the management of human faeces at the household level. It means access to a toilet or latrine.
- Onsite sanitation: the collection and treatment of waste at the place where it is deposited.
- Food sanitation: refers to the hygienic measures for ensuring food safety. Food hygiene is similar to food sanitation.
- Housing sanitation: refers to safeguarding the home environment (the dwelling and its immediate environment).
- Environmental sanitation: the control of environmental factors that form links in disease transmission. This category includes solid waste management, water and wastewater treatment, industrial waste treatment and noise and pollution control.
- Ecological sanitation: the concept of recycling the nutrients from human and animal wastes to the environment.
1.2.2 Environmental health
Environmental health is broader than hygiene and sanitation; it encompasses hygiene, sanitation and many other aspects of the environment that are not included in this Module such as global warming, climate change, radiation, gene technology, flooding and natural disasters. It also involves studying the environmental factors that affect health.
The World Health Organization’s definition is as follows:
Environmental health addresses all the physical, chemical, and biological factors external to a person, and all the related factors impacting behaviours. It encompasses the assessment and control of those environmental factors that can potentially affect health.
Key phrases in this definition are environmental factors and potentially affect health.
1.2.3 Components of environmental health
Table 1.1 describes the areas of environmental health and hygiene that will be of importance to you as a healthworker and that you will learn about in the rest of this Module.
| Description | Concerns |
|---|---|
| Personal hygiene | Hygiene of body and clothing |
| Water supply | Adequacy, safety (chemical, bacteriological, physical) of water for domestic, drinking and recreational use |
| Human waste disposal | Proper excreta disposal and liquid waste management |
| Solid waste management | Proper application of storage, collection, disposal of waste. Waste production and recycling |
| Vector control | Control of mammals (such as rats) and arthropods (insects such as flies and other creatures such as mites) that transmit disease |
| Food hygiene | Food safety and wholesomeness in its production, storage, preparation, distribution and sale, until consumption |
| Healthful housing | Physiological needs, protection against disease and accidents, psychological and social comforts in residential and recreational areas |
| Institutional hygiene | Communal hygiene in schools, prisons, health facilities, refugee camps, detention homes and settlement areas |
| Water pollution | Sources, characteristics, impact and mitigation |
| Occupational hygiene | Hygiene and safety in the workplace |
Figure 1.1 illustrates the various aspects of hygiene and environmental health that are described in Table 1.1. Look at the separate drawings within the figure and match each of them to one of the descriptions.
Starting at top right, the drawing there illustrates solid waste disposal in a pit. Below that is a woman cooking at a stove to show food hygiene in a cooking area. The handpump illustrates water supply. Personal hygiene is represented by the person washing themselves. The next drawing shows a storage cupboard, again illustrating food hygiene. The drawing at top left is a pit latrine to represent human waste disposal. The central drawing illustrates healthful housing. (Vector control, institutional hygiene, occupational hygiene and water pollution are not shown.)
1.3 Concepts and principles in hygiene and environmental health
We will consider diarrhoea, which is a symptom of many common diseases, as a means to understand the concept of disease transmission, the role of environmental health and the framework for hygienic improvements.
1.3.1 Environmental health and disease transmission
The description of diarrhoea transmission represents a good way to understand the pathways of disease through the environment and how environmental health and hygiene can help prevent disease transmission. Figure 1.2 shows the factors that are essential for diarrhoea transmission. (This diagram is widely used to represent these important links in disease transmission. We have included two versions of it here to help you identify it if you see it again. It is used in later sessions in this Module.)
Look first at Figure 1.2 (a). On the left is a person defecating, representing the source of diarrhoea. The infectious agent or disease agent is actively discharged by a patient or carrier of the disease. On the right is the host, who is the person that could be affected by the disease. Between the two, there is the part of the environment that links the two; in other words, the pathway that the disease travels between the source and the host. Now compare Figure 1.2(a) with Figure 1.2(b); you will see they represent the same thing.
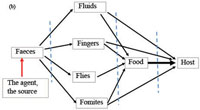
Figure 1.2(b) similarly shows the different pathways of transmission through the environment. The source of diarrhoea is the agent or carrier who discharges infected faeces to the environment. To remember the possible pathways we can use the six ‘F’s:
- Faeces: resulting from defecation.
- Fluids: through contaminated water and other contaminated liquids.
- Fingers: contaminated fingers transmit diseases.
- Flies: all sorts of animals such as flies can carry and transmit diseases.
- Fomites or fields: fomites are inanimate objects that carry the infectious agent (e.g. dishes, cups and other contaminated surfaces in contact with food or water).
- Food: infected by fluids, flies, fingers or fomites and then eaten.
A mother had diarrhoea. She was making a meal for her child but did not wash her hands before preparing the food and her child became sick with diarrhoea. Can you identify the source, pathway of disease transmission and the host?
The source is the mother who had diarrhoea; the pathway in the environment is excreta → fingers → food → mouth; and the host is the child.
If you understand the pathway of the disease, then you can design an intervention for the disease that targets the source, environment or the host. An intervention is a way of stopping the disease from being transmitted. The broken lines, in Figure 1.2, indicate the possible interventions for the prevention and control of diarrhoea. Some of these interventions are described in Table 1.2.
| Intervention strategies | Activities |
|---|---|
Intervention at the source (where the diarrhoea infection comes from) |
|
Intervention in the environment (how the diarrhoea infection is transmitted) |
|
Intervention at the host (the person who might become infected) |
|
1.3.2 The place of environmental health in your community
Our living environment is composed of home, work and recreational centres where people spend their time. Water, air and food are our concern. The provision of environmental health services extends to all these aspects of our lives.
List the locations in your kebele where environmental health is important.
You may have thought of a list that includes the following, but the detail will depend on your own kebele:
- workplaces: health facilities, local workplaces, public offices, shops, mill house, metal and wood works
- schools
- social places: church, mosque
- homes: different types of home in your area.
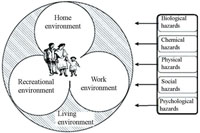
It is important to know the different parts of your kebele so that you can promote better hygiene in all areas. The interaction of the environment and possible environmental hazards are indicated in Figure 1.3. These different types of hazard will be discussed in Study Session 2.
1.3.3 Environmental intervention models
According to the Federal Ministry of Health, more than 80% of communicable diseases in Ethiopia are believed to be preventable using environmental health interventions. Generally, there are two intervention models: the clinical intervention model, which looks at treating the sick person, and the public health model, including environmental health, which looks at how to stop people getting sick in the first place by providing a healthy environment. This is indicated in Figure 1.4.
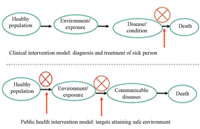
If we look at these two models in a wider context, then there are additional factors that must be considered. These include having helpful local policies, appropriate community (kebele) level organisations, sanitation legislation, developing sanitation technology options and poverty alleviation efforts. Political will in policy development in health and environmental health, designing the hygiene and sanitation legal frameworks and long-term socio-economic developments, are aspects of the government’s responsibilities. As a Health Extension Practitioner you have an important role in the prevention of environmental hazards that affect the health of the public.
1.3.4 Environmental risk factors
You have learned in previous Modules that infectious agents play a part in the transmission of disease. Infectious agents are pathogenic (disease-causing) bacteria, viruses, fungi, protozoa and parasites. To cause a disease, they must be introduced into our bodies in sufficient quantities. The environmental conditions and practices that facilitate the carrying of such infectious agents into our bodies are termed environmental risk factors. A good example is drinking water, which can be contaminated by human faecal matter that contains these infectious agents. When this water is consumed, we are likely to get diarrhoeal diseases.
There are other ways that infectious agents can get into our bodies; for example, the air we breathe can be contaminated by droplets that come out of a patient’s lungs when they breathe or cough. TB and pneumonia are droplet-related infections that are transmitted in this way. There are also diseases and conditions that are not caused by pathogenic organisms, but are caused by other environmental risk factors, which may be due to chemicals or physical hazards such as noise. Major environmental risks and examples of the diseases and conditions that are related to these risks are indicated in Table 1.3. Further descriptions of these diseases can be found in the Communicable Diseases and Non-Communicable Diseases, Emergency Care and Mental Health Modules.
| Environmental risk factors | Related diseases and conditions |
|---|---|
| Contaminated water, lack of latrines, poor hand washing, inappropriate solid waste management, open defecation, vector infestation | Diarrhoeal diseases, trachoma, schistosomiasis, ascariasis, trichuriasis, hookworm, typhoid fever, relapsing fever |
| Indoor air pollution | Chronic obstructive pulmonary disease, lower respiratory infections, lung cancer |
| Outdoor/ambient air pollution | Respiratory infections, cardiovascular diseases, lung cancer |
| General environmental hazards (climate, mosquitoes, nutrition) | Diarrhoeal diseases, malnutrition, malaria and other vector-borne diseases; heat exhaustion |
| Environmental hazards in workplaces (excess noise, heat, dust, chemicals) | Injuries, hearing loss, cancer, asthma, back pain, chronic obstructive pulmonary disease |
1.4 Human interaction with the environment
1.4.1 Urbanisation and industrialisation
Urbanisation and industrialisation bring rural people into urban centres that may not be ready to handle the additional sanitary needs. Ethiopia is at the stage of rapid development with priorities in agriculture and industry. Currently small-scale industries that bridge agriculture and industrialisation are booming. Large-scale industries, such as textiles, food and cement, are growing. The need to improve and expand social infrastructures such as water supply, waste management and health services is obvious in order to handle the needs of the growing urban centres. As a healthworker you need to understand that these developments have environmental health risks due to overcrowding, inappropriate waste management and a shortage of safe drinking water.
1.4.2 Development as a means of interaction
Assume for a minute that a textile factory is planned to operate in your woreda. Now, think what benefits and disadvantages may arise from the introduction of this factory.
Any development requires an interaction with the environment. The obvious advantages are in terms of providing cloth, creating job opportunities and contributing to the growth of the national economy. The disadvantage is when the factory produces environmental risks. The factory uses energy, raw materials and human labour for its process of producing cloth. It generates pollutants in the form of solid waste, liquid waste, air polluting substances and noise. Such wastes can pollute the air we breathe, our food, water and soil. The poor management of these wastes results in human exposure that may subsequently affect human health as well as the environment.
Figure 1.5 shows diagrammatically the relationship between development and the environment.
In this diagram, the two arrows lying between ‘human activities’ and ‘ambient environment’ indicate the relationship between them, i.e. that development requires resources from the environment (forward arrow) and, as a result, waste could be generated as a by-product (backward arrow). In fact, there are three possible types of interaction: humans can affect the environment, the environment can affect humans, and humans and the environment can co-exist (where they sustain each other). The red arrows in Figure 1.5 indicate the negative effect if the generated waste is not properly handled. This affects the environment in the form of pollution of air, water, etc., and can have a negative influence on development.
Matters of development and health have been on the agenda in UN international conferences and meetings. The issue of sustainable development is a key message for the friendly coexistence between development and the environment. The World Commission on Environment and Development defined sustainable development as:
- development which meets the needs of the present without compromising the ability of future generations to meet their own needs.
Referring to Figure 1.5, think of different examples of the three types of interaction between human activities and the environment.
You may think of different examples; here are some that we thought of:
- a.Humans affecting the environment: deforestation, polluting surface water, loss of wildlife.
- b.The environment affecting humans: soil erosion, flooding.
- c.Friendly coexistence (sustainable development): operating a factory so that it provides goods and jobs that are needed now, without polluting the environment so that our children will have safe water in the future.
1.5 The role of environmental health in public health
Environmental health is a part of public health where the primary goal is preventing disease and promoting people’s health. Environmental health is associated with recognising, assessing, understanding and controlling the impacts of people on their environment and the impacts of the environment on the public. The role of the environmental healthworker, therefore, includes the following functions of public health:
- a.Improving human health and protecting it from environmental hazards.
- b.Developing liaison between the community and the local authority, and between the local and higher levels of administration.
- c.Acting independently to provide advice on environmental health matters;designing and developing plans of action for environmental health.
- d.Initiating and implementing health/hygiene, sanitation and environmental programmes to promote understanding of environmental health principles.
- e.Enforcing environmental legislation.
- f.Monitoring and evaluating environmental health activities, programmes and projects.
You, as a healthworker, are very much involved in all of the above except (e) and (f), which are mainly carried out by the woreda environmental healthworker. However, the kebele administrator may ask you to help with the enforcement of environmental legislation, if deemed apprioriate.
1.6 Environmental health planning
Environmental health planning refers to a systematic process by which goals are established, facts are gathered and analysed, alternative proposals and programmes are considered and compared, resources are measured, priorities are established, and strategies and activities are designed to meet the established goals or objectives within a specified period of time. You, as part of kebele cabinet, will be requested to prepare an environmental health plan. The approach to planning is similar to that described in the Health Management, Ethics and Research Module. However, the primary focus is what makes it different. The following planning steps are suggested.
1 Identifying the needs and gaps
This is essentially an inventory (or list) of problems related to environmental health in your local context. You can use various tools in order to identify these problems.
- Environmental health survey: This is a systematic survey using a questionnaire. The questionnaire contains basic indicators of environmental health such as latrine availability, source of drinking water, waste disposal systems, cleanliness of the community, etc. You will need to do some statistical analysis (proportions and averages) to refine basic indicators of environmental health for your local context. You must be careful when designing a survey as it requires time, expertise and resources. You can plan it in coordination with the woreda environmental healthworker.
- Rapid/quick assessment: This is the usual method that helps you gain a quick overview of the range of problems. The usual data collection tools that you can use for this are focused or group discussion, physical observation with checklists and interviewing people.
2 Priority setting
It is difficult to handle all identified problems due to resource limitations. You need to know in advance the available resources in the kebele. Resources can be mobilised from government, community, private organisations and NGOs. Do not rely too much on governmental resources as there are always limitations. Mobilising community resources is the best option that could be sustained. Priorities are then made on the basis of the depth and severity of the problem, the feasibility and the degree of community concern and willingness to be involved in the resource mobilisation.
3 Writing a planning report
This is a systematic description of the planning functions. The recommended sub-titles are:
- Title of the plan
- Introduction or background
- Objectives
- Strategies and activities
- Indicators
- Resources (i.e. budget, human resource and materials)
- Plan of action (i.e. activities by time and responsible person)
You should prepare and present an annual plan of action for improvement of hygiene and environmental health to the kebele head. The plan of action needs careful consideration of your work in the kebele. The activities in the plan should include identifying problems, inspection services (households, food establishments, public utilities such as water sources, health facilities), hygiene promotion, monitoring selected indicators, sanitation promotion, training of local partners, sanitation campaigns and commemorating sanitation and water days.
4 Implementing the plan
Once the plan has been approved by the kebele cabinet it can be implemented. Environmental health activities are put into practice on the ground at this stage.
5 Monitoring and evaluating the planned performance
Daily, weekly or monthly monitoring will help you check the progress of the implementation, while evaluating performance at the end of the year is useful to help you see the overall progress.
6 Learning by doing
You will be able to learn lessons from the experience of the previous year’s implementation and the achievements and failures.
Summary of Study Session 1
In Study Session 1, you have learned that:
- The historical perspectives show us that hygiene and sanitation have a deep-rooted origin. The practice of hygiene and sanitation is part of our daily life.
- There are differences between hygiene, sanitation and environmental health. While hygiene focuses on individual personal hygiene/cleanliness, sanitation often refers to waste management, and environmental health has a broader meaning beyond hygiene and sanitation, referring to where we live, work and play. The focus of environmental health is on how environmental risk factors affect human health.
- Environmental health plays a major role in the prevention and control of communicable diseases caused by pathogens, such as diarrhoea, and other diseases and conditions, such as chronic obstructive pulmonary disease caused through inhalation of air pollution.
- There are various environmental health risks that affect our health. These include water and air pollution, food contamination and the disposal of wastes into our environment.
- The interaction between humans and the environment has various forms. Urbanisation, industrialisation and development are the major forms of interaction. We should remember and try to control the disadvantages of development and not focus only on the benefits.
- Environmental health planning requires you to gain knowledge of problems in your area and to identify needs and gaps, to set priorities and find resources to solve the problems.
Self-Assessment Questions (SAQs) for Study Session 1
Now that you have completed this study session, you can assess how well you have achieved its Learning Outcomes by answering these questions. Write your answers in your Study Diary and discuss them with your Tutor at the next Study Support Meeting. You can check your answers with the Notes on the Self-Assessment Questions at the end of this Module.
SAQ 1.1 (tests Learning Outcomes 1.1 and 1.3)
Emebet is a healthworker. Her weekly environmental health activities in her kebele include inspecting ten households and checking the proper storage of drinking water, food preparation and the presence of open windows. She also visits a first cycle school. In the same week, she inspects the local mill house and advises the workers how not to get hurt by machines.
Match Emebet’s different activities with the different areas of environmental health.
Two lists follow, match one item from the first with one item from the second. Each item can only be matched once. There are 5 items in each list.
Water supply
Food hygiene/sanitation
Housing sanitation or healthful housing
School sanitation/hygiene
Occupational hygiene
Match each of the previous list items with an item from the following list:
a.Inspecting for the presence of open windows
b.Inspecting ten households and checking the proper storage of drinking water
c.Visiting a first cycle school
d.Inspecting food preparation
e.Inspecting the local mill house and advising the workers how not to get hurt by machines
- 1 = b,
- 2 = d,
- 3 = a,
- 4 = c,
- 5 = e
SAQ 1.2 (tests Learning Outcome 1.2)
Outline the differences and similarities in hygiene theory and practices in ancient and modern times.
Answer
- Hygiene and sanitation law and practices existed in ancient as well as in modern times.
- Laws in different religions are important for hygiene practices in ancient and modern times.
- Ancient hygiene practices concentrated on personal hygiene and waste management (sanitation).
- Modern understanding and practices of hygiene improved as it was discovered that microorganisms cause disease.
- Improvements in housing, water supply and sanitation have improved health.
SAQ 1.3 (tests Learning Outcome 1.3)
Make a quick visit in your village or town and make a list for yourself of the hygiene and sanitation problems that you can see.
Answer
You should have made your own list of hygiene and sanitation problems that you can see in your town or village. The list might include: poor handwashing, flies on the face, many flies around the house, excreta around the house, uncovered water container, poor solid waste management, animals are sleeping together with humans, slab of latrine is poorly maintained, children not using latrine, etc.
SAQ 1.4 (tests Learning Outcome 1.4)
Diarrhoea among children under 5 is common in many rural villages. What environmental factors or practices may cause diarrhoea in young children?
Answer
You could list environmental factors such as open defecation, presence of flies, poor waste management that could support the breeding of flies, uncovered food, contaminated plates and cups, a mother not washing her hands after cleaning a child’s bottom or a child eating with dirty fingers.
SAQ 1.5 (tests Learning Outcome 1.5)
Development in your locality may bring job opportunities. List the specific kinds of development that are found in your locality and identify the types of environmental hazard they might cause.
Answer
Your answer will depend on your local situation but examples of economic developments include: mill house, dairy farm, hollow block manufacturing, woodwork or metalwork. Possible environmental hazards due to these undertakings depend on their nature but may include: liquid waste discharged to the immediate environment, presence of noise, presence of machines that cause accidents, absence of latrines, workers welding without eye protection, etc.
SAQ 1.6 (tests Learning Outcome 1.6)
Why do we need environmental health planning? What documents will you need to use or to produce when designing environmental health planning?
Answer
Environmental health planning is needed to:
- Address what must be done effectively – to identify needs and gaps in environmental health
- Utilise resources efficiently
- Set priorities for environmental health
- Implement changes wisely in a given time frame
- Make a link with the overall kebele social development.
You will need to use an environmental health questionnaire to collect survey information and you will need to produce a planning report. You may also use previous planning and performance reports and results from earlier surveys.