4.11 Vaccination
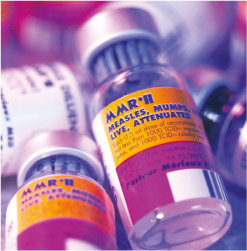
Vaccination relies on the development of immunological memory for its protective effect. Vaccines contain killed pathogens, or extracts from pathogens, or modified strains of pathogens that are no longer harmful. For example, the MMR vaccine contains weakened (the technical term is ‘attenuated’) variants of the three viruses that cause measles, mumps and rubella (Figure 12).
Why do you think most vaccines are given in two (or more) doses spaced at intervals of weeks or months?
The first dose triggers a primary adaptive immune response, but this doesn’t reach a high level and subsides over time. The second dose triggers a much more vigorous secondary response, generating a lot of memory cells, which remain on patrol to protect the child if he or she is subsequently infected with live pathogens of the same type as used in the vaccine.
Note that each of the memory cells and the T cells and B cells generated in an adaptive immune response are specifically directed against just one type of pathogen or a very closely related strain. Vaccination with MMR vaccine is only protective against measles, mumps and rubella infection.
Despite decades of effort, medical science has so far been unable to produce effective vaccines against a number of important infectious diseases, including HIV/AIDS and other sexually transmitted infections (although trials of several candidate vaccines are underway). Vaccines against malaria have shown some potential, but they only protected about half the vaccinated children in large-scale African trials (RTS,S Clinical Trials Partnership, 2012). There are no effective vaccines against infections caused by any other single-celled or multicellular parasites.
Some vaccines are effective only for a relatively short time, e.g. cholera vaccines give protection for only around six months. Others, such as the tetanus vaccine, need repeated booster doses. Annual influenza vaccinations are offered to vulnerable groups in the population because influenza viruses alter their antigens over time.
Why can’t vaccines prepared from last year’s influenza viruses be guaranteed to give protection against currently circulating flu strains?
Vaccines prepared from earlier strains of influenza viruses will not contain any of the altered antigens that currently circulating strains may have developed; last year’s vaccine cannot boost adaptive immunity against viruses with these new antigens.
The second practical challenge is organising and delivering mass vaccination programmes in low- and middle-income countries, especially in remote areas and urban shanty settlements. The terrain may be difficult, transport and communication links are often poor, and communities may not be aware when vaccination teams arrive. Most vaccines have to be kept cold or they lose their potency, but maintaining vaccines at 2–8 °C while vaccinating thousands of children in warm climates without adequate refrigeration requires ingenuity (Figure 13).

Thirdly, education programmes struggle to overcome basic lack of knowledge about vaccination, especially in communities where literacy rates are low and poverty is a daily fact of life. A survey of over 27 000 children in 24 African countries concluded that poor parental education and lack of access to information were critical factors in areas of low vaccine coverage. Only 71% of these children had received the full series of three vaccinations against diphtheria, tetanus and pertussis (whooping cough) by their first birthday, leaving an estimated six million African children unprotected (Wiysonge et al., 2012).
