1.1.2 Pre-natal diagnosis
The type of genetic testing that the majority of us are most likely to come across is still pre-natal diagnosis (PND). This involves testing a fetus during pregnancy, to see whether it is likely to suffer from a number of different disorders — some genetic, some not. While recent developments allow tests for certain multifactorial genetic diseases (such as spina bifida), pre-natal diagnosis has been available since the 1960s to test for Down's syndrome.
Most cases of Down's syndrome are the result of a new mutation arising in the gamete-producing cells. This contrasts with childhood diseases, such as cystic fibrosis (CF), which result from the fetus inheriting two recessive mutations because the parents are carriers. Here pre-natal diagnosis has removed much of the uncertainty about the risks of genetic diseases. In a family who know that both parents are carriers of CF, either because they already have a CF child (Figure 1) or as a result of carrier testing, PND allows the conversion of a probable risk of the disease affecting an unborn child to nearer a certainty that it will or will not be affected.
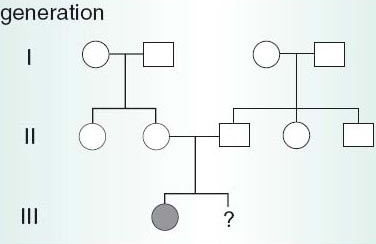
SAQ 2
Examine figure 1 above. Will the second child of the family depicted in the chart be affected with cystic fibrosis?
Answer
For an individual to suffer from cystic fibrosis they must inherit two copies of the cystic fibrosis gene, one from each parent. The parents must therefore be carriers (and they each would have inherited one copy of the cystic fibrosis gene from one of their parents, who would also have been a carrier).
The chance of having a child with cystic fibrosis is 1 in 4 for the second child and for any subsequent children, regardless as to whether or not the first child has cystic fibrosis. This is because it is based on the same two events, namely:
equal numbers of cystic fibrosis and normal gametes are produced;
male and female gametes combine at random during fertilization.
Pre-natal testing might then change the probability from 1 in 4 to near certainty that the fetus is or is not affected. However, pre-natal diagnosis cannot be used to rule out all possible birth defects, or all genetic disorders, because suitable tests do not yet exist to detect them. Nor is it foolproof even for those diseases that it can generally detect, such as CF.
Box 1 outlines the techniques for pre-natal diagnosis of fetal abnormalities early in pregnancy.
As more pre-natal testing is performed, we may see an increase in abortions since there may be no treatment for the particular disease detected. Yet this is obviously a difficult decision to make, not only in terms of the very public debates that surround abortion, but also with regard to the difficult private decisions that women (and their partners) face in these circumstances.
Box 1 Techniques for pre-natal diagnosis of fetal abnormalities
There are a number of techniques available for pre-natal diagnosis, and these are listed in Table 1 along with the abnormalities or diseases they can be used to detect.
| Technique | Abnormality/disease detected |
|---|---|
| maternal serum screening: determination of fetal protein levels | spina bifida |
| ultrasonography | organ abnormalities of nervous system, kidneys, heart, gut and limbs |
| fetoscopy | organ and limb abnormalities, skin disorders, blood disorders |
| amniocentesis: | |
| karyotype analysis | Down's syndrome |
| DNA studies | many genetic disorders |
| determination of fetal protein levels | spina bifida |
| chorionic villi sampling | genetic disorders (e.g. muscular dystrophy, cystic fibrosis, Huntington's disease) |
Maternal serum screening tests the mother's blood for the presence of proteins produced by the fetus; both it and ultrasonography are non-invasive with no known risk to the mother or fetus. Fetoscopy has the advantage that the fetus can be visualized directly by inserting a very fine optical telescope (fetoscope) through the abdominal wall into the uterine cavity. Amniocentesis involves the removal of a small amount of amniotic fluid, which bathes the developing fetus and contains fetal cells. The fluid can be analysed for its protein content, which may be abnormal in spina bifida, or chromosomes can be counted or the DNA analysed for certain genetic abnormalities. Another common approach is chorionic villi sampling, which is the removal of cells from the edge of the placenta. Most of the placenta is fetal tissue, so it is genetically identical with the cells of the fetus. This yields a greater amount of DNA than the sampling of amniotic fluid. These sampling techniques for pre-natal diagnosis are associated with a small increase in the risk of spontaneous abortion, compared with the risk in pregnancies not screened by these methods.
Supporters of pre-natal diagnosis point out that as the accuracy of the tests improve, there should be fewer abortions. At present, they argue, a substantial proportion of post-test abortions are normal pregnancies because the tests are not always accurate and decisions are based on estimated risk. To others, selective abortion of affected fetuses is always morally objectionable, and especially so when the disorder might not be life-threatening, as in many individuals with Down's syndrome. However, fewer than five per cent of all pre-natal diagnoses are, in fact, positive. So for the vast majority of prospective parents, pre-natal diagnosis serves ultimately to reassure them that the unborn baby is not affected by the disease in question.
The tensions and ambiguities that surround fetal testing have given rise to what has become labelled the ‘tentative’ pregancy. Some women, who know that they are due to have an ultrasound scan or other pre-natal test, may refuse to regard themselves as ‘properly’ pregnant, in case the test indicates a problem and they are faced with the decision of whether to abort or not. Merely offering testing and termination might be seen as implying that these choices should be taken up. Yet this suggests that a pregnant woman who agrees to pre-natal diagnosis should have made a prior commitment to terminate the pregnancy if she is carrying a fetus with a genetic (or other serious) disorder.
SAQ 3
Aside from offering the possibility of termination, what other purposes might a pre-natal test serve?
Answer
A couple might wish to be forewarned of the birth of a child with special needs, so they could prepare to care for their baby.
SAQ 3a
What sort of factors might influence personal decisions about abortion?
Answer
Moral, religious, financial, experience of knowing a family with the disease, and having an affected child already.
