Cancer patients and their families are likely to feel anxious about the continuity of their treatment plan during the COVID-19 pandemic. We have collected a series of frequently asked questions regarding patients with different stages of disease. This advice has been gathered from various sources, including cancer charities, NHS advice, and available scientific literature.
What should someone do if they suspect they have cancer-like symptoms?
If someone is concerned they might have an undiagnosed cancer, they are advised to contact their GP. They can phone their GP surgery, visit the GP surgery website or use an online service to contact their GP (for more information visit the NHS website).
Growing evidence shared in the media suggests a decrease of referrals to cancer specialists over the last few weeks.GPs will ask about your symptoms and decide whether a person should go to the clinic or be referred to a specialist for a more precise diagnosis. Hospital teams will contact the person to make an appointment and advise them on the next steps. Please be aware that due to possible disruptions or delays, hospital teams might have to prioritise appointments and tests for those who are in urgent need.
Growing evidence shared in the media suggests a decrease of referrals to cancer specialists over the last few weeks. This might be due to the fact people are reluctant to seek medical help during the pandemic that might bring them into contact with SARS-CoV-2. The NHS is still fully operational and capable of taking care of new patients. Yes, COVID-19 has put a new pressure on the NHS resources, but people should feel free to contact their local GP to get advice if they suspect they have any symptoms related to cancer. If asked to attend an appointment, social distancing and the advice provided by NHS staff should be followed.
How will COVID-19 affect cancer treatment?
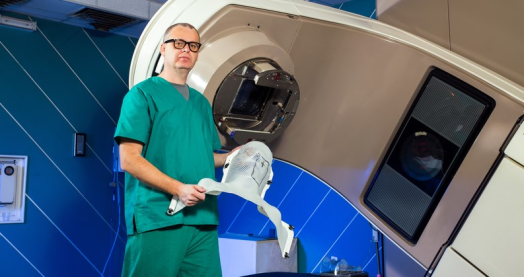
In the UK, 45% of patients diagnosed with cancer have surgery to remove the tumour as part of their primary cancer treatment. 27% of patients have radiotherapy, and 28% have chemotherapy according to Cancer Research UK. Doctors will continue to offer these cancer treatments to patients. However, it is likely that treatment plans and the frequency of treatments will be modified. Patients are advised to speak to their healthcare support team and they will be able to advise them on the best course of action.
Healthcare teams are advised to:
- Balance a delay in cancer diagnosis or treatment against the risk for a potential SARS-CoV-2 exposure,
- Mitigate the risks for significant care disruptions associated with social distancing behaviours,
- Manage the appropriate allocation of limited health care resources in these unprecedented times.
In general terms, clinicians will balance the benefits of the cancer treatment over the risk of SARS-CoV-2 infection to decide whether a cancer treatment should go ahead or be postponed.
Treatment risks regarding COVID-19 include:
- How the cancer treatments affect a patient´s immune system – patients are more at risk of becoming seriously ill from COVID-19 if their immune system is weak after treatment.
- Exposure to SARS-CoV-2 during hospital visits – the healthcare team might look at how the treatment is administered in order to reduce hospital visits.
Benefits of cancer treatment include:
- curing or delaying the progression of the cancer
- lowering the chance of the cancer coming back (relapse)
- helping patients live longer with their cancer
- controlling symptoms caused by cancer progression
The outcome of the risk/benefit assessment will be also be influenced by other factors such as urgency (in comparison to other cancer patients) and prioritising treatments based on available resources.
Will regular tests to control cancer progression be still offered?
Some patients depend on regular tests to monitor the progression of their cancer and/or the efficacy of their treatment. One example is for prostate cancer, where prostate specific antigen (PSA) tests are employed for cancer detection and for post-treatment monitoring to identify possible relapses. GPs will continue to offer this type of test as often as possible and this is likely to depend on the number of people in need of a specific test in a determined area. Patients are advised to speak to their GP to understand any modifications to their treatment plan. It is possible that tests will be rescheduled if the clinician thinks this is the safer option.
Will the coronavirus outbreak delay and/or stop current cancer treatments?
The healthcare support team will always weigh up the benefits and risks of modifying cancer treatment during the pandemic and will try to minimise any impacts on cancer treatment. Unfortunately, delays are likely due to shortage of equipment or space in hospitals.
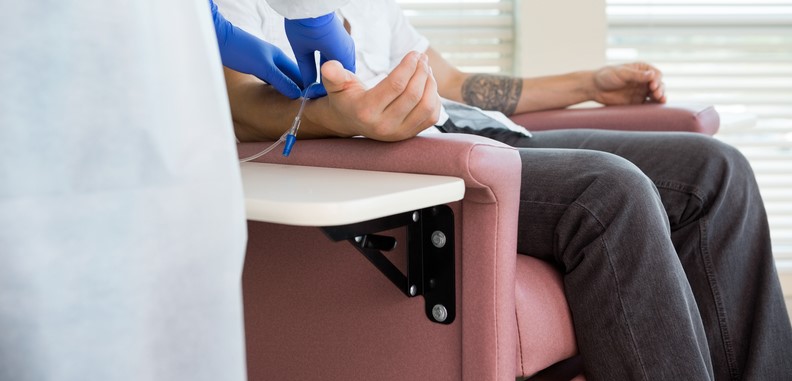
It is possible patients might be asked to reduce their visits to the hospital. Some cancer treatments can be administered orally via pills or via simple skin injections. Hence, cancer patients might be advised to start self-medicating to reduce the number of visits to the hospital. Furthermore, it is also possible that for some therapies there might be an increase in the lag between one cycle of treatment and the following one. Clinicians will weigh up the benefits and risks and discuss with the patient the best approach for their specific cancer treatment.
If a person has recovered from a past cancer, should they be especially worried about COVID-19?
People who have recovered from a past cancer or already finished cancer treatment are unlikely to be considered in the vulnerable group. However, they are still required to follow UK government advice on social distancing, and to consider other risk factors for severe COVID-19 (age, other health conditions including diabetes, obesity and cardiovascular diseases).
In this series of articles we explore how COVID-19 impacts on cancer patients and their treatment. Read on to explore how and why treatments for cancer such as chemotherapy will increase the risk of COVID-19...

Rate and Review
Rate this article
Review this article
Log into OpenLearn to leave reviews and join in the conversation.
Article reviews