1.3 Obesity
At the time of writing (2004) 20% of the adult population of the UK is classified as obese. The number of obese children has doubled since 1982, 10% of six year olds and 17% of fifteen year olds are now classified as obese. As shown in Table 4, obesity is recognized when the BMI exceeds 30 and occurs quite simply when energy intake exceeds energy expended over a period of time. However, hormonal, genetic and metabolic abnormalities can also sometimes be involved. (We will return to a consideration of these factors later.) Some obese people eat considerably more than non-obese people, particularly in the period during which they are actually increasing in weight. However, the difference between intake and metabolic expenditure need only be very small (perhaps eating an extra piece of cake every day for 3 months) to produce a cumulative weight increase over a period of months.
The House of Commons Health Committee published a report in 2004 (House of Commons Health Committee, 2004) in which the increasing problem of obesity was heavily emphasized. The report stated that the incidence of obesity has grown by almost 400% in 25 years and suggested that if it continued to grow at such a rate it would soon overtake smoking as the biggest cause of premature loss of life. The economic cost of obesity was estimated at 3.3–3.7 billion pounds per year. This cost estimate includes predicted costs of the NHS for treatment of obese patients as well as time lost to industry due to sickness.
The report makes many recommendations to government of ways of tackling obesity. Targeting the food industry to reduce food portion sizes and moderate their advertising campaigns were some of the recommendations. The report also recommended that food products were labelled more clearly and a ‘traffic light’ method for labelling foods based on their energy density was suggested. In this system ‘green’ would label foods with low energy, ‘amber’ for medium energy density and ‘red’ for high energy density.
Activity 10
What do you suppose is meant by ‘high energy density’ ?
Answer
A food with high energy density will make available far more energy for its size (i.e. per portion) than a low-energy-density food.
Activity 11
What happens if the amount of energy that can be made available exceeds current requirements?
Answer
The surplus will be stored, potentially adding to body fat.
Education of what constitutes a healthy diet was also a key recommendation, at school level and beyond. There were a number of different recommendations of ways in which to increase individuals’ exercise to the recommended level of 30 minutes five times a week, including school and workplace initiatives.
Exercise is very helpful in aiding obese individuals to lose weight as it increases their TEE. Exercise also has the advantage of increasing BMR for hours beyond the termination of exercise. A long-term advantage of exercise can be an increase in the ratio of lean/fat body weight with subsequent advantages for keeping metabolic rate high. Whilst it is desirable for obese individuals to exercise this is easier said than done and the danger is that individuals can get into a vicious circle: as weight increases so exercise decreases. This means that later, even with the will to do it, an overweight person might not be able to perform enough exercise to increase metabolism sufficiently to lose weight.
There are of course various social, economic and environmental factors that will play a role in how much exercise a person is able to take.
Activity 12
From your general knowledge summarize some of these factors.
Answer
Your summary should be a long one! It might also reflect your age and current interests. Social factors could include family responsibilities, the availability of others to participate in team games or how close you are to clubs and leisure facilities. Economic factors such as cost of membership of clubs and of sporting equipment and sports wear will limit participation by some people. Even walking, which can be a solitary activity and need not involve the outlay of any cash can be limited if one lives in an unsafe environment.
The relationship between decreased physical activity and increasing obesity within the population of the UK can be attributed to a reduction in cycling and walking and increased car use (the number of cars has doubled in 30 years) and increased television viewing (which has also doubled since the 1960s).
Activity 13
Is the relationship between decreased physical activity, increased car ownership and obesity a causal relationship?
Answer
The report is suggesting that it is.
Activity 14
Do you have any reservations about this statement?
Answer
Yes, you should. In the absence of specific data from studies that have eliminated other possible causal factors it is not possible to make inferences about causation just using a common sense approach.
The rise in the number of obese children has been associated with increased television watching, playing of computer games and safety fears of parents for their children which keeps them indoors rather than playing outside. The rise of the ‘school run’ in which children are transported to school rather than walking also does not help with increasing their physical activity levels.
Activity 15
It is known that many obese children have obese parents. What explanations might be given for this effect?
Answer
Either a genetic factor or an environmental factor, or both, could be involved.
Activity 16
How would you distinguish between these two explanations?
Answer
It would be possible to follow up genetically identical (monozygotic) twins who were separated after birth and brought up in different families.
These kinds of studies have been done and we will consider them later in this course.
Case Report 1 provides a more in-depth look into some of the causes and treatment of obesity.
Case Report 1: Obesity
Ron is 59 years old and looking forward to retiring from his sedentary desk job. He was aware that he had gained weight over a number of years and that his weight had increased more rapidly after he sprained his ankle refereeing rugby (causing his retirement from the game) a couple of years ago. He had meant to join the local gym or take up golf but had not quite got around to doing it. He was looking forward to all the time he would have to get fit again once he had retired, as the most exercise he did every day was walk to and from the bus stop to catch the bus to work, which was about 200 yards from his front door.
Ron noticed that he was starting to get breathless when he had to go upstairs and that he had developed varicose veins. He noticed that he frequently suffered from heartburn after eating and started to complain to his wife Margaret that he often just did not feel well. Margaret, a slim woman in her mid-fifties, urged him to go and have a check-up. He booked himself into the well person clinic, run by the practice nurse.
Jane, the practice nurse, started the check-up by chatting to Ron about his general health. She asked whether there was any family history of heart disease or strokes and discovered that he was not currently taking any medicines. Ron replied that his father had died of a heart attack when he was 67 years old and his mother had died following a stroke at 60 years old.
The nurse asked Ron about his current eating and exercise habits and Ron explained about the sprained ankle and the knock-on effects from that. He admitted that he liked a fried breakfast, enjoyed a canteen-cooked lunch of two courses and a cooked dinner with pudding. The nurse asked if he snacked during the day and Ron said ‘No, but I do have a chocolate biscuit with my mid-morning tea and I like to have a pint or two of beer later in the evening often with a bag of crisps’.
Jane weighed Ron (95 kg), measured his height (1.75 m) and then calculated his body mass index (BMI) as:
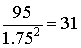
The BMI reading indicated that Ron was obese (Class I). Jane also measured Ron's waist and hips, explaining that the ratio between waist and hips should not exceed 0.95 for men over 40 years old. She explained that abdominal or central obesity is indicated by a ratio greater than 0.95 in men and 0.85 in women and that this increases the risks of heart disease and type 2 diabetes, which is an impairment of insulin activity. She was quick to point out that the possibility that Ron had these diseases would require further investigation before diagnosis could be made. Ron had a central obesity ratio of 0.96.
Jane measured Ron's blood pressure and discovered it was a bit high. Jane pointed out that this reading was a one-off reading and the usual standard for measuring blood pressure is to take one reading per week for 3 weeks. Finally Jane asked Ron to give an urine sample which she tested for glucose (glucosuria is the term used to describe glucose presence in the urine) and ketones (ketones or ketone bodies are a by-product of metabolism when there is excess glucose and ketonuria is the term used to describe the presence of ketones in the urine). Ron's urine sample was negative for glucose and ketones. Glucosuria and ketonuria are indicative of type 2 diabetes.
Jane then asked if Ron had ever considered losing weight and Ron said he would like to but did not know where to start. Jane suggested that Ron kept a diary of his daily food intake and his exercise over the next week and brought it to the next appointment. She told Ron that obesity is caused by taking in more energy than is expended over a period of time and reassured Ron that if he lost weight he would immediately start reducing the risks of the other conditions associated with obesity. She stressed that obesity is a condition that Ron himself could have some control over by eating a balanced diet and increasing his exercise. Ron left the surgery determined to enrol in a local WeightWatchers group and join the gym.
