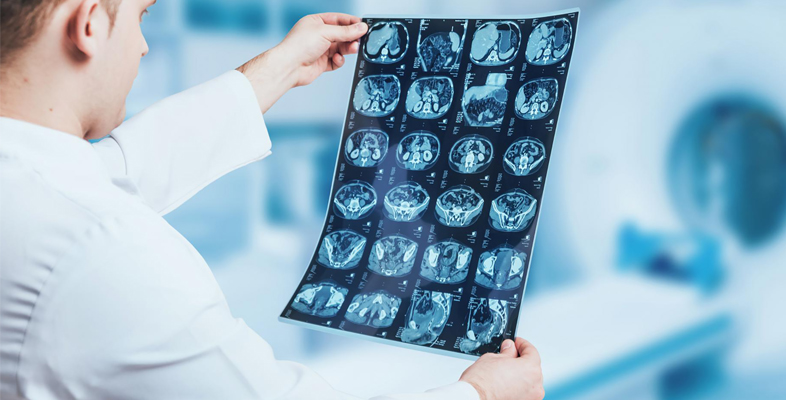
3.1 MRI in practice
It’s important to appreciate from the start that MRI involves the measurement of signals from tissues in the body.
MRI produces a 3D image of the body from a series of 2D images by measuring the signals from mobile protons – mostly in the water present in the body, but also in the protons present in fats and proteins.
These signals are presented in such a way that they may show where they originate in the body. In other words, the image that is seen represents a map of signals in real spatial dimensions.
Watch the following video which demonstrates MRI being used for diagnosis in a hospital –in fact, it’s the patient with the suspected brain injury you saw having the CT scan. It also gives an introductory account of how MRI works.
Don’t worry about terms like , and proton density; these will be explained later.
Transcript: Video 3 Obtaining an MR image of a patient. (3:03 min)
RADIOGRAPHER: It does make a very loud drilling noise, okay? So what we’re going to do is pop these earphones ...
NARRATOR: To obtain images, the patient is placed in a large, static magnetic field produced by a superconducting magnet. This powerful field, typically one and a half teslas in strength, causes the nuclei of the hydrogen atoms in the body to line up. But they can also be flipped into another direction by a radio frequency pulse.
The way these nuclei then relax back to their original position depends on the environment of the hydrogen atoms. In other words, on tissue type. When imaging small parts of the body, specialised coils are used to detect the radio frequency signal given off by the relaxing nuclei. Here a head coil is being used for this purpose.
Laser alignment is used so that the patient can be moved to the correct position in the scanner.
RADIOGRAPHER: Okay?
NARRATOR: Because the powerful magnetic fields can disrupt pacemakers, and cause heating of metal implants, every patient must be carefully checked before entering the scanner room.
RADIOGRAPHER: Okay, so we’re just going to start the scan now. Okay, so what we do first is an initial pilot scan. So that’s so we can exactly locate the patient within the scanner.
NARRATOR: With MRI, it’s possible to choose any direction for the image slices. In this case, the radiographer is taking an axial pilot scan, to give a series of coronal images.
RADIOGRAPHER: What we’ve done now is we’ve planned to scan through that area of this person’s head and we’re going to scan from front to back there. And so, okay, your first scan’s just about to start. Each scan will take about five minutes, okay? And then, after that, we can have a look through the images and we can see what we’ve got.
NARRATOR: There are many different imaging sequences that can be used. But most of them produce an image where the intensity depends mainly on one of three characteristics – T1, T2 or proton density. The intensity in these images depends largely on T2, the spin-spin relaxation time.
Substances with a long T2, such as water, appear bright. This is very obvious if you look at the eyes in this image.
RADIOGRAPHER: We’ve now gone on to sagittal images. This is a T1. So we’ve got bright fat and the fluid’s dark on these images. This is a way that we can differentiate contrast to see different pathologies or anatomy. We also scanned in the axial plane, so that’s head to toe. And again, this is T2 with bright fluid. You can see the eyes. And finally, these ones are proton density. So this is weighting – where each tissue is the protons that are actually there, rather than any specific weighting.
NARRATOR: Thankfully for this patient, the images show no abnormality.
Activity 1
Now that you have watched the video, briefly summarise the main stages in the MRI process.
Answer
The patient is placed in a strong magnetic field. This causes the protons present in molecules in the body to align with or against the magnetic field. The patient is then irradiated with pulses of radiofrequency (RF) radiation which flip these nuclei into another direction. Finally, the radio waves emitted by the subject as the protons relax back to the ground state are collected and converted, via computer processing, into an image.
As has already been mentioned, at the very basic level an MR image is formed from signals from tissue in the body. And as you’ve seen, in order to obtain these signals the body must be
- i.immersed in a strong magnetic field
- ii.irradiated at the appropriate radio frequency.
However, by itself this process will not lead to an image.
Although MRI involves the measurement of signals from tissues within the body, these signals are presented in such a way that they show where they originate from within the body.
There is thus a major difference between the spectroscopic studies used to determine the structure of organic molecules for example, which provided information about chemical environments on the molecular scale, and imaging investigations that provide information about spatial location on a macroscopic scale.
So, how is it possible to be able to identify from whereabouts in the body the excited hydrogen nuclei emit their NMR signals?
In addition, a considerable strength of MRI is its exceptionally high sensitivity to changes in soft tissue. From what you’ve seen so far, a striking feature of an MR image is the level of detail that is available. Areas of high signal intensity appear white, while those of low signal intensity appear dark, and those in between are shades of grey.
How is this excellent contrast achieved? You will address these questions in the sections that follow but first you will briefly revise the relevant theoretical aspects of MRI.