Use 'Print preview' to check the number of pages and printer settings.
Print functionality varies between browsers.
Printable page generated Saturday, 6 June 2026, 3:51 PM
Communicable Diseases Module: 18. Leprosy Diagnosis
Study Session 18 Leprosy Diagnosis
Introduction
Leprosy is a mildly infectious chronic disease caused by the bacterium Mycobacterium leprae — a type of bacterium similar to the one that causes TB. After entering the body, the bacteria grow very slowly and usually affect the peripheral nerves (nerves situated close to the body surface). However, as you will shortly learn, leprosy bacteria can have an influence on other organs of the body, such as the skin and eyes.
Leprosy patients have to deal with stigma and discrimination associated with the disease – feelings of shame or disgrace about the condition and unfair treatment from others. Leprosy patients are often referred to as lepers, but nowadays this is not acceptable; you should refer to them as people with leprosy or leprosy patients. Leprosy is curable with multidrug therapy (MDT), treatment using combinations of anti-leprosy drugs. You will learn all about it in Study Session 19. MDT kills the bacteria responsible and stops the spread of the disease. Early detection and treatment will prevent disabilities.
In this study session, you will learn how to identify a leprosy ‘suspect’ and confirm a leprosy patient. In addition, you will learn how leprosy affects the body and how you can provide support for people living with leprosy. The knowledge and skills you gain will enable you to provide information to the community about leprosy. You will also be able to advise them on what they can do to prevent the spread of the disease, support patients during treatment and help to reduce stigma and discrimination suffered by persons affected by leprosy.
Learning Outcomes for Study Session 18
When you have studied this session, you should be able to:
18.1 Define and use correctly all of the key words printed in bold. (SAQs 18.2 and 18.3)
18.2 Describe the burden of leprosy in the world, Africa and Ethiopia. (SAQ 18.2)
18.3 Describe the mode of transmission of leprosy and how the disease is treated. (SAQ 18.3)
18.4 Explain how you would identify a person with suspected leprosy and diagnose the condition. (SAQs 18.1 and 18.4)
18.1 Leprosy and its control
18.1.1 What is leprosy?
In Study Session 19 you will also learn about paucibacillary leprosy patients, i.e. those who have few bacteria in their body. Pauci is the Latin word for ‘few’.
The sources of infection are untreated multibacillary leprosy patients – patients that have a large number of leprosy bacteria lodged in their body, especially inside the breathing tubes leading to the throat, mouth and nose.
Leprosy affects all age groups and both sexes, with the most affected being the 15–45 years age-group. In the majority of persons infected with leprosy bacteria, the body’s natural immunity is able to kill the bacteria. Only about 5% of individuals infected will develop the disease during their lifetime. Because the bacteria grow very slowly in the body, the incubation period varies from six months to 20 years. As the condition develops, the immune system of the body shows a number of inflammatory responses (called leprosy reactions, which you will learn more about in Study Session 19), which can come about in both treated and untreated patients. Damage to nerves is one commonly-seen reaction, including those that control the function of the hands, feet and eyes, and inflammation of the skin is another.
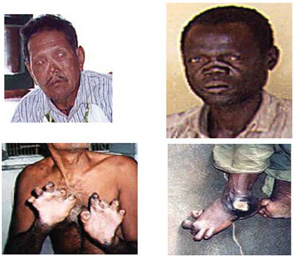
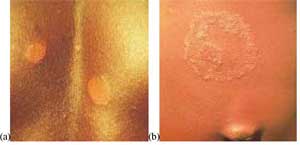
If the disease is untreated, leprosy leads to severe loss of function of organs – one or more disabilities, such as loss of fingers/toes, disfigurement of the nose and blindness (see Figure 18.1).
18.1.2 How can leprosy be controlled?
Access to leprosy information, diagnosis and treatment with MDT remain key elements in the strategy to eliminate the disease as a public health problem (see Box 18.1). Elimination is defined as reaching a prevalence rate of less than one leprosy case per 10,000 population.
Prevalence refers to the total number of cases existing at a given time.
Box 18.1 Leprosy control measures
- Early case finding of infectious persons.
- Adequate treatment using combination of anti-leprosy drugs, multidrug therapy (MDT) and support for all leprosy patients.
- Public education about early signs and symptoms of leprosy, control measures and action against stigma and discrimination.
18.2 Burden of leprosy in the world
Leprosy once affected every continent and left behind a terrifying image of mutilation, rejection and exclusion from society. But what is encouraging is that leprosy is a now a communicable disease ‘in retreat’. Of the 122 countries where it was considered to be a public health problem in 1985, in 119 of them, including Ethiopia, the disease has been eliminated in recent years.
In Ethiopia, 5,004 new cases of the disease were reported between the last quarter of 2007 and the third quarter of 2008 (European calendar), with the lowest number (seven cases) reported by Harar region and the highest number (2,610 cases) reported by Oromia region. Although Ethiopia has attained a leprosy elimination level of 0.57 cases per 10,000 population nationally, over the last few years the number of new child cases, and the number of new cases detected with disabilities of the type shown in Figure 18.1, are seen as unacceptably high by WHO standards. Rates at this level usually indicate continuing transmission of leprosy bacteria in the affected communities.
18.3 Transmission, identification and diagnosis
The exact route of transmission for leprosy is still uncertain at the present time. However, the inside lining of the nose and the mouth is thought to be the main route through which the leprosy bacteria enter the human body – in other words, the main portal of entry. When an untreated leprosy patient coughs or sneezes, the droplets of mucus containing the leprosy bacteria are expelled into the air and can be inhaled by a susceptible person.
Suspecting and then diagnosing someone with leprosy is called case finding. The next section explains how you can do this in your community.
18.3.1 Case finding
The main purposes of case finding are to:
- Identify the sources of infection in the community
- Diagnose and cure leprosy cases before irreversible nerve damage and disability occur.
There are two general strategies for case finding:
Passive case finding: where you ask about, or observe, symptoms and signs of leprosy when individuals attend the health facility or meet you in your community work.
Intensified/active case finding: where you examine all household contacts of a leprosy patient to identify leprosy cases early.
Whenever you are in doubt whether an individual has leprosy or not, encourage and refer such a person to the nearest health facility capable of diagnosing leprosy.
18.3.2 Diagnosing leprosy
Diagnosis of leprosy is most commonly based on the clinical features. The signs and symptoms will be easy for you to look for and observe after a short period of training, based on the descriptions in this section. In rare instances, laboratory and other investigations are necessary to confirm a diagnosis of leprosy. An individual should be regarded as having leprosy if one or both of the following very significant cardinal signs are present:
Doctors often call key signs such as these cardinal signs; the term can be applied to the key signs of any disease or health condition.
- skin lesion: an area of skin with definite loss of sensation (lack of feeling), with or without thickened nerves (we will explain about such nerves shortly);
- positive skin smears: in a small proportion of cases, leprosy bacteria may be seen in the smears taken from the affected skin when examined under a microscope.
Other symptoms and signs of leprosy are:
- Numbness or tingling of the hands and/or the feet
- Weakness of eyelids, hands or feet (tests for muscle weakness are described later)
- Painful and/or tender nerves
- Burning sensation in the skin
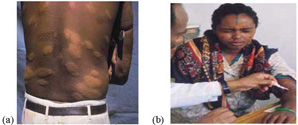
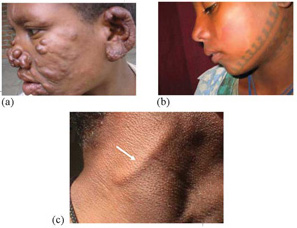
- Painless swelling or lumps in the face and earlobes (see Figure 18.2a)
- Painless wounds or burns on the hands or feet
- Loss of eyebrows and or eyelashes.
The skin lesion can be single or multiple, usually less pigmented than the surrounding normal skin (see Figure 18.2b). Sometimes the lesion may be reddish or copper-coloured. The variety of skin lesions which may be commonly seen include macules (which are flat), papules (raised), and nodules.
Features of the skin that are not indicative of leprosy
Skin patches:
- that are birth marks
- where there is normal feeling
- that itch
- that are white, black or dark red
- with scaling
- that appear or disappear suddenly and spread fast.
If you are not sure about the cause of the skin lesion, you should refer to a clinician.
Thickened nerves (see Figure 18.2c) constitute another feature of leprosy. These occur mainly on peripheral nerve trunks, which are nerve bundles close to body surface. Nerve thickening is often accompanied by other signs of damage, such as a loss of sensation in the skin and weakness of muscles supplied by the affected nerve. Nerve thickening by itself, without sensory loss and/or muscle weakness is usually not a reliable sign of leprosy.
18.3.3 What to do if you suspect leprosy
An individual may present with skin lesions or symptoms suggestive of nerve damage, but the cardinal signs may be absent or doubtful; such a person should be called a leprosy suspect in the absence of any immediately obvious alternative diagnosis. Such individuals should be informed about the basic facts of leprosy and advised to see you again if their symptoms persist for more than six months, or if at any time the symptoms worsen. In these circumstances, suspect cases should be referred to health facilities with more capacities for diagnosing leprosy. Use Box 18.2 to help you take a history from a person you suspect may have leprosy.
Box 18.2 Checklist for history-taking from leprosy suspects
Make the individual comfortable, and ask for the name, age, sex, address, etc. Take a history of the present illness by asking:
- How long has the skin patch been there? How did it start? Has it changed? (Leprosy patches usually appear slowly.)
- Do the patches itch? Is there pain? (Leprosy patches do not itch and are not usually painful.)
- Does the person have unusual sensations in the hands or feet, such as numbness, tingling or burning feeling? (Unusual sensation in the hands or feet, chronic ulcers and eye problems are all signs of leprosy.)
- The nature of the first lesion or symptom, including the time (when) and site (where) the lesion first appeared and the subsequent development of the disease.
- Did the person have any treatment for leprosy in the past? If yes, which type, and for how long?
- Is there any other person in the family with similar symptoms or signs, or who has been treated or is being treated for leprosy?
18.4 Examining the person with suspected leprosy
In this section, we will teach you how to examine someone whom you suspect may have leprosy.
18.4.1 Checklist for examination of the skin
- Ask the person to remove all his/her clothes/garments.
- Examine the skin under adequate light and ensure privacy for the person to feel at ease.
- Examine the person systematically from the head to toe. Examine the front side of the body first and then examine from the back.
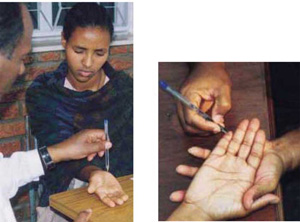
- Examine, count and record the presence of skin lesions; look for pale or reddish discoloration of the skin (see Figure 18.3a).
- Examine for loss of sensation in the skin lesions by rolling the end of a wisp of cotton into a fine point and explaining to the person the purpose of the test is for him/her to point to the spot where he/she feels the touch of the cotton wool. Then touch the skin patch lightly until the cotton wisp bends, first of all while the person has his/her eyes fully open and wait for the reaction of the person to the touch.
- Now repeat the test when the person’s eyes are closed (see Figure 18.3b). If the person points away from where the skin is tested, the skin patch has no sensation and the suspect is probably a case of leprosy. If he/she points accurately to the spot or near the spot where you touched the skin patch with the cotton wisp, and if there are no other signs of the disease, they probably don’t have leprosy.
- Look for loss of eyebrows and/or eyelashes. These are signs of leprosy when they are not due to deliberate removal for cosmetic reasons.
18.4.2 Examination/palpation of the peripheral nerves
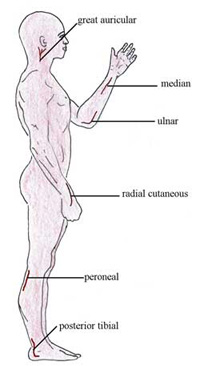
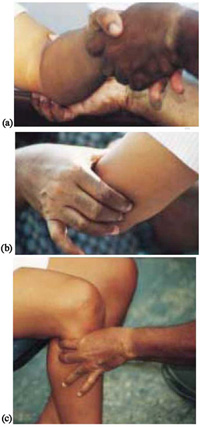
The examination of the nerves is an important part of examination of a person suspected of leprosy. The two most commonly affected nerves in leprosy patients are the ulnar and peroneal nerves, and can be felt quite easily (see Figure 18.4). Palpate (‘feel’) the nerves shown in Figure 18.4, starting from the head to the feet; do so following the technique described in Box 18.3 and the photos in Figure 18.5.
Box 18.3 Palpating the nerves in a person with suspected leprosy
- Peripheral nerves are examined for enlargement or thickening and for tenderness
- When palpating a nerve always use two or three fingers (see Figure 18.5)
- The nerve should be rolled over the surface of the underlying bone
- The same nerve on the left and right sides of the body must always be compared.
18.4.3 Examination of hands and feet for loss of sensation
The sensation test (ST) is an examination to test sensation in the hands, served by the ulnar and median nerves, and also in the feet.
Your aim is to compare the sensation in the little finger with that of the thumb, and the sensation of one hand with the other, to see if there is any difference. Then repeat the test on the feet. If you have done these tests on the same person previously, compare the findings with those shown on any earlier records.
Before you start the test, make a note of any wounds or cracks or bone loss on the hands/feet.
First, support the person’s hand or foot so that fingers/toes are well supported to prevent joint movement during the test (see Figure 18.6).
Make sure you get hold of a Record Card for a leprosy patient and spend time looking at it. On it, you can record all the important details that relate to the patient, such as the skin lesions you can see, the results of palpation and the outcomes of the voluntary muscle tests you will perform.
Explain the test to the person and rehearse it with him/her with eyes open. Then perform the test (described below) with the person’s eyes closed. A book or another suitable object can be held in front of the eyes, so that the person cannot see.
Use the point of a ballpoint pen (biro) to dent the person’s skin to a depth of 1–2 mm at the four test points (dots) on the palm of the hand (Figure 18.7a and c).
Do not allow the pen tip to slide across the skin – press it straight down and lift it straight up again. Ask the person to point to the exact site whenever he/she feels the pressure from the pen – first the ‘rehearsal’ with eyes open, and then with eyes closed. The test points should be pressed at irregular intervals and each test point should be chosen at random – don’t test them in a fixed pattern, so that the person can’t guess where you will test next. Avoid repetitive testing at any one test point. Provide time for a response: older people may need a little more time to respond.
Repeat this process at four test points (dots) on the feet (Figure 18.7b and d).
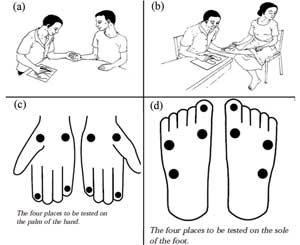
Record the results in a leprosy patient record card, or mark the results on suitable diagrams of the type shown in Figure 18.7(c) and (d). On a record card, mark ✓ if the person feels the pressure at a particular test point, or X if he/she does not feel it.
Where possible, compare your findings with those shown on any earlier records – look for differences over time. Make sure that the change is real and not simply a result of one or other of the tests having been recorded in a careless and therefore inaccurate way.
18.5 Examining the eyes and eyelids
18.5.1 Testing for corneal sensation
The surface of the eye is called the cornea. It is very sensitive to being touched in a healthy person, who will blink if something touches the cornea. Corneal sensitivity is lost in a person with leprosy. Observe the person’s blink when talking to him/her. If the blink is normal, corneal sensation will be normal and there is no need for the test. If there is no blink, the eye is at risk.
Look at Figure 18.8 and Box 18.4 to see how the corneal sensation test is done.
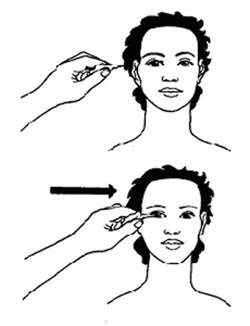
Box 18.4 Steps in the corneal sensation test
- You should wash your hands before testing. Then make a point out of a wisp of cotton wool and explain the test to the person.
- The person should look to the opposite side and upwards, away from you.
- You should:
- Approach from the side
- Touch the edge of the cornea with the cotton wisp
- Observe the person’s reaction.
- Take note or record on the person’s record card: Write yes, if he/she blinks, which means corneal sensation is normal; write No if sensation is absent (no blink).
18.5.2 Eyelid closure to test facial nerve function
Ask the person to close his/her eyes as in sleep. A lid gap may be a sign of leprosy. You can also test the strength of the eyelid muscles by asking the person to close his/her eyes tightly and to resist your gentle efforts to part the eye lids. Record full eye closure with full strength as ‘S’ = Strong. This type of test is known as a voluntary muscle test (or VMT).
Next we will look at somewhat similar VMT tests on the hands and feet of a person you suspect may have leprosy.
18.6 Examination of hands and feet for muscle weakness
By testing the strength of the voluntary muscles (which means the muscles we can move at will, e.g. in our arms and legs), you can find out if the person’s nerve function is normal, or has been weakened or paralysed by leprosy. The findings are recorded as follows:
- Paralysed (P): the muscle has lost all strength and cannot produce any movement;
- Weak (W): there is some movement, but muscle strength is reduced;
- Strong (S): the muscle strength is normal.
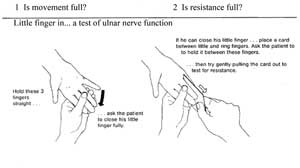
18.6.1 ‘Little finger out’ test of ulnar nerve function
The muscles that move the little finger are activated by the ulnar nerve. Keep the person’s hand flat, palm level and facing the ceiling during this test, as shown in Figure 18.9.
As shown in the left of Figure 18.9, first ask the patient to move his little finger all the way in (touching the side of the ring finger) and all the way out until he can make no further movement at the joint). Is the movement full? How large is the gap between the little finger and the ring finger?
If movement is full, ask the patient to hold his little finger out fully while you give resistance to the outward movement at the base of the finger by pushing it in. Resistance can also be tested in the way shown in the diagram to the right of Figure 18.9. Record your findings.
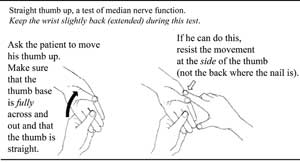
18.6.2 ‘Thumb up’ test of median nerve function
The muscles that move the thumb are activated by the median nerve. Keep the hand flat, palm level and facing the ceiling and the wrist slightly extended backwards during this test, as shown in Figure 18.10.
First, ask the patient to bring his thumb up in front of the index finger but as far away from it as possible, in the way shown to the left of Figure 18.10. Focus your attention on the degree of movement that is possible at the base of the thumb rather than the tip. Can the patient achieve this starting position for the test? Is movement full?
Now test the strength of this movement as shown to the right of Figure 18.10 – seeing if the individual can resist the pressure you apply to the side of the thumb. Ask the patient to stare at you during the test, while you try to push his thumb out and across, away from his little finger.
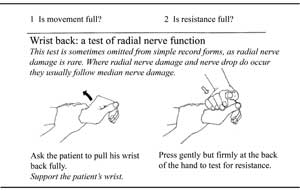
18.6.3 ‘Wrist back’ test of radial nerve function
Study Figure 18.11, which shows you how to perform the test for radial nerve function. Again you are testing for how much resistance there is to pressure you apply, this time to the individual’s raised hand, while you support the wrist.
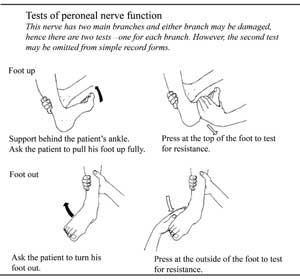
18.6.4 ‘Foot up’ test of peroneal nerve function
The movement of the foot is due to muscles activated by the peroneal nerve and the test for muscle power in this case is shown in Figure 18.12. You apply pressure to the top of the raised foot by trying to push it down. Can the person still lift up the foot against your pressure? A second test of this type is shown at the bottom of Figure 18.12.
It is useful to have ended the main part of this study session by describing these different tests of voluntary muscles. Along with palpation, these are very useful clinical tests for detecting the type of nerve damage typical of leprosy and therefore it is important that you know about them.
Summary of Study Session 18
- Leprosy is a chronic infectious disease affecting mainly the skin and peripheral nerves. Its incubation period is between six months and 20 years.
- Leprosy does not kill, but it can disfigure the sufferers. When discovered early and treated promptly it is fully curable and no disabilities will arise.
- Cardinal symptoms and signs of leprosy are skin lesions, with a lack of sensation, and leprosy bacteria seen in positive skin smears. Thickened nerves are commonly associated with the disease, but they are not always present. Additional signs and symptoms include weakness of eyelids, hands or feet and painful and/or tender nerves.
- Leprosy bacteria are expelled into the air when untreated leprosy patients cough or sneeze and can be inhaled by a susceptible person.
- Diagnosis of leprosy is most usually based on the clinical features. Most often affected areas are the skin, peripheral nerves and the eyes. Palpation of nerves and the testing of a range of voluntary muscles, for example those associated with the hands and feet, are key methods of detecting nerve damage to aid diagnosis. So is testing for reduced skin and corneal sensitivity.
Self-Assessment Questions (SAQs) for Study Session 18
Now that you have completed this study session, you can assess how well you have achieved its Learning Outcomes by answering these questions. Write your answers in your Study Diary and discuss them with your Tutor at the next Study Support Meeting. You can check your answers with the Notes on the Self-Assessment Questions at the end of this Module.
SAQ 18.1 (tests Learning Outcome 18.4)
Look at the skin lesions in Figure 18.13(a) and (b). Identify, with reasons, which one shows the signs of leprosy. Keep in mind that in Figure 18.13(a) there is loss of sensation, but no loss of sensation or nerve enlargement in Figure 18.13(b).
Answer
Figure 18.13(a) is a photo from a leprosy patient, because it shows a skin lesion with accompanying loss of sensation. If you are told there is no loss of sensation or signs of nerve enlargement (Figure 18.13b) you should not suspect leprosy.
SAQ 18.2 (tests Learning Outcome 18.2)
Is it right to say that leprosy has been eliminated in Ethiopia and that as a Health Extension Practitioner you therefore don’t need to be looking out for cases of the disease?
Answer
Leprosy is understood to be eliminated in countries where fewer than 1 case for every 10,000 population is identified; the rate in Ethiopia is 0.57 cases per 10,000 population, so it has been eliminated in Ethiopia. However, this does not mean there are never any cases. So, as a HEP, you need always to be looking out for leprosy suspects to help reduce the incidence in Ethiopia even further.
SAQ 18.3 (tests Learning Outcomes 18.1 and 18.3)
Which of the following statements is false? In each case, explain what is incorrect.
A The inside lining of the nose and the skin are major portals of entry of leprosy bacteria.
B MDT has not proved successful in the fight against leprosy.
C MDT treatment helps nerves and organs damaged as a result of leprosy to start functioning again normally.
D If leprosy is untreated, organs such as the eyes can become damaged and fingers and toes can be lost.
E Case finding is essential to the task of reducing the prevalence of leprosy.
F Case finding involves only the process of carefully looking at individuals attending your health facility for signs of leprosy.
Answer
A is true: as you will have learned early in Section 18.3.
B is false: MDT has resulted in the elimination of leprosy in many countries.
C is false: MDT can stop the progress of the disease, but it cannot restore damaged nerves.
D is true: as you see in Figure 18.1.
E is true: case finding is a very important way of reducing the incidence of the disease.
F is false: this is only one part of case finding. Also involved (Section 18.3.1) is active case finding, where contacts of those with leprosy are examined.
SAQ 18.4 (tests Learning Outcome 18.4)
- a.Someone at your health facility presents to you with weakness of both hands. Should you suspect he has leprosy or not? What should you do to confirm your suspicion?
- b.Another individual explains to you that she has some areas of skin that are sore and that are very itchy. When you test her, she has normal responses to VMT. Do you suspect leprosy or not?
Answer
- a.You should suspect leprosy because weakness of the hands is a sign of leprosy. You should take his history according to the guidelines in Box 18.2 and examine any skin patch for loss of sensation. In addition, you should do sensitivity tests (ST) and voluntary muscle tests (VMT) on both wrists.
- b.Skin signs such as these do not suggest leprosy and the fact that the patient’s responses to VMT are normal is further evidence that the disease is not present.