Use 'Print preview' to check the number of pages and printer settings.
Print functionality varies between browsers.
Printable page generated Saturday, 6 June 2026, 2:52 PM
Communicable Diseases Module: 21. Opportunistic Infections and WHO HIV Clinical Staging
Study Session 21 Opportunistic Infections and WHO HIV Clinical Staging
Introduction
In this study session, you will be introduced to the most common opportunistic infections and diseases that result from the decreased immunity observed in people living with HIV (PLHIV). Knowledge of the signs and symptoms of opportunistic infections will enable you to easily recognise them in patients in your healthcare and community settings.
In addition, you will learn how to categorise HIV patients into the four stages recognised by the World Health Organization (WHO). The WHO clinical staging system has been adapted by the Ethiopian Federal Ministry of Health (FMOH) to include a list of the common infections and diseases occurring in PLHIV in an Ethiopian context. After studying this session, you should be able to group patients living with HIV into the four different WHO clinical stages of HIV/AIDS. Staging will help you to differentiate patients who need urgent clinical assessment and referral to the nearest health facility to receive standardised care and treatment interventions.
Lastly, this session describes the standard chemoprophylactic treatments for opportunistic infections offered to PLHIV. You are not expected to provide prophylactic treatments at your setting, but you should be familiar with the commonly used prophylactic drugs so that you can make community follow-ups for PLHIV.
Chemoprophylactic treatments (or chemoprophylaxis) refers to drug-based medication taken to prevent opportunistic infections from developing.
Learning Outcomes for Study Session 21
When you have studied this session, you should be able to:
21.1 Define and use correctly all of the key words printed in bold. (SAQ 21.1)
21.2 Explain why opportunistic infections occur more frequently in PLHIV. (SAQs 21.1 and 21.2)
21.3 Identify common opportunistic infections in PLHIV and use this knowledge to help patients seek healthcare promptly. (SAQs 21.2 and 21.3)
21.4 Describe WHO HIV clinical staging and classify patients into the appropriate clinical stages. (SAQ 21.3)
21.5 Explain the use of chemoprophylactic treatments to prevent opportunistic infections in PLHIV. (SAQs 21.1 and 21.4)
21.1 What are opportunistic infections?
An opportunistic infection is an infection caused by harmful infectious agents, or pathogens (bacteria, viruses, fungi, parasites or protozoa), that usually do not cause disease in a healthy person, i.e. one with an immune system whose function is not impaired. Opportunistic infections observed in PLHIV include a wide range of diseases, from minor ailments like chronic skin itching to severe diseases such as tuberculosis (TB).
You may be asking yourself why PLHIV are so susceptible to opportunistic infections compared to an uninfected person. Remember from Study Session 20 that the immune system in HIV-infected people becomes progressively weakened. A weak immune system presents an ‘opportunity’ for pathogens to cause an infection. Thus, PLHIV can be infected by pathogens causing opportunistic infections more easily than HIV-negative immune-competent people, because HIV damages the function of the immune system.
An immune-competent person is an individual whose immune system is healthy and functions normally.
There are several important issues that we need to consider here before we describe the possible opportunistic infections that PLHIV may present (Section 21.4).
First, serious opportunistic infections usually develop 5 to 10 years following infection with HIV. You should expect a person who is infected with HIV to show minor and/or mild episodes of opportunistic infections during the early period of the disease. However, untreated PLHIV will increasingly acquire more serious infections as they progress to AIDS, mainly due to the gradual deterioration of their immune system.
Based on your previous study of the role of the immune system in the progression to AIDS, why do you think serious opportunistic infections do not develop until later in the course of the disease?
As you learnt in Section 20.2, during the first few years of HIV infection, a person’s immune system is weakened, but it still functions quite well. Thus, it is able to fight off most infectious agents for some time.
Indeed, an HIV-infected person may have no symptoms during the first stages of HIV infection. Sometimes minor symptoms like skin diseases, a little loss of weight, or repeated sinusitis (inflammation of the nasal sinuses and nasal passages) may be present, and this is indicative of a slightly weakened immune system. The most important information for you to remember here is that the immune system has to be compromised beyond a certain level for serious opportunistic infections to arise in PLHIV.
Nasal means associated with the nose and its related structures.
Secondly, the onset of opportunistic infections will be different for each person living with HIV, and will depend on many factors such as nutritional status, exposure to pathogens, individual level of immunity, etc. These factors differ from person to person. Hence, in some cases PLHIV may progress to AIDS rapidly, while in others it may take longer for serious opportunistic infections to arise.
Thirdly, not all PLHIV develop the same opportunistic infections. The opportunistic infections developed by a person living with HIV depend primarily on the pathogens they have been exposed to. Although progression to AIDS from HIV infection follows a somewhat stereotyped series of different clinical stages, each individual patient has a unique pattern of progression through them (i.e. they present with different opportunistic infections at each stage).
Finally, we also need to briefly consider opportunistic infections in the context of HIV-infected children (Study Session 28). Indeed, opportunistic infections appear earlier in children than in adults. In the absence of treatment, around half of HIV-infected children die by the age of two years, due to serious opportunistic infections and diseases. This is because children have immature immune systems, so their immune system becomes weakened faster than in adults, who already have a well-developed immune system before they get HIV.
In addition, other factors that influence the onset of opportunistic infections, such as exposure to pathogens and malnutrition, are more common problems in children than in adults. You will be learning about HIV in children in detail in Study Session 28. Here, we will be focusing on opportunistic infections occurring in adults.
21.2 Why are opportunistic infections common in PLHIV?
In Study Session 20, you learned that CD4 lymphocytes (also known as CD4 cells) are a type of white blood cell with important functions in immunity. In this study session, we will use the simpler term, CD4 cells.
What is the function of CD4 cells in the immune system?
CD4 cells help to activate other white blood cells in the immune system, in the defence of the body against invasion by pathogens (Section 20.2.3).
Indeed, a reduced number of CD4 cells results in an impaired immune system. The lower the number of CD4 cells, the more impaired the immune system will be. Remember that HIV weakens the immune system precisely by infecting (and ultimately destroying) CD4 cells. Hence, the CD4 count (i.e. the number of CD4 cells in a specified volume of blood) is a good indicator of the ‘health’ of the immune system in PLHIV.
The CD4 counts of uninfected people usually fall between 800 and 1500 cells/mm³. At the early stages of the disease, HIV-infected people with immune systems that are functioning adequately have CD4 counts between 450 and 1500 cells/mm³.
The concentration of cells in the blood is usually expressed as the number of cells per cubic millimeter (cells/mm3), which is the same volume of blood as a millilitre (ml).
However, the risk of acquiring opportunistic infections increases proportionally to the decline in CD4 counts observed as the disease progresses. In other words, if the CD4 count falls below a certain limit, the immune system is unable to cope with invading pathogens and opportunistic infections become more frequent. In general, the following thresholds concerning CD4 counts are observed in adults and adolescents:
- When the CD4 count has decreased below 450 cells/mm³, a person living with HIV will start to acquire some mild or moderate opportunistic infections.
- When the CD4 count has decreased below 200 cells/mm³, a person living with HIV is highly likely to acquire severe opportunistic infections. It is at this stage that a person living with HIV is considered to have AIDS.
Based on your previous studies, why are CD4 counts determined in the blood, and not in other tissues and/or fluids such as urine?
CD4 cells reside primarily (although not exclusively) in the blood, where they are most likely to encounter invading pathogens (Section 20.2.2 and Figure 20.3).
21.3 WHO HIV clinical stages in adults and adolescents
The WHO HIV clinical staging system is a staging system developed for PLHIV to help healthcare providers, such as Health Extension Practitioners, estimate the degree of immune deficiency that an HIV patient presents. Staging means categorising the patient clinically into one of the four WHO HIV stages. It is useful to know these stages because it enables you clinically to identify patients with mild and severe diseases associated with HIV.
A PLHIV in WHO clinical stage 1 usually does not have a serious immune deficiency, and shows no signs of opportunistic infections (i.e. they are asymptomatic — no symptoms). A patient in WHO clinical stage 2 also does not have a serious immune deficiency, but usually shows signs of mild opportunistic infections. Patients in stage 3 or 4 usually have a severe immune deficiency, and show signs of moderate and severe opportunistic infections respectively. Stage 4 is considered to be AIDS.
Would you expect a person living with HIV in stage 2 to have a higher or lower CD4 cell count than a person living with HIV in stage 4 of the WHO clinical staging system? Why?
As the immune status of a person living with HIV becomes weaker, the HIV clinical stage gets higher. Therefore, stage 2 patients have stronger immunity than stage 4 patients, and the CD4 cell count is higher in stage 2 than in stage 4 patients.
We will discuss the WHO paediatric staging for children with HIV in Study Session 28.
Table 21.1 summarises the WHO HIV clinical staging for adults and adolescents adapted for the Ethiopian primary healthcare setting. Most opportunistic infections common in PLHIV will be explained in detail in Section 21.4, but for now you should use Table 21.1 as a reference to give you an idea of how clinical staging of PLHIV is implemented. Some opportunistic conditions may be diagnosed by a health worker in a health centre, whereas others need a diagnosis by doctors or health officers working at regional hospitals (marked with an asterisk in Table 21.1). These patients should be referred for appropriate diagnosis and treatment. Note that if the patient has clinical conditions that fall into more than one WHO clinical stage, the patient will be placed in the highest WHO clinical stage that fits the symptoms.
However, staging of a person living with HIV is not a permanent fixture. For example, a PLHIV who has been successfully treated for, and recovered from, Pneumocystis pneumonia may be downgraded from stage 4 to stage 3 if no other severe conditions are present.
Some opportunistic conditions may be easily identified by Health Extension Practitioners (HEPs), and these will be explained in detail in Section 21.4. For other opportunistic infections you may come across in PLHIV, a short description has been included in the table. You are not expected to memorise the details of these latter conditions. All conditions that require a diagnosis by doctors or health officers working at regional hospitals are marked with an asterisk.
Stage 1 Asymptomatic | Stage 2 Mild disease |
No symptoms or only persistent generalised lymphadenopathy (PGL) (Section 21.4.1) | Weight loss 5–10% Skin problems (Section 21.4.2): seborrhoea prurigo (PPE) herpes zoster Mouth/throat problems (Section 21.4.3): angular chelitis recurrent mouth ulcers Recurrent upper respiratory infections (repeated throat infections, sinusitis, or ear infections) |
Stage 3 Moderate disease | Stage 4 Severe disease (AIDS) |
Weight loss greater than 10% Mouth/throat problems (Section 21.4.3): oral thrush oral hairy leukoplakia acute necrotising ulcerative gingivitis/periodontitis (severe gum disease accompanied by ulcers) Diarrhoea (for more than 1 month; sometimes intermittent) Unexplained fever (for more than 1 month; sometimes intermittent) Severe bacterial infections (e.g. pneumonia, muscle infection): pulmonary TB (Section 21.4.4) TB lymphadenopathy (chronic swelling of lymph nodes around the lungs) | HIV wasting syndrome (Section 21.4.5) Oesophageal thrush (Section 21.4.3) Herpes simplex ulcerations (large and chronic painful wounds on the genitals and/or anus for more than 1 month) Lymphoma* (cancer of the immune system) Kaposi’s sarcoma* (dark lesions on the skin and/or mouth, eye, lungs, intestines) Invasive cervical cancer* (cancer of the female reproductive system) Pneumocystis pneumonia* (severe pneumonia with shortness of breath on exertion and dry cough) Extrapulmonary TB* (TB in tissues other than lungs, e.g. bone) Cryptococcal meningitis* (meningitis caused by a fungus which can present without neck stiffness) Toxoplasma brain abscess* (infection of the brain by a parasite) Visceral leishmaniasis* (infection of internal organs by a protozoan) HIV encephalopathy* (neurological impairment). |
21.4 Common opportunistic clinical manifestations in people with HIV
In this section, we will be describing the clinical signs and symptoms associated with common opportunistic clinical manifestations that you may encounter in PLHIV during community visits, or at your health post. Where possible, we have included photographs showing typical clinical manifestations of an opportunistic disease in a PLHIV, so that you become familiar with them.
Identifying opportunistic infections and diseases will help your work in the context of PLHIV in two ways. First, you may be able to categorise patients in one of the four stages of the WHO HIV clinical staging. You will then be able to refer them to the nearest health centre for comprehensive HIV services, such as cotrimoxazole chemoprophylaxis (used for prevention of opportunistic infections, explained in Section 21.6), and for specific treatments for HIV/AIDS. In some cases, you will need to refer the person living with HIV urgently, whereas in others you will just need to reassure the patient, and/or treat minor ailments. Note that all conditions described below should be referred to the nearest health centre if they are clinical stage 2 and above, with increasing urgency the higher the WHO clinical stage.
Secondly, if staging has been carried out by a health worker at a health centre or hospital, you will be able to appreciate at what stage of the disease a person living with HIV is, and provide the best possible care for that patient.
21.4.1 Persistent generalised lymphadenopathy (PGL)
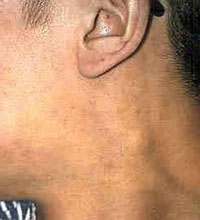
Persistent generalised lymphadenopathy (PGL) is a chronic swelling of the lymph nodes in at least two areas of the body outside the groins, which lasts three months or longer. PGL is common in the neck and underarm areas, as shown in Figure 21.1. Up to half of PLHIV show PGL at one point during disease progression. In some instances, PGL is present even if they are in the early stages of the disease (asymptomatic stage), i.e. when the patient has relatively good immunity. PGL results from a reaction of the patient’s immune system against the virus entering the body and establishing a chronic infection. You should reassure a person living with HIV that this sign does not affect their overall health.
21.4.2 Skin problems
Skin problems are common in HIV/AIDS patients. You need to differentiate minor skin problems from other severe opportunistic diseases that also present with skin manifestations, but need urgent referral. For instance, fungal infections in the blood and internal organs such as cryptococcosis (Stage 4; see Table 21.1), may also result in nodular skin lesions. The following minor skin problems are indicative of WHO clinical stage 2, and you should refer PLHIV presenting these to the nearest health centre for treatment.
Itching skin rash may be due to the following two conditions:
Seborrhoea is a scaly skin rash that usually appears on the edge between face and hair, on the side of the nose, or on the chest. The areas with the rash often contain greasy or oily scales, and are surrounded by some redness of the skin (Figure 21.2).

Prurigo (Pruritic Papular Eruptions, PPE) is an itchy skin eruption on the arms and legs. Often it has small papules (small, solid and usually inflammatory elevations of the skin) and scratch marks. Once cleared, papules may leave dark spots with light centres (Figure 21.3).

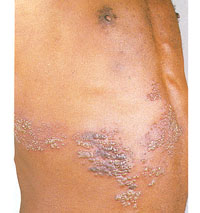
Herpes zoster (‘almaz bale chira’ in Amharic) is a painful blistering skin rash caused by the herpes zoster virus (also known as varicella zoster). It is characterised by vesicles (fluid-filled blisters formed in, or beneath, the skin) that appear in only one area on one side of the body, usually on the chest (Figure 21.4), but also on a leg, arm or one side of the face or the back. Vesicles then turn into lesions, and later into crusts that may become inflamed, and even infected. Vesicles usually heal in two to three weeks and they rarely reappear, but there is often scarring after healing. Note that vesicles are accompanied by intense shooting pain, and sometimes the pain may continue after the lesions heal.
21.4.3 Mouth, throat and oesophagus problems
Mouth and throat problems are also common in HIV patients. Mouth and throat problems include sores at the corners of the mouth, and fungal infections of the oral mucosa and the oesophagus (the tube that connects the mouth and throat to the stomach). These problems are indicative of different WHO clinical stages (2 to 4), and you should refer PLHIV presenting these to the nearest health centre, with a degree of urgency related to the specific stage.
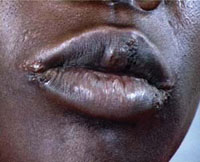
Angular chelitis: These are small chronic sores or cracks around the lips, often at the corners of the mouth (Figure 21.5). Angular chelitis occurs early in HIV infection, and is indicative of WHO clinical stage 2.
Recurrent mouth ulcers (aphtous ulcers): These are small sores or ulcers inside the mouth that appear repeatedly. Ulcers are painful, self-healing and can recur. They can also involve the gums and throat. Note that mouth ulcers are also common in people who are not HIV positive who, for example, have malnutrition. However, in PLHIV, the ulcers are usually severe, making food intake difficult.

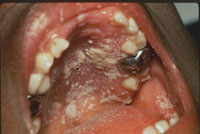
Oral thrush: Also known as oral candidiasis, this is an infection of the lining of the mouth caused by a fungus called candida (the same organism that causes oesophageal thrush which is decribed below, and vaginal candidiasis; see Study Session 31). Oral thrush is a sign of clinical stage 3, and is characterised by white patches (although at times they may appear red) that can be removed with an oral spatula (Figure 21.7).
Oesophageal thrush is a candida infection of the oesophagus. You can identify patients with oesophageal thrush by asking them whether they experience pain while swallowing. A patient who has white patches indicative of oral thrush, and who has severe pain on swallowing, may have oesophageal thrush. Oesophageal thrush is a serious infection, since it can prevent the patient from eating. The pain may be so intense that a patient is unable to swallow. Oesophageal thrush indicates a higher degree of immune suppression than oral thrush, and is a sign of clinical stage 4 (which requires an urgent referral to the nearest health centre).
Oral hairy leukoplakia appears as fine white patches (e.g. white vertical lines) on the side of the tongue, which are painless but cannot be removed. Oral hairy leukoplakia is different from oral thrush or oesophageal thrush in that it does not need to be treated. However, oral hairy leukoplakia (like oral thrush) is still a sign of clinical stage 3, and the patient should be referred to the health centre for health check-ups.
21.4.4 Pulmonary tuberculosis (PTB)
Pulmonary tuberculosis (PTB), that is, TB in the lungs, is extremely common in PLHIV. Remember from Study Session 13 that you should suspect pulmonary TB if a patient has a chronic cough for more than two weeks, whitish sputum, fever or sweating (often at night), loss of appetite, weight loss, and sometimes chest pain or spitting up blood. The presence of pulmonary TB in a person living with HIV indicates WHO HIV clinical stage 3. Note that extra-pulmonary TB (outside the lungs) is indicative of WHO clinical stage 4, and requires an urgent referral.
21.4.5 HIV wasting syndrome
A syndrome is actually not an opportunistic infection, but a clinical presentation in patients consisting of specific signs and symptoms.
Can you recall an example of a syndrome?
Acquired immunodeficiency syndrome, or AIDS.
As the disease progresses, the immune system of PLHIV is increasingly weakened, and this is associated with a gradual loss of weight. At WHO clinical stage 4, HIV wasting syndrome is characterised by an extreme loss of weight (more than 10%), associated with chronic fever and/or chronic diarrhoea. Patients presenting with HIV wasting syndrome require urgent clinical treatment and care, and should be urgently referred to the nearest health centre.
A 32-year-old person living with HIV comes to your health post with unexplained weight loss of 7 kg. His normal weight was 60 kg, but he doesn’t complain of other health problems. How do you explain his weight loss in terms of WHO HIV clinical staging?
Weight loss is one sign used in WHO HIV clinical staging. In this case, the patient has lost 7 kg, which is 11.6% (7 x 100/60) of his normal body weight. Losing more than 10% of normal body weight will immediately put him at WHO clinical stage 3. This patient might have other opportunistic infections that he is not aware of, and he needs to be referred to the health centre for further investigation.
21.5 Opportunistic infections and provider-initiated counselling and testing
You should be aware that only HIV-infected people can be categorised using the WHO clinical staging system. Occasionally, a person showing signs of opportunistic infections may not know their HIV status. If you suspect an HIV-related disease, you should offer them provider-initiated testing and counselling (Study Session 24). This is particularly recommended for individuals with PGL (persistent generalised lymphadenopathy), the most common clinical presentation that leads you to suspect HIV infection. Similarly, the presence of herpes zoster scars, or unexplained weight loss, should be indications for you to advise individuals with unknown HIV status (especially if they also show PGL) on provider-initiated HIV testing and counselling.
Makeda is a 23-year-old woman who has come to your health post for a consultation. She complains about swellings under her arms and on her neck. What would you advise Makeda?
First, you need to verify whether the swellings appear to be PGL. If so, PGL is a good reason for you to suspect HIV infection in this patient. You may need to ask Makeda if she knows her HIV status. If she is a person living with HIV, you should reassure her that PGL will not affect her health. If she does not know her HIV status, you should offer her provider-initiated counselling and testing (Study Session 24).
21.6 Prevention of opportunistic infections
It is very important to know about measures to reduce the risk of developing opportunistic infections in PLHIV, some of which can be fatal. Prevention is carried out by giving certain drugs to PLHIV on a daily basis, before they develop symptoms of the disease, in this case, opportunistic infections. As you learnt in Study Session 1, the use of drugs for the prevention of common infectious diseases is called chemoprophylaxis. Good prophylaxis is not expensive or complicated, but can increase the duration and quality of life of a person living with HIV.
Give one example of a chemoprophylactic drug used in prevention of an infectious disease, which you learned about in Part 2 of this Module.
Isoniazid is a chemoprophylatic drug used to prevent TB infection in children and PLHIV (Study Session 16).
The most commonly used prophylactic drug for HIV/AIDS is cotrimoxazole, a wide-spectrum antibiotic that targets the pathogens causing the most common opportunistic infections. These include pneumonia, brain abscess and chronic diarrhoea caused by protozoans, as well as by some bacterial infections. Note that you do not need to memorise these infections as they need to be diagnosed at a health centre or regional hospital. However, you will need to closely monitor patients on cotrimoxazole in your community on follow-up visits or consultations, in order to check whether they are taking their drugs correctly, and/or to refer them if they experience adverse side-effects.
21.6.1 Criteria for starting cotrimoxazole prophylaxis by adult PLHIV
All HIV-positive people at WHO clinical stages 2, 3, 4, or with a CD4 count less than 350 cells/mm³, should start cotrimoxazole prophylaxis. Patients should first be asked if they are allergic to sulfa-containing drugs like Fansidar — if they are, these patients should not be given cotrimoxazole.
Sulfa drugs are mainly antibiotics related to sulphonamide. Many PLHIV may develop adverse reactions to this class of drugs. Cotrimaxazole is a sulfa-containing drug.
The drug regimen for cotrimoxazole prophylaxis is two 480 mg tablets, or one 960 mg tablet daily. Note that you are not expected to either prescribe or refill prophylactic drugs. However, information about the criteria for cotrimoxazole prophylaxis will enable you to identify patients who need prophylaxis, and to refer them to the appropriate health centre.
21.6.2 Duration of cotrimoxazole prophylaxis for adult PLHIV
If a person living with HIV has no access to HIV treatment, cotrimoxazole prophylaxis should be taken for the rest of the patient’s life. If the patient has access to antiretroviral therapy (ART) for HIV (Study Session 22), cotrimoxazole prophylaxis should be stopped when the CD4 count has increased to 350 cells/mm³ and remains above that level for at least six months. Note that only the healthcare provider at the health centre should stop the cotrimoxazole prophylaxis — you are not expected to stop cotrimoxazole prophylaxis.
21.6.3 Side-effects of cotrimoxazole prophylaxis
If a patient on cotrimoxazole experiences adverse side-effects, medication should be stopped and the patient should be referred to the health centre. Common side-effects include skin rashes involving the eyes or mucous membranes inside the mouth, yellow discolouration of the eyes, and paleness of the conjunctiva (the mucous membrane that lines the exposed portion of the eyeball and inner surface of the eyelids), due to anaemia and tendency to bleed easily.
21.6.4 Monitoring cotrimoxazole prophylaxis
As already mentioned, cotrimoxazole prophylaxis is prescribed by health workers at the health centre or regional hospital. You are not expected to prescribe the drug, but once these patients are referred back to the community you should make sure they are taking their drugs correctly. As a standard, you will need to follow-up patients on cotrimoxazole prophylaxis every month for the first three months. Later, if no problems occur and if the patient takes the drugs correctly, the follow-up can be done every three months.
Follow-up visits from you should include monitoring for side-effects, and education of the patient on the importance of taking the drugs correctly (this will be further explained in Study Session 23).
Summary of Study Session 21
In Study Session 21, you have learned that:
- An opportunistic infection is caused by pathogens that usually do not cause disease in a healthy person, i.e. one with a healthy immune system.
- The WHO HIV clinical staging system is a staging system developed for patients with HIV to help determine the degree of immune deficiency.
- Identifying opportunistic infections and diseases will help you to categorise PLHIV in one of the four stages of the WHO HIV clinical staging. Stages 1 and 2 correspond to asymptomatic or mild disease, whereas stages 3 and 4 imply serious clinical health problems. Stage 4 is AIDS.
- Common opportunistic infections in PLHIV may be mild (e.g. persistent generalised lymphadenopathy (PGL) at Stage 1), progressing to skin rashes and more serious infections of the mouth, throat and oesophagus at stages 2–4, tuberculosis at stages 3 or 4, and HIV wasting syndrome at stage 4.
- The most commonly used chemoprophylaxis to prevent common opportunistic infections in HIV/AIDS is to administer cotrimoxazole, a wide-spectrum antibiotic that targets several opportunistic infections.
- All PLHIV at WHO clinical stages 2, 3, 4, or with a CD4 count less than 350 cells/mm³, should start cotrimoxazole prophylaxis. Monitoring adherence to the prescribed drug regimen is an important part of the Health Extension Practitioner’s role.
Self-Assessment Questions (SAQs) for Study Session 21
Now that you have completed this study session, you can assess how well you have achieved its Learning Outcomes by answering the following questions. Write your answers in your Study Diary and discuss them with your Tutor at the next Study Support Meeting. You can check your answers with the Notes on the Self-Assessment Questions (SAQs) at the end of this Module.
SAQ 21.1 (tests Learning Outcomes 21.1, 21.2 and 21.4)
Are the following statements that describe the relationship between opportunistic infections in PLHIV and their immune status true or false? In each case, explain your reasoning.
A The decline in the function of the immune system of a person living with HIV is associated with the onset and increasing severity of opportunistic infections.
B The onset of severe opportunistic infections usually occurs at CD4 counts between 800 and 1500 cells/mm³.
C The occurrence of an opportunistic infection in a person who has not been tested for HIV is suggestive of HIV infection.
D PLHIV can be categorised by the WHO clinical staging system according to their most severe opportunistic infection.
Answer
A is true: As the immune system’s ability to defend against infectious diseases declines in PLHIV, various and more severe opportunistic infections appear.
B is false: The appearance of severe opportunistic infections usually occurs when the CD4 count falls to below 450 cells/mm³.
C is true: Patients with opportunistic infections who have not been tested for HIV may be unknowingly HIV-positive. You should counsel and refer the patient for HIV testing. However, you should not classify a patient according to the WHO clinical staging system unless they have tested positive for HIV.
D is true: To classify a patient on the WHO HIV clinical staging system, the patient has to be HIV-positive, and specific diagnoses of opportunistic infections and diseases are required. PLHIV are classified into different stages according to their most severe opportunistic infection.
SAQ 21.2 (tests Learning Outcomes 21.2 and 21.3)
A 27-year-old woman comes to the health post complaining of a painful rash over her back on the right side which started three days earlier. The pain is severe and runs along horizontally. You examine her and identify that the rash is due to vesicles.
- a.What is the possible diagnosis of this patient?
- b.What will you do to help this patient?
Answer
- a.The vesicles suggest it may be a herpes zoster rash.
- b.You need to know first whether the patient is HIV-positive or whether she has ever been tested. If the patient doesn’t know her HIV status, advise her on provider-initiated counselling and testing for HIV. In either case, refer the patient to the health centre for treatment.
SAQ 21.3 (tests Learning Outcomes 21.3 and 21.4)
You are asked to provide a home visit to a 40-year-old man who has been bedridden for four months. He is extremely thin, has diarrhoea and appears feverish. He can hardly speak. His wife died one year ago and he has two children. The elder son says his father was tested positive for HIV four years earlier, but he has not gone back to the health centre since then.
- a.What is the possible diagnosis of this patient?
- b.What is his WHO HIV clinical staging?
- c.What should be done for the patient and his children?
Answer
- a.He may have HIV wasting syndrome.
- b.This is classified as WHO HIV clinical stage 4.
- c.The patient has to be referred to the nearest health centre urgently. He needs urgent treatment for his wasting syndrome as well as antiretroviral therapy for HIV. His children also need to be tested for HIV, as it is possible that the mother died of AIDS-related illnesses.
SAQ 21.4 (tests Learning Outcome 21.5)
A 19-year-old HIV-positive woman comes to you and tells you she wants to stop the cotrimoxazole prophylaxis given to her by the nurse in the nearest health centre. She says she is feeling well and doesn’t need to take the drugs any longer. What will you advise her?
Answer
You need to tell the patient that cotrimoxazole prophylaxis has to be taken continuously unless she is told to stop by her nurse at the health centre. You need to encourage her to take the drugs, and explain that they are helping her to avoid some of the common infections associated with HIV infections such as those that can cause diarrhoea, lung and brain disease. If she needs more help, refer her to the health centre for further support and care.