Use 'Print preview' to check the number of pages and printer settings.
Print functionality varies between browsers.
Printable page generated Friday, 1 May 2026, 5:53 AM
Communicable Diseases Module: 23. Adherence to HIV Care and Treatment
Study Session 23 Adherence to HIV Care and Treatment
Introduction
In the previous study session, you were introduced to the main antiretroviral treatments (ARTs) used for people living with HIV (PLHIV) in Ethiopia. Remember that HIV treatment is a lifelong therapy that improves the quality of life of patients but does not completely eradicate HIV infection; that is, the virus persists within the infected person’s body. It is therefore essential that a person living with HIV takes their medication correctly. In this study session, we turn our attention to a critical aspect in HIV treatment and care — adherence. The purpose of this study session is to describe the key concepts of adherence to HIV care and treatment in the context of the services provided for PLHIV in Ethiopia. Here, you will learn why adherence to ART is important, what factors influence adherence from both a patient’s and the health facility’s perspective, and how you can provide advice to HIV patients in the community and at the health post to achieve optimal adherence.
We will then describe the common barriers to adherence to HIV care and treatment that PLHIV face. This will enable you to help patients to continue their follow-up at healthcare units in order to maintain and improve their health. The knowledge gained in this study session will also help you to assess and identify patients who adhere poorly to their treatment and encounter challenges in taking their drugs properly. Hence you will be able to offer them supportive advice in the form of follow-ups at the community and/or refer them to the nearest health centre to provide additional support and treatment services, and ultimately improve the outcome of patient care.
Learning Outcomes for Study Session 23
When you have studied this session, you should be able to:
23.1 Define and use correctly all of the key terms printed in bold.(SAQ 23.1)
23.2 Explain the factors affecting adherence and their importance in maintaining adherence to HIV treatment. (SAQ 23.2)
23.3 Describe optimal adherence to HIV treatment and its goal. (SAQ 23.3)
23.4 Explain the consequences of poor adherence to HIV therapy and its association with drug resistance. (SAQ 23.1)
23.5 Assess the adherence status of PLHIV and advise them on how to improve it. (SAQ 23.3)
23.6 Describe the adherence support mechanisms that cover specific needs of patients on HIV therapy. (SAQs 23.2 and 23.4)
23.1 What is adherence?
Adherence to treatment in the context of any disease is essential to maintain and improve a patient’s health. Similarly, adherence to HIV therapy is essential for the general improvement of quality of life of PLHIV. In the context of HIV treatment, adherence means that a patient takes antiretroviral (ARV) drugs correctly. Incorrect drug taking may not only be inefficient in treating HIV infection, but it may also lead to drug resistance (Study Session 22, Section 22.3.2). Using these drugs correctly involves taking the right drug, in the right dose, in the right frequency, at the right time. We will describe the importance of each of these aspects of taking drugs in turn.

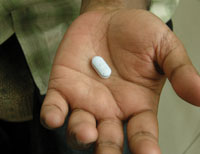
- The right drug: The drug that is prescribed by the health practitioners should not be changed or replaced by any other drug. PLHIV may take various drugs at any given moment depending on their health situation. Usually, patients take ARV drugs to treat HIV infection and other drugs, such as cotrimoxazole, to prevent opportunistic infections. Therefore, it is not unusual for PLHIV to become confused, and they may find it difficult to differentiate between the many different drugs they may be taking (Figure 23.1). Your support is essential in enabling PLHIV to take the right drugs.
- In the right dose: As you learnt in the previous study session, ARV drugs have specific dosages for adults and children. The dose may also sometimes be different amongst adult patients depending on their health status. Therefore, if you are making follow-ups for patients who are taking drugs for HIV in your community, you have to make sure and encourage them to take the correct dose of the drugs.
- With the right frequency (number of times per day): Like other drugs, ARV drugs are prescribed by health practitioners at the health centre or hospital with instructions on how frequently they should be taken in a day. You have to advise patients to follow those instructions strictly.
- At the right time: The time at which ARV drugs should be taken is also essential, maintaining a regular and correct time difference between doses.
Taking the correct ARV drugs at the right doses and frequency, spaced at regular intervals, helps patients to maintain the optimum levels of drugs in their blood to prevent HIV multiplication.
Based on what you learnt in previous study sessions, why is it important to take ARV drugs for the duration of a patient’s lifetime?
ART is a lifelong treatment because it doesn’t eradicate HIV infection; rather it suppresses the multiplication of the virus in the body. This prevents the destruction of CD4 lymphocytes and maintains the normal function of the immune system.
Viral replication refers to the production of new viruses by infected cells. ‘Viral replication’ and ‘viral multiplication’ can be used interchangeably.
Note that adherence to HIV treatment and care not only involves the points above concerning ARV drugs, but also attendance by the patient to all scheduled visits at health centres or hospitals to undertake regular check-ups and clinical assessments. Regular clinical follow-ups may include clinic appointments, laboratory tests and prescription refills. You need to support and encourage PLHIV to regularly visit health facilities as advised by the health workers who follow their treatment and/or provide care. In fact, adherence should involve a long-lasting partnership between the patient and the whole healthcare team, including Health Extension Practitioners (Section 23.5.2).
23.2 What is non-adherence?
Non-adherence is the patient’s inability to take their drugs correctly, or attend scheduled clinical visits in the prescribed manner as recommended by their healthcare providers. Non-adherence has a number of implications for the health outcome of your patients. A patient who is not taking drugs correctly will have poor health and get ill with opportunistic infections frequently. They may also end up developing resistant strains of HIV (or other infectious agents in the case of non-adherence to treatment for opportunistic infections) that will be difficult to treat with the conventional treatments available in your settings. Therefore you need to help and actively advise patients to strictly adhere to all of the services they receive from the health facilities.
In addition to good adherence, other factors should be considered if a patient with HIV needs to be started on ART.
The health practitioners who are monitoring the patient at the health centre or hospital should check whether they are eligible to start ART. This is carried out by clinical assessment (i.e. symptoms and/or signs of disease), and by checking the CD4 cell count of the patient.
23.3 The goal of adherence to ART
From a clinical point of view, patients need to achieve optimal adherence to ART to maintain an efficient level of drugs in their bodies. The measurable goal of adherence for your patients in the community or at the health post should be 100%. Poor adherence (adherence below 100%) leads to drug resistance, increased viral load, increased sickness, and increased possibility of death. Therefore, your activity in the community consisting of follow-up visits to patients on ART or other treatments contributes significantly to the general adherence status of your patients.
Optimal means ‘the most effective’.
How do you assess the adherence status of a person living with HIV on ART? Adherence is a measurable pattern of behaviour. For example, you can calculate the percentage of tablets taken correctly in a month by dividing the total taken by the total number that should be taken. Then you multiply that number by 100 to obtain the percentage adherence of an individual on ART. Optimal adherence is 100%, which means that a patient should take all of their drugs correctly without missing any one at any single time (Figure 23.2).
Calculate the monthly percentage adherence of a patient who missed six tablets out of the total he should be taking in a 30-day month. He should take two tablets every day.
This patient takes two tablets every day, so he should take a total of 60 tablets in one month. However he missed six tablets in one month. So his monthly adherence is 54 tablets out of 60. So, by dividing 54 by 60 and multiplying the result by 100, his percentage adherence can be calculated as 90% (54/60 = 0.9 × 100 = 90).
23.4 Why is drug resistance important for ART?
Blood levels of ARV drugs have to be maintained at optimal concentrations in order to be effective against HIV. Poor adherence to ART will result in low blood levels of ARV drugs, and these low concentrations will be unable to completely suppress viral multiplication. In these conditions, the virus can change in such a way that it resists the action of the drugs, even if drug blood levels return to normal, that is, even if the patient resumes good adherence to ART. Hence, drug-resistant viruses will multiply faster in a patient with a history of poor adherence, leading to the patient becoming sicker. In addition, drug-resistant HIV can be transmitted to other individuals for whom these drugs will not work either.
Whether a person living with HIV is infected with drug-resistant HIV can be confirmed at a hospital by specific blood tests. If this is the case, the regimen of drugs taken by that individual will have to be modified and new drugs prescribed. However, drug resistance is not without problems when it comes to HIV treatment, for two reasons. First, there are limited numbers of drugs available in Ethiopia. Secondly, it may be more difficult for a patient to maintain adherence to the drugs used to replace first-line ARV drugs to which HIV has become resistant, due to their increased side-effects and the larger number of tablets to be taken.
What are the consequences for a patient who has not adhered to their ART treatment and failed to respond to first-line drugs?
In general if patients needing ART treatment fail to adhere to their initial treatment, then HIV within these patients may develop resistance to their ARV drugs. If this patient is not prescribed other combinations of ARV drugs (which may be more difficult to adhere to), they will eventually become sick and develop AIDS-related symptoms.
23.5 Why do people fail to take ARV drugs correctly?
In order to help patients in your community, you need to understand the common problems that people on ART encounter that may influence adherence. These are usually different from community to community, and even from individual to individual. In this section, we will give you a general overview of the factors that may affect adherence either negatively or positively. We have classified these factors as either related to the patients, or to the healthcare provider like nurses, doctors, or you working in the community.
23.5.1 What personal, family or community factors influence adherence?
Barriers to adherence arising from the patients themselves include personal, family or community factors. Examples of personal circumstances that negatively influence adherence are patients that repeatedly forget to take their medication, patients that travel away from home without medication, and patients who develop mental health issues, or who have a history of drug or alcohol abuse that may interfere with their ability to take drugs as prescribed. Economic problems, such as lack of money for transportation to the healthcare provider can also negatively affect adherence. Other issues are related to low literacy or lack of understanding of the treatments a patient should be taking. Religious beliefs should also be taken into account in the context of adherence. For instance, fasting during daytime is a common religious practice for many Ethiopians, and may therefore interfere with the frequency of daily doses to be taken for ART.
At the family or community level, stigma and/or discrimination may make it difficult for a patient to adhere to ART due to the absence of a supportive environment. Another example involves pressure from others to comply with certain practices (i.e. travelling to Holy Water or other local rituals) that may negatively influence adherence (Figure 23.3).
In the context of HIV/AIDS, Stigmatisation is the negative labels or stereotypes used when referring to PLHIV. Stigmatised PLHIV often feel isolated, abused and discriminated against by other members of the community.

By contrast, other factors can help your patients to take their treatments properly. The ability of your patients to make their medication a routine part of their life is the first step in good adherence practice. Most patients use reminders to take their treatment at the right time. Some may use alarms, and others may use routine activities such as prayer time as reminders. You may have to help your patients find the right reminder, based on their individual circumstances.
What other factors involving the family and/or community may positively influence adherence to ART?
Social support, motivation and encouragement are all helpful. Treatment supporters such as friends and partners, or members of an ART support group can contribute tremendously to adherence in ART.
23.5.2 How can healthcare providers affect patient adherence?
The role of health workers like you is essential for good adherence to ART. Good knowledge and skills about ART and issues concerning adherence, and about patient education and counselling, can provide them with practical support. Healthcare providers can help patients by providing medication alerts, charts, diaries, by giving them advice on the use of reminders, and by putting into place tracking mechanisms for their drug intake. By providing support for patients, you can create trust and maintain a fruitful partnership between the patients and the health system.
Negative attitudes towards patients’ ability to adhere to ART will discourage your patients and undermine their efforts to maintain good adherence practices. By contrast, positive views about patients’ attitude to treatment, and being careful to avoid patients feeling controlled, will help you to build a successful partnership with patients to promote optimal adherence (Section 23.6).
23.5.3 What other factors negatively affect adherence to ART?
There are other factors unrelated to patients or to the healthcare provider that result in poor adherence. The most common ones are the large number of tablets to be taken, high frequency of doses, and common side-effects like nausea and vomiting. Pill burden is one of the key factors that can affect adherence negatively. These factors are relatively easy to deal with — for example, patients may simply need reassurance about the treatment’s side-effects, or a change in the frequency of doses (twice versus three times per day). Other factors, especially those associated with drug interactions and food restrictions towards different drugs, may require referral to a health centre or hospital for counselling and other support services. At the health centre, health workers will help your patients to find solutions related to common adherence problems.
A patient on ART in your community tells you that he wants to stop taking his cotrimoxazole prophylaxis medication because he is also taking ARV drugs. He describes how difficult it is to take so many tablets in a day. What advice will you give him?
Reassure the patient that drugs should be taken as prescribed by the health workers. As you are not allowed to stop any of the drugs, refer him for further support to the health centre.
23.6 Encouraging good adherence in patients on ART
During follow-up visits, you need to keep in mind several general issues when giving advice and counselling related to adherence to HIV therapy and care to PLHIV.
First, giving information to patients, and their active involvement in deciding whether to follow ART, are essential for good adherence practices and hence for treatment success. Patients should be informed beforehand of the consequences for their lifestyle of starting HIV therapy. They should realise that the decision whether to take ARV drugs or not will influence their own long-term health. Moreover, patients should be aware of the fact that ART is a lifelong commitment. In preparing patients to start ART, other factors that may affect adherence should be discussed, including those related to disclosure of their HIV-status to partners and family members, and socio-cultural issues like stigma and discrimination.
Secondly, a patient’s adherence to ART may be affected by difficult life situations. The support and monitoring provided to patients by their healthcare providers is critical for maintaining good adherence throughout the patient’s life. In your community, you will need to undertake follow-up and monitoring activities to ensure adherence to ART and HIV care services. This is particularly important in the instances when a patient is confronted with difficult life situations. If adherence has not been strictly followed, patients need to be supported, not blamed, punished, made to feel guilty, or controlled in any way. In order to achieve this, you and the patient will need to work collectively as a team with the health practitioners in health centres and hospitals, including nurses, doctors, adherence counsellors, pharmacists, pharmacy technicians and voluntary health workers in the community.
Finally, it is important to discuss with patients and identify a person who is willing to escort PLHIV on ART to the health facilities as a treatment supporter. This may be the patient’s partner, a friend, or a family member chosen by the patient to help them remember not only to attend clinic appointments, but also to take the drugs correctly. Similarly, PLHIV or ART support groups can encourage adherence. Support groups are good sources of information and educational resources for those who start treatment, or are already on treatment.
23.6.1 What should you do before a patient starts ART?
Starting ART is a life-changing experience for most PLHIV. As adherence is a skill that your patients learn progressively, you have to start supporting them by providing information, education and counselling about maintaining complete adherence. Before starting ART, the health workers or adherence counsellors at the health centre should ensure that the topics listed in Box 23.1 are well explained to the patient. At the community level, you may also be expected to repeat this kind of information and education for patients who are about to start ART, as the patient may feel overwhelmed by the amount of information they receive.
Box 23.1 Information that should be given to patients before they start ART
- Define antiretroviral therapy (ART) and give basic drug information.
- Define adherence and teach the goal of 100% optimal adherence.
- Discuss reasons why adherence is important and the consequences of non-adherence.
- Help patients learn what to expect from the treatment, the timing of taking their drugs, and possible side-effects.
- Tell them what to do if they miss a dose.
- Help them identify potential barriers to optimal adherence and create plans for success.
This information will enable patients to understand their treatment regimen better, and empower them to adhere to their prescriptions more successfully once they start ART. You should also help them identify potential barriers to adherence, and organise support systems in the community or at home to promote adherence. If they encounter difficulties once they start treatment, patients should be reassured that these will be solved in partnership with the healthcare team. Patients should understand that sometimes you will refer them to other support services to help address barriers like financial difficulties, transportation, housing and food support. Discuss with your patient delaying the start of ART until significant barriers are addressed.
Tailoring treatment to the patient’s lifestyle and routine is a key factor for good adherence. For example, you could encourage the patient’s self-confidence by helping them to identify reminder strategies like daily activity planning, pill box, diary, calendar, telephone reminder, etc. Alternatively, you could suggest they associate taking ARV drugs with regular daily events such as meals or prayer, or designate specific places and times for taking medications. Patients have to plan ahead for changes in routine lifestyle, such as travel. You need to educate them about possible side effects, and instruct patients on how to manage them, or to go to the health facilities for further care and support if they are struggling to maintain 100% adherence.
23.6.2 What should you do after a patient starts ART?
Once patients start ART, they need to get support from you and the rest of the healthcare system to maintain adherence at all times. From the perspective of a Health Extension Practitioner, you need to follow-up patients closely and frequently in the form of regular visits or appointments. At these meetings, you should be vigilant of factors that can affect adherence significantly. This is particularly important at the start of ART, as there might be side-effects that may result in poor adherence. Discuss adherence at each visit and ask patients about new symptoms or any changes in their health status. If they have new symptoms, refer them to the health centre for better management. Reinforce the information and education about adherence given previously by assessing their knowledge and skills.

Providing support for adherence to HIV treatment and care involves creating a comfortable atmosphere where exchange of information between you and the patient is encouraged on each visit or appointment (Figure 23.4). As you talk to your patient, always use simple terms and visual aids, if available. Being non-judgmental and creating a trusting environment are essential in making the patient feel comfortable. Asking open-ended questions will enable you to assess whether the patient has understood the information you have provided in the current meeting or in earlier meetings. For example, ‘Sometimes it is difficult to take medications on time. Have you missed any pills since your last appointment?’, or ‘Why do you think you were unable to take your pills on time?’
Assessment of adherence should also be part of each visit as patients come for appointments, or as you visit them in the community. You should assess their percentage adherence (as explained in Section 23.3). If adherence is not 100%, try to get specific information about missed doses and work with the patient to determine why they encountered problems and which specific strategies might enable them to achieve 100% adherence. You should also attempt to recognise and acknowledge the difficulties of adherence and show a positive attitude. Patients should be regularly reminded about taking their medicine at the right time, but in a way that makes them feel motivated and encouraged to achieve 100% adherence to improve their quality of life.
If doses are missed, use the following rule to help your patients: If the drug is taken twice a day, the missed dose can be taken up to six hours later, but no later than that. For example, if the normal dose is taken at 7:00 a.m., the missed dose can be taken up to 1:00 p.m. Again, you can convey this message to the patient in simpler terms. For example, ‘If you miss a dose, take the dose as soon as you remember, but not if it is almost time for your next regular dose. Never take a double dose.’
Notify an HIV/AIDS healthworker at the nearest health centre if there are adherence difficulties, and discuss it with the healthcare team. In your regular follow-ups with PLHIV, help them to identify strategies to improve adherence. These may include using a treatment supporter, more home visits, either by you or by voluntary community health workers, a referral to home-based care, or encouraging patients to participate in social support activities such as participation in a PLHIV support group.
Summary of Study Session 23
In Study Session 23, you have learned that:
- Adherence to HIV care and treatment is essential for improving the health and quality of life of PLHIV.
- Adherence to treatment means taking the right drugs at the right dose and prescribed frequency.
- Adherence to ART is unique, in that for optimal treatment it requires 100% strict adherence.
- The result of poor adherence to ART is the development of resistance to the drugs, which leads to more difficult options for future treatment.
- There are factors relating to the patients’ life circumstances, their family, their community, and the behaviour of health workers that affect adherence negatively and positively, and you need to identify them to help your patients on ART in the community.
- Before starting ART, there are essential issues such as adherence preparation and education that need to be discussed with patients.
- In adherence follow-up meetings, one of your responsibilities is to calculate the percentage adherence of your patients and encourage them to maintain good adherence.
Self-Assessment Questions (SAQs) for Study Session 23
Now that you have completed this study session, you can assess how well you have achieved its Learning Outcomes by answering the questions below. Write your answers in your Study Diary and discuss them with your Tutor at the next Study Support Meeting. You can check your answers with the Notes on the Self-Assessment Questions at the end of this Module.
SAQ 23.1 (tests Learning Outcomes 23.1 and 23.4)
Explain what poor adherence to ART means, and why it results in drug resistance and poor health in PLHIV.
Answer
Poor adherence to ART means not taking drugs as prescribed by the health workers. It results in low levels of drugs in the blood so that multiplication of HIV is not completely suppressed, thereby inducing resistance to drugs. As a result of increased multiplication of the virus, CD4 lymphocytes will be destroyed, which results in various opportunistic infections that damage the patient’s health.
SAQ 23.2 (tests Learning Outcomes 23.2 and 23.6)
A female patient who is on ART comes to your health post and tells you that she takes her drugs in hiding from her family, as she does not want them to know about her HIV status. She says she has missed three tablets in the last two weeks, as she could not take them in front of her relatives. How can you help her?
Answer
One of the barriers of adherence is stigma and discrimination resulting from patients not disclosing their HIV status to people around them. In this patient’s case, counselling about disclosure is essential, and you should try to find someone in the family or the community who will support the patient in taking ART. Otherwise, refer the patient to the health centre for further support.
SAQ 23.3 (tests Learning Outcomes 23.3 and 23.5)
For the patient in SAQ 23.2, ART involves taking one tablet twice per day. Based on the total number of missed tablets in a month, calculate her adherence percentage. Is her adherence percentage optimal?
Answer
If she is taking two tablets per day, then a total of 28 doses are expected in 14 days. If she misses three tablets, then she has taken 25 out of 28 tablets. Therefore, her adherence level is 25 × 100/28 = 89%. Her adherence is not 100%; therefore you need to counsel her about strict adherence.
SAQ 23.4 (tests Learning Outcome 23.6)
Explain what it means to form a partnership between you, as the Health Extension Practitioner, and your patient in adherence counselling.
Answer
In adherence counselling, a partnership between the patient and the healthcare team is vital. It means you should treat your patients as an active agent of their own health. Your relationship with them shouldn’t be like a boss who tries to control their behaviour. An equal partnership greatly helps in building trust with your patients.