Use 'Print preview' to check the number of pages and printer settings.
Print functionality varies between browsers.
Printable page generated Saturday, 6 June 2026, 3:50 PM
Communicable Diseases Module: 28. HIV in Children
Study Session 28 HIV in Children
Introduction
In Study Session 27, you learnt that mother-to-child transmission of HIV during pregnancy, delivery and labour, and breastfeeding are the main sources of HIV infection in children. In this study session, we will focus on the consequences of HIV infection in children. You will first learn about the key differences in chronic HIV care between adults and children. The immune system in young children is still developing, and as a consequence HIV-infected children suffer from many more opportunistic and common infections, and also progress more rapidly to AIDS than HIV-infected adults. For these reasons, early diagnosis and treatment of HIV infection is particularly important in children.
Within your health post, you will have to establish a link between your own family-focused care and HIV care services. To do so, you will need to learn how to routinely discuss and recommend HIV testing for children born to HIV-infected mothers, and when it is appropriate to refer them. Finally, we will briefly describe important issues concerning the care of HIV-infected children, namely their nutritional status and psychosocial needs. You will learn more on the diagnosis of HIV in children, and the care for HIV-exposed infants and HIV-infected children in the Integrated Management of Newborn and Childhood Illness (IMNCI) Module.
Learning Outcomes for Study Session 28
When you have studied this session, you should be able to:
28.1 Define and use correctly all of the key words printed in bold. (SAQ 28.1)
28.2 Describe the key differences in diagnosis of HIV status and chronic HIV care between adults and children. (SAQs 28.1 and 28.2)
28.3 Explain when to refer HIV-exposed infants born to HIV-positive mothers for early diagnosis. (SAQ 28.3)
28.4 Describe the nutritional and psychosocial needs of children with HIV. (SAQ 28.3)
28.1 Critical issues in HIV infection and progression to AIDS in children
There are important differences in HIV infection and progression to disease between adults and children. These have implications for the care needed by HIV-infected children (explained further in Section 28.3). We will describe here the main issues related to HIV/AIDS and children that will help you provide the best care for HIV-infected children in your community.
28.1.1 Minimising risk of infection in children
The most important thing for you to remember in the context of HIV prevention in children is that mother-to-child transmission is the main source of HIV infection. Children at any age who continue to be breastfed from HIV-positive women are at risk of acquiring HIV infection through contaminated breastmilk throughout the time they are breastfed. You should provide feeding advice to mothers according to the national guidelines on infant feeding (this is covered in detail in the Integrated Management of Newborn and Childhood Illness Module).
Remember the AFASS criteria. It is not always possible for a mother to give her child replacement milk; sometimes breastfeeding is the only viable option.
Where one child is HIV positive, it is possible that other family members, including siblings (brothers and sisters), are already infected. Therefore, you should always encourage HIV testing of parents, and young, siblings of HIV-exposed infants and HIV-infected children. You should appreciated that unless an HIV test result is confirmed, infants born to HIV-positive mothers are called HIV-exposed infants, and HIV-infected children are those whose HIV test results are confirmed as being positive.
What is the main route of HIV transmission among adults?
The main route of HIV transmission among adults is sexual intercourse.
28.1.2 Early diagnosis of HIV
There are differences in disease progression and diagnosis of HIV infection between adults and children. The main differences in disease progression and diagnosis are listed below:
- Young children have immature immune systems and thus are more susceptible to common childhood infections, as well as opportunistic infections.
- Early diagnosis of HIV infection in children is essential, as the infection in infants and children progresses faster than that of adults Although HIV-infected infants are generally symptom-free at birth, in the absence of any intervention, most of them develop severe symptoms in the first two years of life, and die. Therefore, early diagnosis and management of HIV-exposed and HIV-infected children is key to ensure maximum benefit from ART, and to reduce AIDS-related morbidity (the presence of an illness or disease) and death in children.
- In HIV-exposed infants, maternally acquired antibodies make the diagnosis of HIV challenging. The antibodies present in the blood of an HIV-exposed infant may originate from the mother and not the infant itself. Therefore, a positive rapid HIV test is not definitive for the diagnosis of HIV infection in children below the age of 18 months. However, a rapid test, done six or more weeks after the complete cessation of breastfeeding, which gives a negative result, is more useful, because it excludes HIV infection in HIV-exposed infants.
The antibodies the mother makes against her HIV can cross the placenta and get into the fetal bloodstream. After birth, these antibodies can show up when the baby is HIV-tested.
28.1.3 Differences in the management of children and adults with HIV
The management of HIV in children, especially the young ones, differs from that of adults. Below are some of these differences:
- Normal CD4 counts are higher in young children than in adults, and decrease with age to reach adult levels around the age of six years. In children younger than six years, it is better to use the percentage of CD4 cells in the blood as a criterion to start ART. This is more stable than the CD4 cell count used in adults.
- Once started on ART, children need to be followed-up more frequently than adults. Their response to ART should be checked by regular monitoring of growth and development (Figure 28.1 illustrates the profound improvement that can be seen in HIV-positive children given ART).
- ARV drug dosages need to be adjusted regularly to account for changing body weight and growth as children develop.
- Communication with children can be challenging. This regards issues related to disclosure, counselling and explaining the need for long-term treatment, particularly adherence to the treatment regimen.
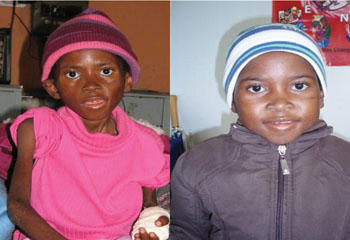
28.2 Providing care for HIV-exposed infants and HIV-infected children
Routine childhood services, e.g. immunization, nutrition, OPD (out-patient department) and in-patient (hospital ward) services, are entry points for HIV-exposed and infected children. Health workers should use these services as opportunities to provide access to early diagnosis of HIV for families with children at risk.
As we discussed above, HIV-exposed infants/children should be enrolled into HIV care services and receive a regular follow-up at a health centre or hospital. They should also be given cotrimoxazole prophylaxis to prevent severe infections such as pneumocystis pneumonia (a fungal infection of the lungs), which can cause death in HIV-infected children. Cotrimoxazole prophylaxis is given to HIV-exposed children starting from four to six weeks of age, until a diagnosis of HIV infection is definitely excluded. Those who present late to a health facility should also be given cotrimoxazole prophylaxis.
Cotrimoxazole prophylaxis is also protective against opportunistic bacterial infection, as you learnt in Study Session 21.
Remember that a rapid HIV test is not a reliable test to diagnose HIV infection in children under the age of 18 months. This is because there are maternally acquired antibodies in the blood of the child, and these antibodies can give a false positive HIV test result. Therefore, the best test for diagnosing HIV infection in children less than 18 months of age is a DNA PCR test (see Figure 28.2). This test detects the presence of viral components in blood. However, you are not required to know the details of this test.

The Federal Ministry of Health of Ethiopia has already started a DNA PCR service at several regional laboratories, where blood samples can be sent for analysis to aid early infant diagnosis. DNA PCR can be done as early as six weeks of age. Therefore, you, as a health worker, should encourage the family of an HIV-exposed infant/child to take the infant/child to a nearby health centre for early diagnosis.
DNA PCR does not rely on the detection of antibodies – remember, these could come from either the mother or baby. Instead, this test looks for DNA molecules that can only come from the virus. If the test is positive, it means the virus is in the baby’s blood.
When you encounter such children, either when visiting a household or at the health post, you should inform the family or caregiver about the importance of follow-up care and cotrimoxazole prophylaxis for the HIV-exposed child. The caregiver might not easily recognise the importance of cotrimoxazole prophylaxis and follow-up care, particularly if the child appears to be healthy. Your role is to coordinate the care of the HIV-exposed child with that of the mother.
28.3 Nutritional and psychosocial support for children with HIV
HIV-exposed infants and HIV-infected children need special nutritional and psychosocial support, both at the level of the health facility and the community. Below we will discuss why they need this special support.
28.3.1 Nutritional needs of HIV-infected children
The nutritional status of a child will significantly affect the incidence and severity of HIV-related illnesses, such as tuberculosis and diarrhoea. In addition, HIV-related illnesses also have severe nutritional consequences that commonly precipitate appetite loss, weight loss and wasting. Clinical situations that may impair the nutrition of HIV-infected children are recurrent or chronic infection, fever, intestinal infections, oral or oesophageal lesions, and persistent diarrhoea. Box 28.1 summarises some of the key issues that need to be considered when thinking about the nutritional needs of HIV-infected children.
Box 28.1 Nutritional management of HIV-infected children
- Increase energy intake by 50% to 100% over normal requirements in children experiencing weight loss.
- Identify local foods that are available and affordable, and provide advice for the caregiver on energy requirements. For the type of local foods that are available, you may find it useful to refer to a local food adaptation table.
- HIV-infected children from the age of six months should receive vitamin A supplements every four to six months (100,000 IU for infants up to 12 months, and 200,000 IU for children above 12 months.) This level is consistent with the current WHO recommendations for the prevention of vitamin A deficiency in all children.
- For persistent diarrhoea, refer to the IMNCI Module.
- Feeding and increased fluids should continue during illness. The child may develop nausea and vomiting as a result of ARV drugs. Encourage small, frequent fluids, and give foods that the child likes. Let the child eat before medication. For a child with sores in the mouth, give soft and mashed food, or give paracetamol half an hour before solid feeding.
Note: you will also learn more on this topic in the IMNCI Module.
28.3.2 Providing psychosocial support to children infected with HIV
Beyond disease management, children infected with HIV face a number of problems that impact upon their social, educational and emotional development and wellbeing. These children require psychosocial support, which includes a range of interventions that enable individuals and families to cope with the overwhelming feelings that result from their experiences with long-term disease and death. Providing psychosocial support may include addressing self-esteem, adaptation to illness and its consequences, communication, social functioning and relationships — these topics will be discussed in more detail in Study Session 30 (Providing Palliative Care for people living with HIV.)
Health facility-based and home-based stimulation of children improves their mental, social and emotional development. Remember, encourage family members to play and talk with the children. This will help provide an enriching and stimulating environment that will greatly enhance and support the children’s psychosocial development.
For those children who are also malnourished, combining psychosocial stimulation with food supplementation has been shown to produce better outcomes and growth for the children.
Children’s development will flourish when they form secure attachments to a responsive caregiver. Furthermore, children need to be provided with psychological (relating to both the mental and social aspects of life) and emotional support within their family or through other caregivers, and to be able to communicate openly about their own or their family member’s condition, so as to give relief to deep fears that may be difficult to share.
You may need to provide psychosocial support to HIV/AIDS orphans (children who have lost their parents through HIV/AIDS).
For caregivers to provide this support to children, they must themselves be provided with psychosocial support. This can be done when you do home visits, or through community-based organisations or peer support groups. It is important for you to ensure adequate linkage of families with these groups, and to pay attention to the psychosocial needs of the whole family on each visit.
Summary of Study Session 28
In Study Session 28, you have learned that:
- There are differences between HIV infection in adults and children. The main differences are the mode of transmission of HIV, disease progression, diagnosis of HIV infection, especially among children less than 18 months of age, and that CD4 counts are higher in children compared with adults.
- ARV drugs are handled differently in children’s bodies, affecting the doses that are needed. Dosages in children need to be adjusted to the child’s weight as the child grows.
- Communication, adherence and disclosure in children are challenging.
- Infants and children born to HIV-positive parents should be tested for HIV as early as possible. If not, they may die of common childhood illnesses and opportunistic infections in a shorter time. You need to refer such infants/children to a nearby health centre/hospital for early infant diagnosis.
- HIV-infected children need special psychosocial and nutritional support.
Self-Assessment Questions (SAQs) for Study Session 28
Now that you have completed this study session, you can assess how well you have achieved its Learning Outcomes by answering the following questions. Write your answers in your Study Diary and discuss them with your Tutor at the next Study Support Meeting. You can check your answers with the Notes on the Self-Assessment Questions at the end of this Module.
SAQ 28.1(tests Learning Outcomes 28.1 and 28.2)
What is meant by the term ‘HIV-exposed infant’? How is the child’s HIV status diagnosed?
Answer
HIV-exposed infants are infants born to HIV-infected mothers. The HIV status of such infants is regarded as unknown until a definitive rapid diagnostic test is carried out at the proper age and conditions (e.g. cessation of breastfeeding for longer than 6 weeks before the test), or until a DNA PCR test (that measures directly viral components in the blood) is performed. If the test confirms the presence of HIV in the infant’s blood, we considered the infant to be infected by HIV.
SAQ 28.2 (tests Learning Outcome 28.2)
Which of the following statements is false? In each case, explain what is incorrect.
A The progression of HIV infection in children is slower than that of adults because they have fewer viruses in their body.
B Rapid HIV testing can confirm HIV infection in a six-months-old infant born to an HIV-positive mother.
C ARV drug dosages should be adjusted as the child gains weight or grows.
D Young children normally have higher CD4 counts than adults, and it is better to use the CD4 percentage (instead of the CD4 cell count) as a criterion of whether to start them on ART.
Answer
Statements C and D are true.
A is false. Compared to adults, HIV infection progresses more rapidly in children, due to their immature immune system.
B is false. In children under the age of 18 months we do not use a rapid HIV test to confirm HIV infection, because maternally acquired antibodies can give a false positive test result. The definitive diagnosis of HIV at this age is done by using DNA PCR testing.
Read Case Study 28.1, and then answer the questions that follow it.
Case Study 28.1 Kebede’s story
Kebede is a one-year-old male child who is the last of three siblings. All of the three live with their grandmother who is 65 years old. You hear from the grandmother that the mother of the children died of AIDS six months after giving birth to Kebede, and their father died in an accident 10 months ago. The grandmother also explains to you that Kebede is not feeling well, and has had diarrhoea on and off for two months. He has also lost weight. The grandmother needs your help.
SAQ 28.3 (tests Learning Outcomes 28.1, 28.3 and 28.4)
- a.What do you say about Kebede’s HIV status?
- b.Explain what you should do for Kebede.
- c.Will screening his siblings for HIV help the family?
Answer
- a.Kebede is an HIV-exposed infant, since he was born to an HIV-positive mother. Remember that unless their HIV test result is confirmed, infants born to HIV-positive mothers are called HIV-exposed infants.
- b.You should teach the grandmother about HIV transmission and prevention. You should stress that HIV might have been transmitted to Kebede from his mother. Hence, you should advise the grandmother to take Kebede to a nearby health centre or hospital for management of the diarrhoea and early infant diagnosis of HIV infection. You should provide her with oral rehydration salts (ORS) and tell her how to give it to the infant until he arrives at the health centre. Remember that she should continue feeding him with locally available foods recommended for children with chronic diarrhoea.
- c.Screening Kebede’s siblings for HIV is also important to provide early care for them if they are HIV-infected.