Use 'Print preview' to check the number of pages and printer settings.
Print functionality varies between browsers.
Printable page generated Saturday, 6 June 2026, 3:50 PM
Communicable Diseases Module: 31. Prevention and Control of Sexually Transmitted Infections
Study Session 31 Prevention and Control of Sexually Transmitted Infections
Introduction
In this study session you will be learning about prevention and control of sexually transmitted infections (STIs) or in other words, infectious diseases that are transmitted primarily (although in some cases not exclusively) by the sexual route. You will also be studying about the relationship between HIV and other STIs. This session also describes syndromic management of STIs, that is a diagnosis based on the identification of the symptoms the patient reports and the signs the health care provider observes. Syndromic management of STIs is the standard approach for diagnosis and management of these communicable diseases recommended by the WHO and adapted by the FMOH for use at both health centre and hospital level. After studying this study session you should be able recognise patients who have STIs in the community. This will help you to refer patients with STIs to the nearest health facility. Treatment and care for STIs includes HIV testing and counselling, prevention and treatment of other STIs, and couple counselling and treatment. Note that at the moment you are not expected to treat or manage patients with STIs at the health post or in the community. You are expected to recognise cases of STIs in your community or at the health post and refer them to the health centre for further care.
Learning Outcomes for Study Session 31
When you have studied this session, you should be able to:
31.1 Define and use correctly all of the key words printed in bold. (SAQ 31.1)
31.2 Explain the routes of transmission and risk factors for the common sexually transmitted infections (STIs). (SAQ 31.1)
31.3 Describe the signs and symptoms of common STIs. (SAQ 31.2)
31.4 Briefly describe the importance of syndromic management of STIs. (SAQs 31.3 and 31.2)
31.5 Explain the importance of STIs in the prevention of HIV transmission. (SAQ 31.4)
31.6 Describe how you would identify and offer provider-initiated testing and counselling for people with STIs and refer them to the nearest health centre for treatment. (SAQ 31.2)
31.1 Introduction to sexually transmitted infections (STIs)
Sexually transmitted infections (STIs) is a term used to describe more than 20 different infections that are transmitted mainly through sexual contact via the exchange of semen, vaginal fluid, blood and other fluids; or by direct contact with the affected body areas of people with STIs. Sexually transmitted infections are also called sexually transmitted diseases (STDs) or venereal diseases. In this study session, we will be talking about STIs in general, with particular emphasis on their impact on individual health. You will also appreciate the implications of preventing STIs in reducing HIV transmission, and the complications resulting from untreated STIs.
STIs are very common. The most widely known are gonorrhoea, chlamydia, syphilis and HIV. STIs can cause serious and permanent complications in infected people who are not treated in a timely and effective way. In people with untreated STIs, the complications and long-term consequences can be devastating. The social and economic burden of STIs can be enormous. Untreated STIs can lead to loss of employment and broken marriages. STIs can place a heavy financial burden on families, communities and health services.
Prevention campaigns in order to reduce the incidence of STIs have a marked impact on the general health of the population. Effective prevention of STIs reduces complications that are life threatening for the infected individual, and decreases economic and psychosocial problems associated with the complications arising from STIs.
Fewer STIs means fewer complications like pelvic inflammatory disease (PID), inflammation of the uterus and fallopian tubes due to bacterial infection or other pathogens), infertility, ectopic pregnancy (pregnancy outside of the uterus), etc. as well as decreased rate of HIV transmission during unprotected sexual contacts.
The uterus and fallopian tubes form part of the female reproductive system. You have learned about the female reproductive system in Study Session 3 of the Antenatal Care Module, Part 1.
For patients who are HIV-negative, or who have not been tested, the presence of an STI is an important indication to trigger testing (or repeat testing). Because STIs and HIV infection frequently co-exist and are transmitted together, anyone seen for an STI should be offered HIV testing and counselling. So you should refer any patient presenting with STIs for HIV counselling and testing services.
31.2 Transmission and risk factors for STIs
31.2.1 Transmission of STIs
Now you are going to learn about how STIs are transmitted from one person to another person. As the name implies, by far the most common mode of transmission of STIs is sexual transmission. The modes of transmission could be vaginal or anal sex. In Ethiopia, most STIs in relation to sexual transmission are through the vaginal route (though cases of anal transmission are also common). Heterosexual (sexual intercourse with an individual of the opposite sex) transmission is the most common mode of transmission of STIs. Another mode of transmission is mother-to-child during pregnancy (e.g. HIV and syphilis), at delivery (e.g. gonorrhoea and chlamydia), and during breastfeeding (e.g. HIV). Rarely STIs can also be transmitted through unsafe use of unsterile needles or injections, or coming in contact with contaminated blood or blood products (e.g. syphilis, HIV and hepatitis).
From your previous studies, what are the common modes of transmission of HIV in Ethiopia?
Sexual transmission is by far the most common mode of transmission; next comes transmission of HIV from mothers to children.
31.2.2 Risk factors for STIs
There are a number of factors that increase the risk of transmission of STIs, including biological, behavioural and socio-cultural factors. In this section we will be discussing the major risk factors that are associated with the transmission of STIs. Understanding these factors will help you in identifying the factors that promote STIs and their relation to the most ‘at risk’ groups of the population affected by STIs. In your daily assessment you will utilise this knowledge to assess patients and give them health education and counselling support in order to prevent STIs.
Biological factors
Biological factors are related to the age, sex and immune status of an individual. Certain age groups of the population are known to have a high prevalence of STIs.
Women in general are at greater risk of HIV transmission than men due to the larger vaginal surface area that comes in contact with the penis during sexual intercourse. In particular, young women between 15 and 24 years old, and women going through the menopause, are at high risk of acquiring STIs. Young women also may not have a comprehensive knowledge of STIs transmission. In addition, the risk of transmission of STIs is high in these groups due to immature or weakened vaginal mucosal lining of young and menopausal women, respectively.
The immune status of an individual also determines the risk of STIs. People with weak immunity have a greater risk of acquiring STIs than individuals who have a healthy immune system.
Behavioural factors
Behavioural factors are associated with actions of individuals towards a certain situation, in this case their sexual behaviour. It is well known that certain risky behaviours expose people to the transmission of STIs. These factors include having more than one sexual partner or having sex with ‘casual’ partners, for instance sex workers or their clients. One of the main risk behaviours that promotes transmission of STIs is unprotected sexual intercourse, that is sex without using a condom. Proper use of condoms effectively prevents the transmission of STIs; hence you should educate your clients at health post level, or in the community, about the proper use of condoms (Study Session 25). Changing sexual partners frequently is also a behavioural risk factor.
The use of alcohol, stimulants like ‘khat’ or illegal drugs may negatively affect the proper use of condoms. They usually affect our ability to weigh up risky situations and may result in involvement in unsafe sexual acts.
Socio-cultural factors
These are factors that indirectly affect the ability of individuals to take an independent responsibility for their behavioural actions. For example, factors like gender bias of a community, women’s economic dependence on men, and young marriage, affect women indirectly to be exposed to the transmission of STIs more than men. Harmful traditional practices like tattoos and unsterile circumcisions are also associated with contracting of STIs directly from the sharp materials that are used for that purpose.
31.2.3 Epidemiology of STIs in Ethiopia
There is little information on the incidence and prevalence of STIs in Ethiopia. The prevalence of HIV has been mentioned in Study Session 20 and that of syphilis is thought to be about 2.7% (FMOH, 2006). There is no actual information or estimate on other STIs in Ethiopia. This is because reports often under-represent the true number of people infected with STIs. As you can imagine the reasons are many, but a major contributing factor is that people with STIs who have minor or no symptoms do not seek treatment at public health facilities. They usually tend to take self-prescribed drugs or go to private pharmacies to buy treatment without consulting trained health workers.
Another contributing factor to the lack of information on STIs is also irregular access to treatment; that is health facilities offering treatment for STIs may be too far away from clients who present with STIs. Stigma associated with attending public STI clinics is also a factor in that clients tend to shy away from being seen at STI clinics. As noted above, many patients may then choose to go to alternative providers like pharmacies and traditional healers that do not report formally to the Federal Ministry of Health.
The formal public health facilities also do not report all STI cases properly and comprehensively for data to be compiled nationally. Last but not least some patients also do not attend formal STI clinics due to economic factors and they would rather go to traditional healers that provide services for free or with cheap costs.
31.3 Presentation of common STIs
In this section you will study the clinical presentations of common STIs caused by bacteria, viruses or protozoa. The clinical signs and symptoms of common STIs described below will help you to reasonably identify STIs. Now let us describe them.
All the photos in Figures 31.1 to 31.5 are taken from the Ethiopian Adaptation, 2007, of the WHO/IMAI Guidelines acknowledged at the front of this Module.
31.3.1 STIs caused by bacteria
Gonorhoea
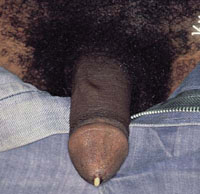
Gonorhoea is one of the most common STIs and is caused by bacteria called Neisseria gonorrhoeae. Men with gonorrhoea may present with a burning sensation while urinating and a discharge from the urethra (Figure 31.1), whereas women may present with vaginal discharge and lower abdominal pain. A discharge is a yellowish or whitish substance released from the opening of the reproductive tract in both men and women. Most men infected with gonorrhoea have symptoms, but in women gonorrhoea is commonly asymptomatic (i.e. they do not have any symptoms). Women who have gonorrhoea (with or without symptoms) can transmit the bacteria to infants during birth. In newborn babies, gonorrhoea usually presents with eye disease (termed neonatal conjunctivitis) and can lead to blindness.
What can you see in Figure 31.1? What could be the possible cause?
A whitish discharge from the opening of the penis can be seen; the likely clinical diagnosis is gonorrhoea.
Chlamydia
Chlamydia is also one of the most common (if not the commonest) STIs, and is caused by bacteria called Chlamydia trachomatis. In men it usually presents with discharge from the urethra and in women it presents with cervicitis (inflammation of the neck of the womb or cervix) and lower abdominal pain. The discharge is generally less ‘sticky’ and lighter in colour than for gonorrhoea. Chlamydia, like gonorrhoea, can also be asymptomatic, but in this case in both men and women. In addition, pregnant women with chlamydia can also transmit the STI to their babies during childbirth and cause neonatal conjunctivitis.
Syphilis
Syphilis is caused by bacteria called Treponema pallidum. Syphilis has four stages: primary, secondary, latent and tertiary syphilis, with different signs and presentations according to the time passed from the initial infection. The different stages can be described as follows:
- Primary syphilis is characterised by a painless ulcer (known as chancre) in the genital or anal area resulting from direct sexual contact with a person with syphilis. The chancre has obvious edges, and the lymph nodes in the groin may also appear swollen. Primary syphilis takes 10 to 90 days to develop from initial exposure to the bacterium.
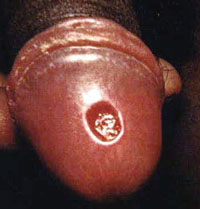
Describe what you see in Figure 31.2. What could be the most likely diagnosis?
A solitary ulcer with clear edges on the penis. The possible diagnosis is primary syphilis.
- Secondary syphilis is characterised by a non-itchy rash over the trunk and the extremities, arising 1 to 6 months after primary syphilis.
- Latent syphilis is the stage between secondary and tertiary syphilis in which an infected patient shows few or no symptoms.
- Tertiary syphilis is a rare phenomenon characterised mainly by soft tumour-like balls of inflammation under the skin, or on bones, that may appear anywhere in the body. Some individuals with tertiary syphilis may show serious neurological (nervous system) or cardiovascular problems (heart and blood vessels). Tertiary syphilis takes 1 to 10 years to develop, but it can take up to 50 years.
Chancroid
Chancroid is caused by bacteria termed Haemophilus ducreyi and in the majority of cases it presents with painful ulcers and sores in the genital area (particularly in the foreskin of the penis). Many patients also develop a bubo, an enlargement of the lymph nodes on one side of the groin that exudes liquid. By contrast, most infected women do not show any symptoms.
Granuloma inguinale
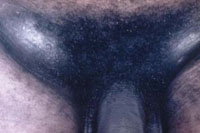
Granuloma inguinale is caused by an infection with bacteria called Calymmatobacterium granulomatis. It presents initially with small lesions in areas surrounding the anus and/or genitals, which are difficult to differentiate from chancroid, but then turn into ulcerative lesions and lead to painless raised solid bumps in both sides of the groin area (Figure 31.3).
31.3.2 STIs caused by viruses
HIV, the virus that causes AIDS, has been dealt with extensively in previous study sessions. Here we will focus on other STIs caused by viruses.
Herpes genitalis
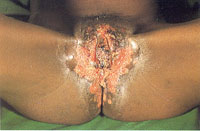
Herpes genitalis is the most common STI caused by a viral infection. The pathogen responsible for genital herpes is Herpes simplex virus type 2 (HSV-2). Genital herpes usually presents with blisters that, when they break, lead to painful sores and ulcers in the outer surface of the genitals and in areas surrounding the anus. Following initial infection, it may take around 2–4 weeks for the lesions to heal, but symptoms usually recur weeks or months after the first outbreak. Although geneital herpes may affect anyone, if it involves an extensive area of the genitals and persists for longer than a month as seen in Figure 31.4, you should suspect an HIV-related opportunistic infection. Hence you should offer or refer these patients for provider-initiated HIV testing and counselling if their HIV status is unknown.
Genital warts
Genital warts is a viral STI caused by human papilloma virus (HPV) and commonly presents with small fleshy growths of skin on the genital area or around the anus (Figure 31.5). HPV has also been shown to be the causative agent of cervical cancer in women. However, the types of HPV that cause genital warts are not the same as the types that can cause cancer, which is usually asymptomatic for years.
Cancers (including cervical cancer) are covered in Study Session 3 of the Non-Communicable Diseases, Emergency Care and Mental Health Module.

31.3.3 STI caused by a protozoan
Trichomoniasis is a STI caused by a protozoan that is usually found in vaginal and urethral tissues. It presents in women with profuse and frothy vaginal discharge. Although this condition is most often treated in women, men can also be infected but often show no symptoms.
31.3.4 STI caused by a fungus
Vaginal candidiasis is a vaginal infection caused by a fungus termed Candida albicans. The main symptoms of candidiasis in women are a curd-like vaginal discharge, vaginal itching and sometimes a burning sensation.
From Study Session 21, which opportunistic infection in PLHIV is caused by the same organism that causes vaginal candidiasis?
Oral thrush in HIV-positive people is also caused by Candida albicans.
31.4 Syndromic management of STIs
A syndrome is a group of symptoms that patients describe, combined with classic signs that health workers observe during clinical assessment. A number of different organisms that cause STIs give rise to a limited number of syndromes.
Now that you have studied about how common STIs present, in this section you will learn about how to group similar STI together and manage them. You should identify and classify patients into syndromes for effective management of their condition.
31.4.1 Classification of patients into syndromes
Using the syndromic approach, health workers at health centres and hospitals can identify one of these syndromes and treat accordingly. The objective of introducing you to syndromic management of STIs is to help you identify and refer cases to the nearest health centre. At this moment you are not expected to treat STI cases either at the health post or in the community. In the health centre the patient will receive all necessary services including testing for HIV. Table 31.1 shows a modified summary version of syndromic management of the common STIs described in Section 31.3 and others. For detailed reading you can refer to the Ethiopian National Syndromic Management of STIs Guideline.
| Syndrome | Signs and symptoms | Most common causes | Management |
|---|---|---|---|
| Vaginal discharge | Unusual vaginal discharge, vaginal itching, dysuria (pain on urination and pain during sexual intercourse) | Trichomoniasis Bacterial vaginosis | Refer to health centre |
| Candidiasis | Refer to health centre. Consider HIV-related illness if it is recurrent | ||
| Gonorrhoea Chlamydia | Refer to health centre Counsel and refer for HIV and syphilis testing Include partner tracing | ||
| Urethral discharge | Urethral discharge, dysuria, frequent urination | Gonorrhoea Chlamydia | Refer to health centre Offer HIV testing and counselling and refer for syphilis testing Consider HIV-related illness Consider partner tracing |
| Genital ulcer | Genital sore | Syphilis, Chancroid | Refer to health centre Promote and provide condoms Consider HIV-related illness; offer HIV testing and counselling Educate on STIs, HIV and risk reduction |
| Genital herpes | Refer to health centre | ||
| Lower abdominal pain | Vaginal discharge, fever, lower abdominal pain and tenderness | Gonorrhoea Chlamydia, | Refer to health centre. Consider HIV-related illness Consider partner tracing |
| Scrotal swelling | Pain and swelling of the scrotum | Gonorrhoea Chlamydia | Refer to health centre. Consider HIV-related illness Consider partner tracing |
| Inguinal bubo | Painful enlarged lymph nodes on the groin | Lymphogranuloma venerum (LGV) Chancroid | Refer to health centre Consider HIV-related illness; offer HIV testing and counselling Educate on STIs, HIV and risk reduction |
| Neonatal conjunctivitis | Swollen eyelids, eye discharge in newborns and infants | Gonorrhoea Chlamydia | Refer to the nearest health centre for management |
31.4.2 Treatment and management of STI syndromes
The aim of syndromic management is to identify the seven syndromes listed in Table 31.1 and manage them accordingly. While clinical diagnosis is based on identifying just one specific causative agent, syndromic diagnosis leads to immediate treatment for all of the most important possible causative agents. This is important because mixed infections occur frequently in STIs. Besides, syndromic management of STIs can effectively treat cases in settings with limited laboratory capacity like health posts and health centres. This means that, if necessary drugs are available and affordable, syndromic treatment can quickly render the patient non-infectious.
Therefore the key features of syndromic case management of STIs are first that it is problem-oriented, i.e. it responds to the patient’s symptoms; second, it is efficient in identifying the causes of STIs; and third, it does not miss multiple infections caused by different pathogens.
Syndromic management also makes treatment and control services for STIs more accessible to patients as it can be implemented at health centre level. For example, syndromic management offers a good opportunity to provide health education and HIV testing and counselling during any encounter with STI cases.
In managing STI cases using syndromic management, the health worker is guided through logical steps of clinical decision-making. The following four steps are to be followed:
- Assessing patients for symptoms, signs and risk factors.
- Syndromic diagnosis and treatment.
- Education and counselling on HIV testing and safer sex, including condom use, promotion and provision.
- Management of sexual partners, in your case tracing sexual partners.
A patient complains of a discharge from the penis. Upon examination, you notice a discharge from the urethra. What syndrome does the sign and symptoms suggest? What action should be taken, and why?
Urethral discharge syndrome is suggested. It is commonly caused by gonorrhoea and/or chlamydial infection. Not only can these cause serious complications, but also they can facilitate the transmission and acquisition of HIV. It is therefore essential that we treat the patient for both.
A young woman complains of a sore on her vulva. Upon examination you notice an ulcer on the outer labia. What syndrome does the sign and symptoms signify? What are the possible causes?
This indicates the syndrome of genital ulcer. There are two main bacterial causes of genital ulcer: chancroid and syphilis.
31.5 Common complications of STIs
In this section we will just briefly describe the common complications of STIs. You have to note that complications of STIs have huge health, social and economic implications. Therefore your active identification and referral of STIs cases in the community greatly reduces the burden associated with them. Table 31.2 summarises the common complications of STIs with their respective causes.
| STI infection | Complication |
|---|---|
| gonococcal (gonorrhoea) and chlamydia infection |
|
| gonocchocal infection (gonorrhoea) | Conjunctivitis and blindness in infants |
| human papilloma virus | Genital or cervical cancer |
| chlamydia, gonorrhoea, herpes virus and trichomoniasis bacteria | Increased transmission of HIV from genital inflammations due to the cuts, tears, abrasions that would expose the genital mucosa to HIV. |
31.6 STIs and HIV
Remember that you have learned that HIV is sexually transmitted in Study Session 20. HIV infection is therefore a STI but due to its high priority as a general health concern it has been dealt with separately in this module. In this section you will learn about the relationship between HIV and other STIs. It is important that you remember that HIV is transmitted in the same ways as any other STIs. There are strong links between having an STI and becoming HIV-positive. STIs increase the risk of HIV transmission and HIV infection may make people more susceptible to other STIs and even make other STIs more difficult to treat. These observations make it even more urgent to prevent and control STIs.
31.6.1 The link between STIs and HIV/AIDS
Certain STIs facilitate the spread of HIV. The following three points generally describe the relationship between HIV and other STIs:
- Certain STIs facilitate the transmission of HIV through the small cuts and inflammations they cause around the genitalia.
- The presence of HIV can make people more susceptible to the transmission of STIs. This is because HIV weakens the immunity that can protect us from other infections like STIs.
- The presence of HIV increases the severity of some STIs and makes them more difficult to treat than in HIV-negative individuals. This is also related to the poor immunity of PLHIV.
31.6.2 Which STIs facilitate the transmission of HIV?
A person with open sores in the genital area is much more likely both to contract and to transmit HIV. Chancroid and syphilis are the main bacterial causes of sores: if they are correctly diagnosed and treated, these routes of HIV transmission can be reduced. Genital herpes also facilitates HIV transmission. Genital herpes causes recurrent genital ulcers. An ulcer in the genital area provides an open door, through which HIV can easily pass. Chlamydia, gonorrhoea and trichomoniasis can also facilitate the transmission of HIV although they do not cause sores. This may be due to the fact that genital inflammation associated with these STIs can cause microscopic cuts in genital tissues, creating potential sites where HIV can enter the body.
31.6.3 HIV increases the risk of infection with other STIs
It is also true that people infected with HIV are more vulnerable to getting multiple infections. This is because changes in their body’s immunity make them more vulnerable to infection by pathogens in general.
31.6.4 Key issues regarding STIs and HIV infection
You need to keep in mind the following essential points about the relationship between HIV and STIs. Firstly, an obvious point in common between STIs and HIV is behavioural. For example, unprotected sexual behaviour exposes people to both HIV and other STIs as you learned in Section 31.2.1 and elsewhere in this Module. Equally, the consistent use of condoms can prevent both kinds of infection. So, you need to educate and counsel your clients about the proper and consistent use of condoms to reduce the risk of transmission of both HIV and other STIs.
Secondly, STI control is also important for preventing the spread of HIV from PLHIV, which you learned in Study Session 29 on positive living. PLHIV are more likely to transmit HIV to others if they also have another STI. PLHIV should thus be taught how to recognise STI symptoms and be encouraged to seek care promptly if they think they may have an infection.
Note that all STI cases that you identify at your health post and in your community have to be referred to the nearest health centre for treatment. In the health centre, STI treatment should be provided along with the following key interventions:
- Educating clients about the transmission, treatment and control of STIs and HIV
- Providing risk reduction counselling by focusing on the prevention of STIs and HIV
- Condom promotion and provision for all clients
- Consideration of HIV-related illness and offering provider-initiated counselling and testing
- Partner counselling and treatment: management of partners for STIs is an essential component of STIs to stop further recurrent infection among partners
- Encouragement for HIV testing through provider-initiated counselling
- Referral of patients and their partners to counselling units and laboratories for HIV and syphilis testing, or to higher health care if they do not respond to syndromic treatment of STIs.
Why do STIs increase the risk of HIV transmission? List three STIs that can increase the risk of HIV transmission.
It is due to the fact that genital inflammation associated with STIs can cause small cuts in genital tissues, creating potential sites where HIV can enter the body. Examples of STIs that increase the transmission of HIV are genital herpes, syphilis and gonorrhoea.
Summary of Study Session 31
In Study Session 31, you have learned that:
- STIs are very common communicable diseases in the community.
- The transmission of STIs is greatly affected by demographic, social, biological, economic and behavioural factors.
- Syndromic management of STIs is an important tool to simplify the diagnosis and treatment of STIs. It involves treating all possible causes, even though the specific infectious agents have not been identified.
- HIV testing and counselling is an essential component of STI management.
- The risk of HIV transmission increases when an individual has concurrent and untreated STIs. The presence of HIV increases the severity of some STIs and makes them more difficult to treat.
Self-Assessment Questions (SAQs) for Study Session 31
Now that you have completed this study session, you can assess how well you have achieved its Learning Outcomes by answering the following questions. Write your answers in your Study Diary and discuss them with your Tutor at the next Study Support Meeting. You can check your answers with the Notes on the Self-Assessment Questions at the end of this Module.
SAQ 31.1 (tests Learning Outcomes 31.1 and 31.2)
- a.List all routes of transmission of STIs and give two examples for each.
- b.Explain why the risk of transmission of STIs is greater in women than in men.
Answer
- a.The following are the common routes of transmission of STIs, together with two typical examples.
- Sexual: e.g. HIV, gonorrhoea
- Mother to child: e.g. HIV, chlamydia
- Unsafe injections and blood transfusion: e.g. HIV, syphilis.
- b.The risk of transmission of STIs is higher in women than men mainly due to biological and socio-cultural factors. Specifically, young women 15 to 24 years old and menopausal women are at higher risk of STIs. This is because young women usually lack comprehensive knowledge of STIs transmission. In addition, the risk of transmission of STIs is higher due to immature and weakened vaginal mucosal lining of young and menopausal women respectively. Also the surface area of the vagina that comes in contact during sexual intercourse is larger than that of the penis and this is associated with an increased risk of transmission. Socio-cultural issues like gender bias, economic dependence, societal values relating to sexuality and harmful traditional practices like female genital mutilation also contribute significantly to the increased risk of STIs in females.
SAQ 31.2 (tests Learning Outcomes 31.3, 31.4 and 31.6)
A 22-year-old young man came to the health post complaining of a yellow urethral discharge with burning pain on urination. He has had these complaints for the past five days.
- a.What syndrome does this young man present with?
- b.What will you do?
Answer
- a.The syndrome that this patient appears to have is urethral discharge.
- b.You need to refer him to the health centre urgently for further care and support. Provider-initiated testing and counselling can also be offered for HIV. You need to ask him about past sexual partner(s) so that they can be traced and encouraged to access screening for HIV or other STIs at the health centre.
SAQ 31.3 (tests Learning Outcome 31.4)
Explain why syndromic management of STIs is a feasible intervention in settings like Ethiopia.
Answer
Syndromic management of STIs enables health workers to treat similar causes all together. Syndromic diagnosis leads to immediate treatment for all of the most important causative agents of an STI. This is important because infections by multiple pathogens occur frequently in STIs. Besides, syndromic management can be implemented to effectively treat cases in settings with limited laboratory capacity such as health centres in Ethiopia.
SAQ 31.4 (tests Learning Outcome 31.5)
Explain how the presence of HIV can increase the risk of transmission of other STIs and vice versa.
Answer
The following points explain the relationship between HIV and other STIs:
- Certain STIs facilitate the transmission of HIV through the small cuts and inflammations they cause around the genitalia.
- The presence of HIV can make people more susceptible to the transmission of STIs. This is because HIV weakens the immunity that can protect us from other infections like STIs.
- The presence of HIV increases the severity of some STIs and makes them difficult to treat. This is also related to poor immunity in PLHIV.