Use 'Print preview' to check the number of pages and printer settings.
Print functionality varies between browsers.
Printable page generated Sunday, 3 May 2026, 4:31 AM
Communicable Diseases Module: 36. Louse-Borne Diseases: Relapsing Fever and Typhus
Study Session 36 Louse-Borne Diseases: Relapsing Fever and Typhus
Introduction
You already learned about the most widespread vector-borne disease in Ethiopia – malaria, transmitted by mosquitoes (Study Sessions 5 to 12 in Part 1 of this Module). Two other vector-borne diseases of public health importance in Ethiopia are the subject of this study session: they are caused by different bacteria, but are transmitted by the same vector – the human body louse (plural, lice). The diseases are louse-borne relapsing fever and louse-borne typhus, which are classified as febrile illnesses because the symptoms always include high fever. In this study session, you will learn about the causes, modes of transmission, symptoms and methods of prevention of these diseases. This will help you to identify patients and quickly refer them to the nearest health centre or hospital for specialist treatment. You are also expected to report any cases of these louse-borne diseases to the District Health Office, so that coordinated action can be taken to prevent an epidemic from spreading in your community.
Learning Outcomes for Study Session 36
When you have studied this session, you should be able to:
36.1 Define and use correctly all of the key words printed in bold. (SAQs 36.1 and 36.3)
36.2 Describe the vector and the modes of transmission of relapsing fever and typhus, and the conditions in which epidemics are most likely to occur. (SAQs 36.1 and 36.3)
36.3 Describe the symptoms of relapsing fever and typhus, and the actions you should take if you identify a suspected case. (SAQs 36.3 and 36.4)
36.4 Explain how you would apply effective methods to prevent and control relapsing fever and typhus. (SAQs 36.2, 36.3 and 36.4)
36.1 The human body louse
Before we discuss relapsing fever and typhus, it is first helpful to describe the vector of both these diseases. The human body louse (species name, Pediculus humanus humanus) is commonly found in the clothes, bedding and on the bodies of people living in overcrowded and insanitary conditions, where there is poor personal hygiene. When body lice are found, for example in clothes, the articles are said to be louse-infested. (Note the term is infested, not infected.)
Can you suggest examples of places where louse infestation is more likely to occur because of overcrowding and lack of sanitation?
You may have suggested refugee camps (Figure 36.1), badly maintained prisons or army camps during times of war.
 Figure 36.1 Overcrowding and poor sanitation create perfect breeding sites for body lice.
Figure 36.1 Overcrowding and poor sanitation create perfect breeding sites for body lice.
Male and female lice mate and the female lays eggs (known as nits), which she attaches to body hairs or fibres in clothing and bedclothes where people sleep (Figure 36.2). The eggs hatch into small immature lice (called nymphs), which bite their human hosts to suck blood, nourishing their growth and development into adult lice (Figure 36.3). They have a lifespan of only a few weeks, and feed at frequent intervals. The bites cause an allergic reaction in the person’s skin, which becomes inflamed and itches, causing the person to scratch the area. Lice are transmitted from person to person during close contact and when sharing bedding in which eggs have been laid. They can survive for only a few days off the human host.


Although human body lice can transmit relapsing fever and typhus, the modes of transmission are somewhat different in these two diseases, as you will see in the following sections.
36.2 Louse-borne relapsing fever
Louse-borne relapsing fever (RF) is caused by spiral-shaped bacteria called Borrelia recurrentis. RF is common in Ethiopia, Sudan and Rwanda. It is one of the epidemic-prone diseases that can cause small- or large-scale epidemics anywhere in Ethiopia, with an estimated 10,000 cases annually. RF is more common in the highlands, where it occurs mainly in the rainy seasons, but in south west Ethiopia it occurs in dry and rainy seasons equally. Epidemics of RF are often associated with epidemics of typhus, since both are transmitted by the body louse in similar conditions of overcrowding and lack of hygiene.
36.2.1 Mode of transmission of relapsing fever
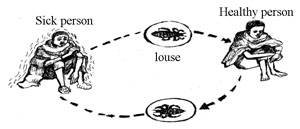
The bacteria that cause RF infect body lice when they take a blood meal from an infected person (Figure 36.4). The bacteria multiply in the gut of the louse, but the infection is not transmitted to new hosts when the louse bites a healthy person. Instead, humans acquire the infection when they scratch their bites and accidentally crush a louse, releasing its infected body fluids onto their skin. The bacteria enter through breaks in the skin, typically caused by scratching the itchy louse bites. After entering into the skin, the bacteria multiply in the person’s blood and they can also be found in the liver, lymph glands, spleen and brain.
36.2.2 Symptoms of relapsing fever
The incubation period between the infection and the start of symptoms is typically five to ten days. The common clinical manifestations of RF include the sudden onset of episodes of high fever, up to 40oC, with periods of shivering and chills, accompanied by headache, joint pain, dry cough and sometimes bleeding through the nose. About one third of patients develop tiny red or purple spots on the skin. The symptoms continue for three to nine days, while the immune system of the patient makes antibodies that attach to the bacteria and clear them from the blood, and the patient appears to recover. However, not all of the bacteria are destroyed. The numbers of bacteria gradually increase, and four to seven days after recovering from the first episode of fever, the patient ‘relapses’, i.e. the symptoms begin all over again. Almost all the organs are involved and there will be pain in the abdomen and an enlarged liver and spleen, in addition to the other symptoms. Without treatment with special antibiotics, 30% to 70% of cases can die from complications such as pneumonia and infection in the brain, leading to coma (a state of deep unconsciousness) and death.
What other disease that you have already learned about has similar episodes of fever, headache and chills, with periods of recovery and then relapse?
Malaria has similar symptoms to relapsing fever.
36.2.3 Actions if you suspect relapsing fever
![]() Immediately refer all patients with suspected relapsing fever.
Immediately refer all patients with suspected relapsing fever.
The similarity between the clinical manifestations of malaria and RF mean that you should first consider whether a diagnosis of malaria can be ruled out. If your community is in a malaria-endemic area, perform a malaria rapid diagnostic test (RDT) on the patient’s blood, as described in Study Session 7 of this Module. If there is no malaria in your area, or the RDT is negative, you should immediately refer a patient suspected of having RF to the nearest health centre or hospital.
The good news is that RF can be easily and successfully treated with special antibiotics, but these can only be prescribed by a doctor. You are not expected to prescribe drugs for relapsing fever. The symptoms usually begin to improve within 24 hours of starting the treatment. Make sure that the patient and the family know that RF can be life-threatening without treatment, but that it can be cured with the right medicine.
Lice carrying the bacteria that cause RF are very easily transmitted between close contacts of the infected person. Therefore, you should also do active case finding – searching actively for other cases of RF by asking about anyone with the characteristic symptoms in the patient’s family or village to detect if there could be an epidemic spreading. Precautions should be taken by you and by health workers in the hospital or health centre, to avoid close contact with a patient with relapsing fever, to prevent acquiring the infection.
36.3 Louse-borne typhus
You learned about typhoid fever in Study Session 33.
Typhus should not be confused with typhoid fever. Although there are some similarities between these two febrile illnesses, they are caused by different bacteria and typhoid is transmitted mainly in infected food, not by body lice.Louse-borne typhus (also known as epidemic typhus, ‘jail fever’ or tessibo beshita in Amharic) is similar in many ways to relapsing fever. Like RF, it is a bacterial infection transmitted by the human body louse, but the causative bacteria are different. They are extremely small bacteria called Rickettsia prowazekii (named after two doctors who died of typhus when they were researching into the disease). These bacteria quickly have to get inside the cells of their human host in order to survive and multiply – unlike the bacteria that cause RF, which circulate in the blood and don’t live inside the host’s body cells.
Louse-borne typhus has caused major epidemics over many centuries, resulting in millions of deaths during war, famine and mass displacement. The WHO estimates that globally in recent years around 1,400 people die from typhus every year. Like RF, outbreaks occur in situations of overcrowding in unhygienic conditions where body lice can easily breed and spread. Outbreaks of the disease have occurred in Ethiopia from time to time. Typhus is more common in the highlands, in places such as Gondar, Shewa, Bale, Arsi, Gojam and Tigray.
36.3.1 Mode of transmission of louse-borne typhus
There is one difference in how the Rickettsia bacteria that cause typhus, and the Borrelia bacteria that cause RF, are transmitted by body lice to new human hosts. The Rickettsia bacteria acquired during a blood meal from an infected person multiply in the gut of the louse and pass out of its body in the louse’s faeces, which are deposited on the person’s skin. These bacteria can survive for several days in the faeces. The louse bites are itchy and when the person scratches them, the louse faeces are rubbed into breaks in the skin. This is how the typhus bacteria are transmitted to healthy people when an infected louse gets into their clothes or bedding. They quickly enter the new host’s body cells and begin to multiply.
36.3.2 Symptoms of louse-borne typhus
The clinical manifestations of louse-borne typhus are similar to other common febrile illnesses in Ethiopia, including relapsing fever. After an incubation period of about one to two weeks the symptoms begin suddenly, with severe headache and fever rising rapidly to 38.8ºC to 40.0ºC. But unlike RF, the high temperature in typhus is sustained throughout the illness and the symptoms do not spontaneously improve and then relapse. A prominent cough is very common, occurring in 70% of patients. They also experience very severe muscle pain, sensitivity to light, lethargy and falling blood pressure. If untreated, the most severe cases end in coma and death.
36.3.3 Actions if you suspect louse-borne typhus
If you suspect a case of typhus, your actions should be exactly the same as already described for suspected cases of RF.
What should you do?
Test for malaria if you are in a malaria endemic area. Refer patients suspected of having typhus to the nearest health centre or hospital, where they will be treated by doctors with special antibiotics. You are not expected to prescribe these drugs. Typhus is an epidemic-prone disease, so search actively for other people locally with a similar illness and report all suspected cases to the District Health Office.
In addition to the above actions, you should also educate your community about how to prevent these louse-borne diseases. This is the subject of the final section of this study session.
36.4 Prevention of louse-borne relapsing fever and typhus
Let us now focus on the common prevention aspects of relapsing fever and typhus. As we said earlier, these diseases are associated with overcrowding and insanitary conditions – in other words, they are associated with poverty. They are best prevented by addressing the underlying socioeconomic circumstances that promote louse infestation: overcrowding, poverty, homelessness and population displacement. However, you should also educate people in your community to take the following preventive actions:
- Maintain good hygienic practices, such as washing the body, clothes and bedding regularly, and drying clothes and bedding in direct sunlight, which damages the lice and their eggs to some extent
- Change clothes and bedding at frequent intervals to reduce the number of body lice
- Treat louse-infested clothes and bedding with chemicals to kill the lice and their eggs (this is called delousing). In infested situations like those in refugee camps, clothes and bedding should be deloused by trained personnel with appropriate insecticides, such as 0.5% permethrin dust or DDT. You are not expected to apply these chemicals. Treating clothing with liquid permethrin can provide long-term protection against louse infestation.
Note that close contact with patients should be avoided and delousing of the patient’s clothes and bedding should be done immediately, to prevent transmission of infected body lice from the patient to healthy people – including the health workers who are caring for them.
If there is an outbreak of relapsing fever or typhus, the spread of infection can be controlled by active case finding and effective treatment of infected persons and their close contacts with the correct antibiotics. These drugs have to be prescribed and monitored by doctors – you are not expected to give any drugs to patients with RF or typhus. Early treatment controls the spread of infection by reducing the reservoir of bacteria in the local population.
In the next study session, we complete the discussion of vector-borne diseases by describing four that are of significant public health importance in Ethiopia.
Summary of Study Session 36
In Study Session 36, you have learned that:
- Louse-borne relapsing fever (RF) and typhus are major epidemic-prone diseases in Ethiopia. They are vector-borne febrile illnesses caused by bacteria and transmitted by the human body louse.
- RF and typhus are diseases of poverty and overcrowding, which are most likely to occur in refugee camps, prisons and other places where large numbers of people live in crowded conditions, with poor sanitation and lack of personal hygiene, which promote infestation with body lice.
- RF and typhus have similar symptoms, including high fever, headache, and joint and muscle pain. Patients with typhus often also have a persistent cough. The symptoms of RF typically occur in cycles of a few days, resolving spontaneously for a few days before the patient relapses with another episode of symptoms. Typhus symptoms tend to be sustained over time.
- Patients with RF or typhus should be referred immediately for antibiotic treatment in higher health institutions; both diseases are life-threatening if not treated, but respond well to the correct antibiotics.
- When you suspect a case of RF or typhus, you should conduct active case finding in the community to locate any similar cases; you can control the spread of an epidemic by referring all patients for early treatment, reporting cases to the District Health Office and seeking help to apply prevention measures.
- Regular washing of clothes, bedding and bodies, delousing using chemicals such as permethrin and DDT, and treatment with antibiotics are the major prevention and control methods during epidemics of RF or typhus.
Self-Assessment Questions (SAQs) for Study Session 36
Now that you have completed this study session, you can assess how well you have achieved its Learning Outcomes by answering the following questions. Write your answers in your Study Diary and discuss them with your Tutor at the next Study Support Meeting. You can check your answers with the Notes on the Self-Assessment Questions at the end of this Module.
SAQ 36.1 (tests Learning Outcomes 36.1 and 36.2)
- a.What are the similarities in how relapsing fever (RF) and typhus are transmitted from person to person?
- b.Can you describe one difference?
Answer
- a.The major similarity in the way that relapsing fever (RF) and typhus are transmitted from person to person is that the infectious agents of both these vector-borne diseases are transmitted by the human body louse. Lice acquire the causative bacteria when they take a blood meal from an infected person, and they transmit the bacteria to new hosts when people come into close contact with infected lice in clothes, bedding or on bodies. The bacteria causing both diseases multiply in the gut of the louse. The infection enters the new host through breaks in the skin, caused mainly by scratching the itching louse bites.
- b.One difference is that the bacteria that cause RF are transmitted in the fluids leaking from crushed lice, whereas the bacteria that cause typhus are transmitted in infected louse faeces.
SAQ 36.2 (tests Learning Outcome 36.4)
During your visit to a rural area, you observe that many people in a particular village wear dirty clothes and do not change their clothes for several weeks. What educational messages do you give the families in that village and what is your health education aiming to prevent?
Answer
There is poor personal hygiene in the village. Relapsing fever and typhus can quickly spread in such poor hygienic conditions if someone brings infected lice into the village on their body or clothes. You have to educate families to wash their clothes, bedding and bodies frequently to prevent diseases related to poor personal hygiene, particularly relapsing fever and typhus.
SAQ 36.3 (tests Learning Outcomes 36.1, 36.2, 36.3 and 36.4)
Which of the following statements is false? In each case, explain what is incorrect.
A It is possible to distinguish between relapsing fever and typhus at Health Post level by identifying differences in their symptoms.
B Relapsing fever and typhus occur only in the rainy seasons in Ethiopia.
C Treatment with the correct antibiotics is sufficient to control epidemics caused by relapsing fever or typhus.
D The correct antibiotics can effectively treat relapsing fever and typhus if the patient is referred immediately.
E Health workers should protect themselves from developing relapsing fever or typhus by avoiding close contact with patients with these diseases.
Answer
A is false. Relapsing fever and typhus have similar clinical manifestations such as fever, headache, joint and muscle pains. It is very difficult to distinguish between them by clinical manifestations alone, without laboratory investigations.
B is false. Relapsing fever and typhus can occur at any season if poor hygienic conditions and overcrowding encourage lice infestation.
C is false. Treatment with drugs is not sufficient to control an epidemic of relapsing fever or typhus. Health education about personal hygiene, and delousing clothes and bedding with chemicals such as permethrin, are other necessary control measures.
D is true. The correct antibiotics can effectively treat relapsing fever and typhus if the patient is referred immediately.
E is true. Health workers are at risk from close contact with patients with RF or typhoid because they can get the infection from the body lice of the patient; therefore, close contact should be avoided.
SAQ 36.4 (tests Learning Outcomes 36.3 and 36.4)
Estifanos is a 30-year-old farmer who came to your Health Post with fever, severe headache and extreme muscle pain. He tells you that there are many similar illnesses in his village.
- a.What are the possible diagnoses for Estifanos?
- b.What action do you take?
Answer
- a.Estifanos may have one of the febrile illnesses such as malaria, relapsing fever, typhus or typhoid fever.
- b.You should immediately refer him to the nearest health centre for further diagnosis and treatment. Visit his village to see the other sick persons and actively search for other cases, which you should immediately report to the District Health Office. There might be an epidemic of one of the febrile illnesses, which needs to be controlled by sustained preventive actions.