Use 'Print preview' to check the number of pages and printer settings.
Print functionality varies between browsers.
Printable page generated Saturday, 6 June 2026, 4:51 PM
Labour and Delivery Care Module: 11. Postpartum Haemorrhage
Study Session 11 Postpartum Haemorrhage
Introduction
Worldwide, every year, an estimated 127,000 women die as a result of blood loss following labour and delivery. It is the world’s leading cause of maternal mortality, accounting for a quarter of all maternal deaths. In total there are 14 million cases of haemorrhage occurring every year in association with pregnancy and childbirth, the majority of which are because failure of the uterus to contract properly after delivery of the placenta results in heavy bleeding or postpartum haemorrhage. In Study Session 6 you learned about the management of the third stage of labour, which begins with delivery of the baby and ends with delivery of the placenta and fetal membranes.
In this study session, you will learn about postpartum haemorrhage (PPH) and its management. PPH is one of the most alarming and serious emergencies in childbirth and your rapid actions can save many lives. Do not forget that antepartum haemorrhage (excessive bleeding before labour begins) can also threaten the life of the mother and fetus. You learned about early and late pregnancy bleeding in Study Sessions 20 and 21 of the Antenatal Care Module.
Can you recall the two most common causes of late pregnancy bleeding?
They are: placenta previa, when the placenta is close to or covering the cervix and it tears away as the cervix begins to efface and dilate as labour begins; and placental abruption, when the placenta is situated normally in the top two-thirds of the uterus, but it detaches before the birth of the baby.
Learning Outcomes for Study Session 11
When you have studied this session you should be able to:
11.1 Define and use correctly all of the key words printed in bold. (SAQ 11.1)
11.2 Describe the causes and risk factors for atonic and traumatic postpartum haemorrhage. (SAQ 11.2)
11.3 Describe interventions that can help to prevent postpartum haemorrhage, including actions during pregnancy and labour stages two and three. (SAQ 11.3)
11.4 Explain how you would provide emergency management for women who develop postpartum haemorrhage. (SAQ 11.3)
11.1 What is postpartum haemorrhage?
Postpartum haemorrhage (or PPH) is defined as excessive bleeding from the reproductive tract at any time following the baby’s birth and up to six weeks after delivery. Some 70–90% of PPH cases occur within the first 24 hours after delivery and are due to failure of the uterus to contract properly after the placenta detaches. Firm uterine contraction is necessary to close off the torn blood vessels in the placental bed.
Risk factors are existing underlying conditions which make a condition more likely to happen or more dangerous.
PPH is an unpredictable and rapid cause of maternal death. It is unpredictable in that two-thirds of women who develop PPH have none of the known risk factors (doctors refer to an adverse condition as idiopathic if there is no known reason why it occurred). In other cases, a woman with PPH does have one or more of the known risk factors (we review them later in this study session), or the PPH is due to mismanagement of the third stage of labour by the healthcare provider.
11.1.1 How much bleeding is ‘excessive’?
You learned how to measure blood pressure and pulse in Session 9 of the Antenatal Care Module; the causes and management of haemorrhagic shock were covered in Sessions 20–22 of that Module.
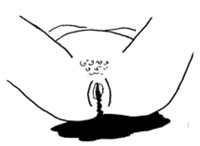
In normal births, the mother usually loses a small amount of blood (about 150 ml or a cupful) as the baby is born and after delivery of the placenta. When the amount exceeds 300 ml (2 cupfuls) it is considered as heavy bleeding (Figure 11.1). Excessive bleeding is often defined as more than 500 ml of blood loss. However, for severely anaemic women, blood loss of even 200–250 ml can be fatal. For that reason, a better definition of postpartum haemorrhage might be ‘any amount of bleeding that causes deterioration in the woman’s condition and signs of haemorrhagic shock’, i.e. low blood pressure, fast pulse, pallor, weakness or confusion).
11.1.2 Classification of postpartum haemorrhage
Postpartum haemorrhage can be classified based upon the timing of the bleeding following delivery of the baby and the cause of the bleeding.
Classifications based on the timing of bleeding are:
- Primary postpartum haemorrhage is excessive bleeding occurring during the third stage of labour, or within 24 hours of delivery.
- Secondary postpartum haemorrhage (also known as late postpartum haemorrhage) includes excessive bleeding occurring between 24 hours after delivery of the baby and 6 weeks postpartum.
Classifications based on the cause of the bleeding are termed either atonic or traumatic PPH. We will discuss each of these and their management in the next two sections.
11.2 Atonic postpartum haemorrhage
The word ‘atonic’ means ‘loss of muscular tone or strength to contract’. Atonic postpartum haemorrhage is characterised by excessive bleeding when the uterus is not well contracted after the delivery, and is soft, distended and lacking muscular tone.
More precisely, in atonic PPH, the myometrium (the muscle layer in the wall of the uterus) fails to contract and compress the maternal blood vessels that tear as the placenta pulls away from the wall of the uterus. Most bleeding after birth comes from the place where the placenta was previously attached. If the myometrium fails to constrict strongly, it cannot compress the blood vessels to control the bleeding.
11.2.1 Causes of atonic PPH
Any condition that interferes with uterine contraction, such as a retained placenta, remnants of placental tissue, or retained amniotic membranes or blood clots, increases the risk of excessive bleeding. If the placenta has separated but is still, even partially, in the uterus, it can prevent the uterus from contracting. Even a small piece of placenta or a blood clot left inside the uterus can keep it in the atonic condition. When the uterus is not contracted, the mother’s blood vessels continue to pump blood out and the woman will quickly lose blood.
The real problem with atonic PPH is that you cannot predict who will bleed excessively after the birth, and this is because two-thirds of women who develop atonic PPH have no known risk factors. This is why it is important to remember that all women must be considered at risk and prevention of PPH must be a part of every birth. The most important known risk factors are summarised below.
Interference with the ability of the uterus to contract
Note that while you cannot prevent an atonic uterus from occurring (nor can you always predict it), knowing the factors that make it more likely will help you to be alert to these possible signs of atonic PPH:
- Placenta previa or placental abruption: in both conditions the muscle fibres in the myometrium are damaged at the placental site.
- Retained placenta: this is when the whole or part of the placenta remains inside the uterus, interfering with the normal muscular contraction at the placental site.
- Incomplete separation of the placenta: this is when part of the placenta has separated from the uterine wall and part of it remains attached.
- Full bladder: the structural closeness of the uterus and the bladder means that a full bladder can interfere with the normal uterine contractions throughout labour and after delivery.
- High parity: this refers to a woman who has had more than five pregnancies; the muscles of the myometrium can lose their strength to contract firmly, due to repeated stretching.
- Multiple pregnancy: causes the uterus to increase its size to accommodate two or more babies (Study Session 10); following their delivery, the overstretched uterus may take a long time to contract firmly.
- Polyhydramnios: an excessive amount of amniotic fluid surrounding the baby (more than 3 litres) can overstretch the uterus in the same way as multiple pregnancy.
- Large baby: (over 4.0 kilograms) can also overstretch the uterus.
- Prolonged labour: when the labour extends more than 12 hours (Study Session 9), the muscles of the myometrium can become so exhausted by repeated contraction that they can no longer contract properly (uterine inertia).
Anaemia in the mother
Anaemia (lack of red blood cells due to low haemoglobin) puts the mother at greater risk of postpartum haemorrhage, because her blood does not clot as easily as in a non-anaemic person. Blood loss is also more serious in someone with anaemia. (You learned about the diagnosis and management of anaemia during pregnancy in Study Session 18 of the Antenatal Care Module.)
Mismanagement of the third stage of labour
Study Session 6 described how active management of delivery of the placenta should be conducted and what actions should be avoided.
What is the name given to the correct method of actively assisting delivery of the placenta?
It is called controlled cord traction.
What incorrect actions by the birth attendant during the third stage could result in postpartum haemorrhage?
Trying to deliver the placenta before it separates; pushing down on the fundus of the uterus while pulling on the umbilical cord; not waiting for a contraction before applying controlled cord traction and/or not applying counter-pressure to the mother’s abdomen. (Read Study Session 6 again if you are unsure of the steps in controlled cord traction.)
11.3 Traumatic postpartum haemorrhage
In traumatic postpartum haemorrhage, excessive bleeding occurs as a result of trauma (injury) to the reproductive tract following delivery of the baby. Trauma can occur to the cervix, vagina, perineum or anus. It could also be from a ruptured uterus (see Study Session 10). Signs of traumatic postpartum haemorrhage are when there is bleeding from the vagina but the uterus is well contracted (hard).
Trauma to the reproductive tract is preventable through skilled and gentle management during delivery, and referring the mother in good time if the labour is prolonged, or if the fetus is in an abnormal presentation or malposition (Study Session 8).
11.4 Reducing the risk of postpartum haemorrhage
In this section we briefly review the actions you can take at different stages to reduce the risk of postpartum haemorrhage occurring – beginning with a pregnant woman before labour starts.
11.4.1 Interventions during antenatal care
You should arrange for women with known risk factors (as described above for atonic PPH) to give birth in a health facility, where the risk of PPH can be more easily managed and urgent action taken if it occurs. In some cases (e.g. of placenta previa, malpresentation or twins), the baby may have to be delivered by caesarean surgery. There are many reasons why women may not want to go to a health facility, and it is important that you explain clearly and sensitively to mothers who are at increased risk why it is not safe for them to give birth at home. If they refuse, make sure that an emergency referral plan is in place and that potential blood donors are ready in case the woman needs a blood transfusion.
The high risk of PPH associated with anaemia is one reason why you should screen routinely for anaemia at every antenatal (and postnatal) visit, and take action to prevent it.
What should you do to prevent anaemia in the pregnant women in your care?
Counsel them on good nutrition with a focus on available iron-rich and folate-rich foods (e.g. dark green leafy vegetables, whole grains, red meats, eggs) and provide iron/folate supplements.
You learned how to do this in the Antenatal Care Module as part of focused antenatal care (Study Session 13), nutrition in pregnancy (Study Session 14), and the prevention and treatment of anaemia (Study Session 18).
What actions should you take to prevent anaemia caused by malaria and hookworm?
Encourage the use of insecticide-treated bed nets as protection against being bitten by the mosquitoes that transmit the malaria parasite. Provide treatment (mebendazole) after the first trimester of pregnancy in areas of high hookworm prevalence.
Malaria and hookworm are covered in detail in the Communicable Diseases Module.
11.4.2 Interventions during the second stage of labour
- Use a partograph to monitor and manage labour and prevent prolonged labour (see Study Session 4 of this Module).
- Encourage the woman to keep her bladder empty.
- Do not encourage pushing before the cervix is fully dilated.
- Do not apply fundal pressure (pressing on the top of the uterus) to assist the birth of the baby.
- Assist the woman in the controlled delivery of the baby’s head and shoulders to prevent tears (see Study Session 3 of this Module). Place the fingers of one hand against the baby’s head to keep it flexed (bent), support the perineum with the other hand, and teach the woman breathing techniques to push or to stop pushing.
11.4.3 Interventions during and after the third stage of labour
For women with no known risk factors, you can reduce the risk of PPH by correct and careful management of the third stage of labour, as described in Study Session 6. In summary, the main points to remember are as follows:
- After delivering the baby (and checking that there is no other baby left behind in the uterus), give the woman misoprostol 600 µg (micrograms) by mouth, or oxytocin 10 IU (international units) by intramuscular injection to help the uterus to contract.
- Do not apply fundal pressure to assist the delivery of the placenta.
- Rub the uterus immediately after the placenta is delivered, and at least every 15 minutes for the first 2 hours after birth to keep the uterus well-contracted. Teach the woman to massage and check her own uterus to keep it firm, and tell her to call for assistance if it is soft or if bleeding increases (Figure 11.2).

- Do a careful inspection for lacerations of the vagina, perineum and anus.
- Do a careful inspection of the placenta to ensure that it is intact (Study Session 6 showed how to do this).
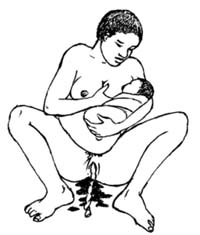
- Help the mother to breastfeed the baby immediately after it is born – even before the placenta has delivered (Figure 11.3). When the baby sucks, the mother’s body makes its own oxytocin, which stimulates the uterus to contract at the same time as it stimulates the milk ducts to contract and let down milk into the baby’s mouth. Breastfeeding helps to deliver the placenta and reduce postpartum bleeding.
- Encourage the woman to empty her bladder immediately after the birth. The uterus may stay soft because the mother’s bladder is full. If she cannot urinate help her by trickling warm water over her abdomen. If this does not work, she may need to have a catheter (a plastic tube) put into her bladder to help her urinate.
You learned the principles of urinary catheterisation in Study Session 22 of the Antenatal Care Module and your practical skills training.
There are interventions you can make before, during and after labour which may help to reduce the risk of PPH. Quickly see how many of these you can list.
To check how well you answered, re-read Sections 11.4.1, 11.4.2 and 11.4.3 of this study session.
However, remember that even if you make all the interventions possible, postpartum haemorrhage can still occur unpredictably after any delivery and you should always be prepared to take emergency action, as described next.
11.5 Emergency management of postpartum haemorrhage
If the mother begins to bleed excessively after the delivery, you must take action quickly to transport her to the nearest health facility. Postpartum haemorrhage can kill her and many healthcare providers underestimate how much blood a woman loses. If you face such a problem your first action should be to shout for help so the woman’s family or neighbours come to help you take her to the nearest health facility (Figure 11.4).

11.5.1 Uterotonic drugs and IV fluids to manage atonic PPH
If the mother is bleeding heavily, while you are waiting for the emergency transport, give her a second dose of oxytocin 10 IU by intramuscular injection, or a second dose of misoprostol 400 µg rectally (by pushing the tablets gently into the rectum through the woman's anus), or by putting the tablets under her tongue where they can slowly dissolve. Do not give additional misoprostol if oxytocin was the drug used originally.
Do not exceed 1,000 µg of misoprostol! If you gave 600 µg orally straight after the baby was born, the second dose should be no more than 400 µg rectally.
If you have been trained to do so, begin pre-referral infusion of intravenous (IV) fluids to prevent and treat shock. Infuse Normal Saline 9% or Ringer’s Lactate solution, set with the fastest possible flow rate. Ensure that the bag of IV solution is held higher than the woman’s head all the time, including when she is being transported to the nearest health facility.
You learned the principles of IV fluid infusion in Study Session 22 of the Antenatal Care Module and your practical skills training.
11.5.2 Use two-handed pressure on the uterus
If bleeding is very heavy and rubbing the uterus does not stop the bleeding, try two-handed pressure on the uterus (see Figure 11.5). Scoop up the uterus, fold it forward, and squeeze it hard (you will be shown how to do this in your practical skills training). Cup one hand over the top of the uterus. Put your other hand above the pubic bone and push the uterus towards your cupped hand. You should be squeezing the uterus between your two hands.
If you have been trained to do so, you can apply two-handed uterine compression by inserting one gloved hand inside the vagina and clenching your hand behind the cervix, while the other hand is pressing on the abdomen to compress the uterus.
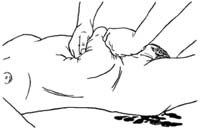
As soon as the bleeding slows down and the uterus feels firm, slowly stop the two-hand pressure. If bleeding continues, refer the woman to the nearest health centre facility. Try to keep two-handed pressure on the uterus while you are transporting the mother. Do not leave the baby behind – have someone carry it. Make sure you take possible blood donors from her relatives with you as the woman may need a blood transfusion.
11.5.3 Emergency management for traumatic PPH
Try to slow the bleeding from an injury (e.g. a tear in the perineum or vagina) by applying pressure over the source of the haemorrhage. Roll up 10 to 15 pieces of sterile gauze or a small, sterile cloth into a thick pad and push it firmly against the bleeding part of the tear. Hold it there for 10 minutes. Carefully remove the gauze and check for bleeding. If the tear is still bleeding, press the gauze against the source of the haemorrhage again and take the woman to the nearest health facility. Do not stop pressing on the tear until you get to there. If the woman has a long or deep tear, even if it is not bleeding much, take her to a health facility where it can be repaired.
11.6 A checklist for emergency referral
Finally, as we come to the end of this Module on Labour and Delivery Care, Table 11.1 summarises some key points to remember during emergency referral for postpartum haemorrhage, or any of the other life-threatening emergencies described in earlier study sessions. In the next Module, the continuum of care moves forward to the conduct of Postnatal Care.
| Aim to maintain: | Actions |
|---|---|
Contraction of the uterus | Apply gentle uterine massage, or two-handed compression of the uterus, and maintain this during referral |
Empty bladder | If the woman cannot urinate, insert a self-retaining catheter to drain the bladder and leave it in place during referral |
Adequate blood volume | If the woman is haemorrhaging or in shock, administer intravenous fluids and maintain the infusion during referral |
Vital signs | Check colour, pulse, blood pressure, temperature, blood loss, level of consciousness |
Warmth | Cover the woman with blankets |
Position | The woman should lie flat, but with her legs raised above the height of her head to help maintain her blood pressure |
Confidence | Give the woman your emotional support and reassurance; keep her as calm as possible |
Accurate records and referral note | Write down all your findings and the interventions you are making on the referral note, with the woman’s history and identification details |
What are the two most important points to remember about PPH?
You should remember that:
- Although some risk factors are associated with PPH, two thirds of women who develop PPH have no known risk factors. Which women will develop PPH is therefore highly unpredictable.
- Because of this you need to be alert to the possibility of PPH for every woman in your care who gives birth. And because PPH is life-threatening you must be ready to take appropriate emergency action, including getting her as quickly as possible to a health facility.
Summary of Study Session 11
In Study Session 11, you have learned that:
- Postpartum haemorrhage (PPH) is one of the leading causes of maternal death in developing countries. It is difficult to predict which women will develop PPH, so you should be prepared to deal with it at every birth.
- PPH can be prevented to a great extent by skilled care during pregnancy, labour and delivery, and the immediate postpartum period.
- During antenatal care, all pregnant women should receive advice about diet and malaria prevention, treatment for hookworm, and iron/folate supplements to prevent anaemia, which is a risk factor for PPH.
- Refer early if labour is prolonged and control the delivery of the baby’s head during second stage to prevent traumatic PPH.
- After delivery of the baby, give misoprostol or oxytocin to prevent atonic PPH, and massage the uterus after delivery of the placenta.
- If PPH develops, identify the cause of the bleeding. If due to atonic uterus (with or without with retained placenta), massage the uterus using two-handed pressure, empty the bladder (using a catheter if necessary), secure an IV fluid infusion, and administer either a second dose of oxytocin 10 IU by intramuscular injection, or a second dose of misoprostol 400 µg rectally or by putting the tablets under her tongue.
- If PPH is due to trauma, apply firm pressure to the source of the bleeding with a sterile pad for 10 minutes. If bleeding continues, reapply the pressure and refer the woman to a health facility where the tear can be repaired.
- When you need to arrange referral to a health facility, stay with the mother, checking her vital signs, maintaining uterine pressure and giving her warmth and emotional support.
Self-Assessment Questions (SAQs) for Study Session 11
Now that you have completed this study session, you can assess how well you have achieved its Learning Outcomes by answering the following questions. Write your answers in your Study Diary and discuss them with your Tutor at the next Study Support Meeting. You can check your answers with the Notes on the Self-Assessment Questions at the end of this Module.
SAQ 11.1 (tests Learning Outcome 11.1)
You are drafting the information that you want to send with the referral notice for a mother with PPH and you write it out as below. A young trainee colleague asks you to explain what you have written. How would you explain your referral note, including all the terms in bold, so that your colleague can understand?
‘I am referring Mebrihit. She is a high parity mother with excessive bleeding and is considered to be experiencing primary postpartum haemorrhage. I was careful to avoid trauma when assisting her delivery. Palpation indicates atonic postpartum haemorrhage which I suspect is due to failure of the myometrium.’
Answer
Here is how you could have explained to your trainee colleague what you had written in your referral note:
‘I am referring Mebrihit. She has had more than 5 pregnancies (high parity) and developed bleeding in excess of 500 ml of blood (excessive bleeding) within 24 hours of delivery (primary postpartum haemorrhage). I was very careful to avoid any injury (trauma) during the delivery. Feeling her abdomen (palpation) indicates that her uterus is soft and has not contracted properly after delivery (atonic postpartum haemorrhage). I suspect this is because the muscular wall of her uterus (myometrium) is failing to contract and close the blood vessels where the placenta pulled away from the uterus’.
SAQ 11.2 (tests Learning Outcomes 11.2 and 11.3)
You are assessing a pregnant woman in your care for potential risk of PPH.
- a.What questions would you ask her and what would you remember to check as part of your antenatal care visit?
- b.What checks and interventions would you make during her labour and delivery?
Answer
Here are some of the questions to ask and things to do. We expect you may have thought of even more.
- a.Antenatal care - questions to ask and things to check:
- Is she a first-time mother (primiparous) or has she had one or more deliveries already (multiparous), i.e. putting her more at risk of atonic PPH?
- If multiparous, was her earlier baby very large (over 4 kg) or did she have twins? (either of which may have overstretched her uterus).
- Does she remember if she had an excessive amount of amniotic fluid in a previous pregnancy (polyhydramnios)? More than 3 litres can also overstretch the uterus.
- Have you screened for anaemia (which you should continue in your postnatal checks)? If she has anaemia have you advised her about good nutrition?
- Is the community transport plan ready in case of emergency referral?
- b.During and after delivery – interventions to make and things to check:
- Make sure she regularly empties her bladder to avoid interfering with normal uterine contractions, including immediately after birth.
- Use the partograph to monitor labour progress so that you quickly notice any signs that might potentially lead to PPH (e.g. obstruction leading to possible uterine rupture).
- Be careful not to encourage pushing before the cervix is fully dilated and help to ensure controlled delivery of the baby’s head and shoulders in order to prevent tears.
- Encourage and help the mother to breastfeed immediately (so she starts to make her own oxytocin, which will stimulate the uterus to contract).
- Check that the placenta has fully separated and is intact, then rub the uterus every 15 minutes for the first 2 hours to help keep the uterus well contracted.
SAQ 11.3 (tests Learning Outcome 11.4)
Gelila delivered a baby 40 minutes ago. You gave her 600 µg of misoprostol orally immediately after the birth, but the placenta has not come out yet. She has emptied her bladder. After 10 minutes the placenta comes out and you check that it is intact, but Gelila starts bleeding heavily. What do you do?
Answer
Here is what you should do:
- Immediately shout for Gelila’s family and neighbours to get transport ready in case the bleeding becomes excessive and she needs to go to the nearest health facility.
- Check her rate of bleeding and unless it has quickly reduced, assume this is a case of atonic postpartum haemorrhage.
- If she had 600 μg misoprostol after the birth, give her a second dose of 400 μg misoprostol rectally or under her tongue to help her uterus to contract. If she had oxytocin before, give her another 10 IU by intramuscular injection.
- Lie Gelila on her back with her feet higher than the head, cover her with blankets and make sure she is warm.
- If you are trained to do so, begin pre-referral infusion of IV fluids.
- Try rubbing the uterus to encourage it to contract. If this fails then try two-handed compression on the uterus. If the bleeding stops and the uterus starts to feel firm, slowly release the pressure. If bleeding doesn’t stop, continue the referral process and get her to the health facility as quickly as possible.
- Accompany Gelila to the facility, checking her vital signs, and continuing to administer intravenous fluids. Make sure her baby comes too and that there are appropriate people to look after it and to act as possible blood donors.
- Write down everything that you have done on the referral note, together with Gelila’s history and identification details.