Use 'Print preview' to check the number of pages and printer settings.
Print functionality varies between browsers.
Printable page generated Monday, 25 May 2026, 7:51 PM
Postnatal Care Module: 2. The Normal Puerperium
Study Session 2 The Normal Puerperium
Introduction
In this study session you will learn about the normal postnatal changes that occur to women during the six weeks after childbirth. The postnatal period is also known by doctors, nurses and midwives as the puerperium. It includes the normal processes of physical and psychological adjustments during this period. Do you remember the physiological changes in pregnancy from the Antenatal Care Module, Study Session 3? Here we focus in detail on the normal adjustments during the puerperium, in particular the changes that occur in the reproductive system and in other body systems.
Puerperium is pronounced ‘poo-ayre-peer-ee-um’.
Some women in your postnatal care may not understand all of the normal changes which they experience after childbirth. They may become alarmed about changes that are perfectly normal, or ignore symptoms that are really danger signs. Some women find mothering a new baby very easy and natural; for others the mothering role may be difficult. As a Health Extension Practitioner working in the community, you have a unique opportunity to assist mothers and their families to cope with the adjustments during the postnatal period.
Learning Outcomes for Study Session 2
After studying this session, you should be able to:
2.1 Define and use correctly all of the key words printed in bold. (SAQ 2.1)
2.2 Describe the expected physiological responses of new mothers during the normal puerperium. (SAQ 2.2)
2.3 Explain what advice you will give new mothers for self-care during the puerperium at home. (SAQ 2.2)
2.1 Changes in reproductive organs during the puerperium
The important physiological events that occur during the puerperium include, among others, the return of the reproductive organs and the levels of the female hormones to approximately their pre-pregnant state. We will briefly describe these changes in turn, always focusing on what can be expected in a normal postnatal woman.
2.1.1 Uterus
The full term uterus has grown at least ten times bigger than it was before pregnancy. On its own it weighs approximately 1kg (not including the baby, placenta, amniotic fluid, etc), whereas its pre-pregnant weight was only 50-100 gm. Immediately after the baby is born, the uterus can be palpated at or near the woman’s umbilicus (belly button), as it contracts to expel the placenta and fetal membranes. It normally shrinks to its non-pregnant size during the first six weeks after delivery, but most of the reduction in size and weight occurs in the first two weeks. At around this time, the uterus should have shrunk enough to be located in the woman’s pelvis, below her umbilicus.
The inner lining of the uterus (the endometrium) rapidly heals after the birth, so that by the seventh day, it is restored throughout the uterus, except at the placental site. The inside of the uterus, where the placenta was attached, undergoes a series of changes which reduce the number of blood capilliaries entering that site. The capilliaries that remain ‘leak’ blood plasma for a time, which results in a normal vaginal discharge called lochia. This discharge often continues for several weeks after the birth. In the first week, the lochia is bloody and brownish red, but it gradually changes over time to a more watery consistency. Over a period of two to three weeks, the discharge continues to decrease in amount and the colour changes to pale yellow (straw coloured). The period of time the lochia continues varies, with an average duration of around five weeks, with a waxing and waning amount of flow and colour. Each woman has her own pattern, with the various phases of the lochia lasting for different lengths of time.
2.1.2 Cervix
Immediately after the delivery, the muscular walls of the cervix are relaxed, thin and stretched. The cervix may also appear swollen and bruised from the delivery, and it may have small breaks where the tissue was torn as the baby passed through. But within the first day the cervix has usually narrowed and regained its normal muscular consistency. On vaginal examination with a gloved hand, you should find the cervical opening about two fingers in diameter by 24 hours after the delivery, and by the end of the first postnatal week the opening narrows to one finger width.
2.1.3 Vagina and vulva
The vagina, which was stretched widely to allow the passage of the baby, gradually shrinks to its non-pregnant size and state over a period of about three weeks after the birth. By this date, the increased blood flow and swelling of the vagina and vulva, which was visible immediately after delivery, should have disappeared. Sexual intercourse may resume when the lochia ceases, the vagina and vulva are healed, and the woman is physically comfortable and emotionally ready. Physical readiness usually takes about three to five weeks, but the woman may not feel ready for sexual intercourse for a longer period and she should not be forced to accept it. Your role is to speak gently to her partner to ensure he understands and respects her feelings. In most communities there is a norm for when sexual intercourse starts, which is often after the puerperium ends, at around six weeks from the birth.
Remember that birth control is important to protect against another pregnancy following too soon after the previous birth. The first ovulation is very unpredictable and the woman may get pregnant again even before the return of her first menstrual period.
Birth spacing was discussed in Study Session 14 of the Antenatal Care Module.
What is the benefit of using postnatal family planning to space out the births of more children?
An interval of at least two years between births, and preferably a longer gap, reduces the risk of complications occurring to the mother during the next pregnancy. It also increases the health of the new fetus and the previous infant who may still need it’s mother’s constant care and attention (Figure 2.1).

2.1.4 Perineum
The perineum is the part of the body between the vaginal opening and the anal opening. It has been stretched and traumatised, and sometimes torn, during the process of birth. Or it may have been cut intentionally with sterilised scissors by a skilled birth attendant to widen the opening and help the baby out. Most of the muscle tone (strength) of the perineum is regained by six weeks after the birth, with more improvement over the following few months. You can help the mother to regain the muscle tone by encouraging her to contract and relax the muscles of the perineum ten times as soon as it is comfortable to do so, and to repeat this exercise several times every day. Strengthening the perineum is important because it forms the ‘pelvic floor’ which supports her uterus, vagina and bladder.
2.1.5 Abdominal wall
The abdominal wall remains soft and relatively poorly toned for many weeks after the birth, but it gradually becomes stronger over time. The extent of return to the muscular tone of the pre-pregnant abdomen depends greatly on the amount of exercise the woman takes as she returns to full fitness. For rural women, who work in the fields as well as in and around the home, the problem can be putting too much strain on their abdominal muscles (for example to lift heavy weights) too soon after the birth.
2.1.6 Ovaries
The resumption of normal function by the ovaries is highly variable and is greatly influenced by breastfeeding the infant. The woman who exclusively breastfeeds her baby has a longer period of amenorrhoea (absence of monthly bleeding) and delayed first ovulation after the birth, compared with the mother who chooses to bottle-feed. A woman who does not breastfeed may ovulate as early as four weeks after delivery, and most have a menstrual period by twelve weeks; the average time to the first menstruation for a woman who is not breastfeeding is seven to nine weeks after the birth.
Amenorrhoea is pronounced ‘aye-men-or-ee-ah’.
In the breastfeeding woman, the resumption of menstruation is highly variable and depends on a number of factors, including how much and how often the baby is fed, and whether the baby's feed is supplemented with formula milk. Ovulation is suppressed in the breastfeeding woman by a hormone released from the pituitary gland in the woman’s brain whenever the baby suckles. Half to three-quarters of women who breastfeed their babies exclusively, including during the night, will begin their first menstrual period within 36 weeks after the birth.
What kinds of points might you make to a young mother who has given birth recently and is breastfeeding, who asks you when she can resume sexual intercourse?
You could say that once her vaginal discharge (lochia) has more or less ceased and become pale yellow (after five to seven weeks) she can resume sexual intercourse if she feels physically and emotionally ready. You could also explain that breastfeeding makes it hard to predict when she will start ovulating again. And you could encourage her to think of family planning by explaining the risks of another pregnancy so soon after the birth, and the benefits of spacing babies by two years or more.
2.1.7 Breasts and initiation of lactation
Another important event that happens soon after the birth is the initiation of lactation, that is the production of colostrum and then milk by the breasts, and the release of these nutritious fluids when the baby suckles the mother’s nipple. The breasts begin to develop the capacity to produce milk as pregnancy progresses, in response to hormones circulating in the mother’s blood. For the first few days after the birth, the breasts secrete colostrum (a creamy yellow substance). Colostrum is rich in nutrients for the baby and also has maternal antibodies which protect the newborn from infection. Thus, it is very important that all babies are fed colostrum. In some parts of Ethiopia it is considered unhealthy to feed colostrum to newborns, but even if the mother is reluctant try to persuade her that it should not be thrown away.
Antibodies are special proteins that help to identify and destroy infectious agents.
Three days after delivery, in response to increased hormones from the pituitary gland in the brain, which stimulate milk production, the breasts become firm and milk supply begins. They rapidly become distended, hard and warm because of increased blood flow; this state of the breasts is called engorgement (Figure 2.2). It lasts about 24-48 hours and will resolve spontaneously. Thereafter, the breasts are not so hard and do not feel excessively warm, but they become firm and somewhat tender as they fill with milk between feeds, and they soften and reduce in size when emptied as the baby suckles milk. Ongoing milk production is stimulated by the suckling of the baby. The more the baby feeds, the more milk the breasts will produce.
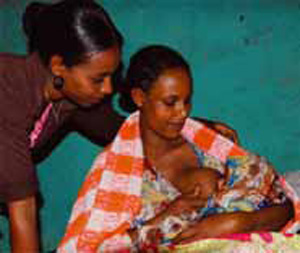
You should advise new mothers that early breastfeeding (within one hour of the birth) and exclusive breastfeeding (no other foods or fluids to be given to the baby) for the first six months is the best nutritional start in life. Allow the baby to be put to the breast whenever it wants to feed from the first day onwards. Breastfeeding is neither easy nor automatic, and it takes a lot of time in every day and during the night. It requires much effort on the part of the mother to breastfeed her baby exclusively for six months. Producing plenty of rich breast milk requires a lot of extra energy. The mother will need more nutrients and fluids, so advise her to drink plenty of clean fluids and to try to eat at least one additional meal every day while she is breastfeeding. More detailed information on breastfeeding is given in Study Session 7.
Suppression of lactation in non-breastfeeding women
There are circumstances when the mother cannot or will not breastfeed, for example if the baby is born dead or dies in the first few weeks, or when the mother strongly prefers to feed her baby with formula milk from a bottle. To reduce the discomfort of prolonged breast engorgement, it is recommended to wrap a tight compression bandage around the woman’s chest, covering the breasts, for the first two to three days after the birth. Care should be taken not to stimulate the breasts in any way that would encourage milk production. Ice packs can be applied to the breasts and pain-control tablets containing aspirin or paracetamol may be given to relieve the breast tenderness.
2.1.8 Excretion of excess body fluids
During the pregnancy, the woman’s body contains more body fluids than in the non-pregnant state. Some of this additional water is held in her tissues, some in her increased volume of blood, and some in the uterus. This excess water is rapidly eliminated after the birth. The amniotic fluid drains away through the vagina. From the second day after the delivery, the urine volume will increase up to three litres per day for a few days, but within one week it returns to the normal pattern of urination. The bladder increases its capacity during the period in which excess body fluids are being eliminated, filling with between 1,000 to 1,500 ml of urine without discomfort.If urine is retained for long periods in the bladder, because the urethra is obstructed by swollen or bruised tissues after the birth, it increases the risk of urinary tract infections developing.
You learned about urinary tract infections (UTIs) in Study Session 18 of the Antenatal Care Module.
2.2 Important information for the first-time mother
2.2.1 Looking after the baby
New mothers (and often also new fathers) should be taught routine care of the baby, including bathing and keeping its body and clothes clean of its faeces and urine. Teach the parents what can be expected from the baby in terms of sleep, urination, bowel movements, feeding and crying. The baby should be kept warm, but not wrapped too tightly. It should be checked carefully and often to ensure that it is not too hot or too cold, and that it is feeding well and passing normal stools and urine frequently. More details of newborn baby care are given later in this Module in Study Sessions 6 to 8.
2.2.2 Rest and recovery for the mother
Pregnancy, labour, delivery and care of the newborn are strenuous and stressful; the mother needs sufficient rest to recover. She also needs information about when it is safe for her to resume her normal activity. Tell her that she may resume some household activities within two or three days of the birth, as long as she experiences no pain or discomfort. The key to resuming normal activity is not to do too much one day so she feels completely exhausted the next day.
2.2.3 Birth control options
The mother and her partner should also be counselled about birth control options. She may not be ready to decide about a method, but she needs to know the options. Her decision will be based on a number of factors, including her motivation in using a particular method, how many children she has, and whether she is breastfeeding.
Many options are available, which we will mention only briefly; the details of the different methods are addressed in the Module on Family Planning.
- Natural methods involve looking at the nature of the cervical mucus (quality and quantity), which can work fairly well to indicate when the woman is ovulating, but are not a secure way to prevent pregnancy.
- Breastfeeding exclusively and on demand by the baby can give reasonably good protection from pregnancy for up to six months, if the woman’s menstrual periods have not returned.

Barrier methods of contraception create a barrier between the male sperm and the vagina or cervix. The most commonly used barrier method is male condoms, which are widely available.
- Hormonal methods of contraception include contraceptive pills, injectable contraception, and implants (a tiny rod containing slow-releasing hormones which is put under the skin).
- Intrauterine devices (IUDs) are devices put inside the uterus to prevent implantation of an embryo; they can be inserted at the end of the puerperium.
- Permanent methods of birth control include cutting and tying the fallopian tubes (which extend from the uterus on either side towards the ovary) in females, and cutting the tube transporting male sperm from the testacles to the penis (vasectomy).
Without looking back at the sections above, write a very brief note for yourself of the key points that you will make to the parents of a newborn, advising them about caring for their baby.
Now check your list against the information in Sections 2.2.1, 2.2.2 and 2.2.3.
2.3 In conclusion
In most women, the puerperium passes without problems and is a time of joy for the mother and other members of the family to be with the new baby. But it is important that mothers and their partners are informed of what normally happens during this period, and that you make sure there are no danger signs which can compromise the health of the mother or the newborn. We are going to turn to the abnormal puerperium in Study Session 3 of this Module. Remember that if you detect abnormalities during postnatal follow-up visits, refer the woman and baby quickly for further assessment and treatment to the next higher health facility.
Summary of Study Session 2
In Study Session 2, you have learned that:
- The period of six weeks after childbirth is called the puerperium; this is when the physiological changes to the mother’s body that occurred in pregnancy revert back to normal. The uterus, cervix, vagina and vulva reduce in size and the excess fluids retained during pregnancy are quickly eliminated in the mother’s urine.
- Postnatal mothers have a normal reddish, watery vaginal discharge after childbirth called lochia, which gradually reduces during the puerperium and changes colour to pale yellow.
- The changes to the breasts that prepare them for breastfeeding occur throughout pregnancy; production of colostrum begins soon after the birth, followed at about three days by breast engorgement and production of true milk.
- The colostrum released by the breasts during the first two to three days after delivery is rich in nutrients and maternal antibodies; it should always be fed to the newborn.
- Breastfeeding should begin within the first hour after childbirth and continued exclusively, and on demand by the baby, for the first six months.
- Mothers (and often fathers) need support to adjust to the demands of caring for a new baby, including support for beginning breastfeeding and keeping the baby warm and clean. Mothers need time for rest and recovery before resuming normal activities.
- The various options for postnatal family planning should be discussed with both parents.
Self-Assessment Questions (SAQs) for Study Session 2
Now that you have completed this study session, you can assess how well you have achieved its Learning Outcomes by answering the questions below. Write your answers in your Study Diary and discuss them with your Tutor at the next Study Support Meeting. You can check your answers with the Notes on the Self-Assessment Questions at the end of this Module.
SAQ 2.1 (tests Learning Outcome 2.1)
Which of the following statements is false? In each case (i) explain what is incorrect, and (ii) define the term that is in bold.
A A woman during the puerperium will not normally produce lochia after the birth.
B Initiation of lactation and production of colostrum follows soon after delivery of the baby.
C Breast engorgement is a sign that breastfeeding can be initiated.
D The endometrium can take seven weeks to heal after the birth.
Answer
A False: all postnatal women will have watery, coloured vaginal discharge (lochia) for around five weeks after the birth. This is about the same time as the puerperium – which is the postnatal period of physiological changes occurring during the five to six weeks after childbirth.
B True: initiation of lactation – i.e. the production of colostrum (a creamy yellow nutrient rich ‘first milk’ which also contains the mother’s antibodies), follows automatically soon after delivery of the baby and then true milk begins after about three days.
C Not quite true: breast engorgement is a response to the initiation of the milk supply and usually happens about three days after the delivery. Mothers are encouraged to initiate breastfeeding within one hour of the birth.
D False: the endometrium (which is the inner lining of the uterus) heals rapidly and by the seventh day is normally restored except at the placental site.
SAQ 2.2 (tests Learning Outcomes 2.2 and 2.3)
You are seeing a woman who gave birth to her second child 14 days ago. She looks reasonably well, but she seems a bit worried. Briefly describe all the checks you would do to make sure that everything is OK and she is recovering normally.
Answer
There are many checks that you could do – here are some of the key ones:
- By palpating below the women’s umbilicus, you can see if the uterus has shrunk at the normal rate.
- Ask her whether she has a lot of vaginal discharge and what colour it is.
- By doing a vaginal examination, check that the cervical opening has shrunk to less than one finger width.
- Examine whether the swelling of the vagina and vulva is going down or has nearly gone.
- If the perineum was cut or torn during the birth, make sure it is healing properly, and if so encourage the mother to start exercising her perineum muscles.
- Check if she has difficulty breastfeeding, or (if she has decided not to breastfeed) that she is managing to reduce her milk production.
- Check that the baby is neither too hot nor too cold, is feeding well and passing stools regularly.
- Ask, tactfully, if the mother feels any pressure from her partner to resume sexual intercourse before she feels ready to do so.
- Try and assess whether she may be taking on too much work too soon.
- With the physical checks there are key signs which will tell you whether the puerperium is progressing normally, and if it is, you can reassure your worried mother. What she feels able to say to the more personal questions will be more difficult to assess. You will have to use all your sensitivity and tact in order to judge whether something else may be going wrong.