Use 'Print preview' to check the number of pages and printer settings.
Print functionality varies between browsers.
Printable page generated Sunday, 17 May 2026, 2:57 PM
Postnatal Care Module: 3. The Abnormal Puerperium
Study Session 3 The Abnormal Puerperium
Introduction
As you learned in Study Session 2, the course of the puerperium goes smoothly in most women. The puerperium is the period of about six weeks after the birth, in which physiological adjustment to the non-pregnant state occurs. However, sometimes women will develop health problems which should come to your attention. You may handle some of these problems yourself, but you will need to refer others for further assessment and treatment at a hospital or health centre. Infections are among the most prominent puerperal complications and are a major cause of maternal mortality in Ethiopia. Fever is the main symptom and antibiotics are the main treatment. Prevention of infection by ensuring cleanliness and hygiene at delivery is obviously the best course of action.
The term ‘postpartum’ means ‘after the birth and related to it’.
The other common complications include late postpartum haemorrhage (PPH), urinary tract infections, hypertension and mental health problems. In this study session, you will learn about the common abnormalities that can occur in the course of the puerperium, and one uncommon but life-threatening complication – deep vein thrombosis (a blood clot inside the veins that blocks the blood flow).
Learning Outcomes for Study Session 3
After studying this session, you should be able to:
3.1 Define and use correctly all of the key words printed in bold. (SAQ 3.1)
3.2 Describe the causes of late postpartum haemorrhage. (SAQ 3.1)
3.3 Discuss the common types of puerperal infections and their risk factors. (SAQ 3.2)
3.4 Identify the signs and the risk factors for deep vein thrombosis. (SAQ 3.3)
3.5 Define the clinical features of the common puerperal abnormalities, including postpartum mental health problems. (SAQs 3.1 and 3.4)
3.1 Postpartum haemorrhage
Study Sessions 3 and 11 of the Labour and Delivery Care Module explained that a life-threatening postpartum haemorrhage (PPH) involves losing at least 500 ml of blood from the uterus or vagina. The most critical period to develop a PPH is during the third and fourth stages of labour.
What are the third and fourth stages of labour?
The third stage is delivery of the placenta and fetal membranes; the fourth stage is the next four hours.
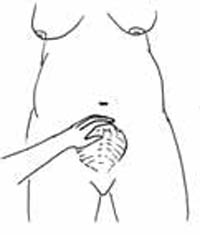
About 90% of deaths due to PPH take place within four hours of delivery. During the first four to six hours, you should make sure that the uterus remains well contracted (Figure 3.1) and that there is no heavy loss of blood. However, a woman can develop a haemorrhage at any time during the puerperium, generally in the first week after delivery, but even up to six weeks postpartum. This type of bleeding is referred to as secondary (late) postpartum haemorrhage.
The presence of anaemia or a heart condition can be life-threatening for the mother even if the loss of blood is less than 500 ml. A woman who is malnourished is also usually less able to cope with blood loss than a woman who is well nourished.
3.1.1 Causes of late postpartum haemorrhage
The bleeding is usually as a result of poor contraction of the uterus after the birth, which fails to close off the torn blood capillaries where the placenta has pulled away. If the uterus is unable to reduce in size as it should do normally, it may be because of infection, or retention of a piece of the placenta, which later tears loose from the wall of the uterus and causes a haemorrhage. Box 3.1 summarises the common causes of late PPH.
![]() If there is obvious excessive vaginal bleeding, or you suspect heavy bleeding may be happening internally, refer the mother urgently to the nearest hospital or to a health centre with a blood transfusion service.
If there is obvious excessive vaginal bleeding, or you suspect heavy bleeding may be happening internally, refer the mother urgently to the nearest hospital or to a health centre with a blood transfusion service.
Box 3.1 Causes of late postpartum haemorrhage
- Endometrial wall infection: Endometritis is described in Section 3.2.1. When the site of placental implantation (the placental bed) is not yet healed, infection in the uterus can cause the blood capillaries in the placental bed to start bleeding again.
- Poorly contracted uterus: The uterus may not contract well because of infection, retained placental fragments, or an unknown reason. As a result, bleeding can start again.
- Retained placenta: Remnants of placental tissue or fetal membranes retained in the uterus are common causes of late PPH.
- Sloughing of the placental bed: There is a possibility that the healed placental bed peels away (sloughs) and opens the blood capillaries again.
- Molar pregnancy: Although it is uncommon for a woman to develop a molar pregnancy after delivery, its occurrence can have life-threatening complications; the rapidly growing mass of grape-like tissues in the uterus can cause profuse haemorrhaging.
3.1.2 Pre-referral management of PPH
You should remember that any amount of active (fresh or bright red) vaginal bleeding after 24 hours may be due to one of the causes listed in Box 3.1, or others not mentioned. Therefore, you should refer these women to a hospital regardless of the amount of bleeding. You should also remember that if the bleeding is severe, only a blood transfusion can save the life of the mother.
The more detailed management of PPH was taught in Study Session 11 of the Labour and Delivery Care Module and described in Study Session 22 of the Antenatal Care Module, as well as in your practical skills training.
What did these study sessions tell you to do before referring a women with PPH?
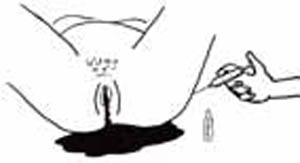 Figure 3.2 Inject 10 IU of oxytocin (or give 400 micrograms misoprostol) before referring a woman with PPH.
Figure 3.2 Inject 10 IU of oxytocin (or give 400 micrograms misoprostol) before referring a woman with PPH.Put up an intravenous (IV) line, and start the woman on intravenous fluid therapy with Ringer’s Lactate or Normal Saline, using a 1,000 ml (1 litre) bag and a flow rate set to run as fast as possible.
As a pre-referral treatment, you should also give her a second dose of misoprostol (400 micrograms orally or rectally), or oxytocin 10 IU (International Units) by intramuscular injection (Figure 3.2).
3.2 Puerperal sepsis and fever
Puerperal sepsis refers to any widespread bacterial infection of the reproductive tract in a woman following childbirth. Some women are more vulnerable to puerperal sepsis, for example those who are anaemic and/or malnourished. Fever (raised body temperature) in a mother during the postnatal period is a general danger sign. She suddenly feels chills with shivering, followed by feeling hot and sweating. Fever in the postpartum period may be due to puerperal sepsis, but it can also be caused by:
All these infections are described in the Communicable Diseases Module.
- Urinary tract infection
- Wound infection
- Mastitis or breast abscess
- Infections not related to the pregnancy or delivery, such as HIV, malaria, typhoid, tetanus, meningitis, pneumonia, etc.
In the majority of cases, postnatal maternal infection is preventable either by conducting a clean and safe delivery, by immunizing all pregnant women against tetanus, and by providing timely treatment of pre-existing infections. In malaria endemic areas, do not forget to give long lasting insecticide-treated bed nets (ITNs, Figure 3.3) during your home visit, if they were not given before, and advise mothers on how to regularly and continuously use them. Make sure the mother and newborn are sleeping under a net every night.

3.2.1 Endometritis
Endometritis is an infectious process involving the inner wall of the uterus (the endometrium). It is commonly caused by bacteria ascending from the vagina, or bacteria transferred to the reproductive tract from the rectum and anus. Commonly known and avoidable risk factors contributing to the risk of endometritis include:
PROM is the subject of Study Session 17 of the Antenatal Care Module.
- Long labour: This risk can be managed by timely referral of women in prolonged labour.
- Prolonged and premature rupture of fetal membranes (PROM): The risk of infection is greatest if PROM has occurred long before the baby is delivered. You can reduce the risk by early referral.
- Repeated vaginal examinations: You can avoid this risk by not doing unnecessary internal examinations.
- Poor standard of hygiene and cleanliness during delivery: For example, insertion of an unclean hand into the vagina, or use of non-sterile instruments, can transmit infection.
- Pre-existing infection: Colonisation of the vagina and uterus from untreated sexually transmitted infections (STIs) or urinary tract infections (UTIs).
- Retained placenta or fetal membranes: The dead cells in these tisues favour the multiplication of bacteria.
- Manual removal of the placenta: If the umbilical cord tears (breaks) when you apply controlled cord traction to help delivery of the placenta, it may be retained and the woman may start to bleed profusely. In these circumstances, you will be forced to remove the placenta manually by inserting your fingers into the endometrial cavity, locating the placenta and removing it in pieces or in totality. In addition to the risk to the mother from the haemorrhage, there is also a risk of endometrial infection.
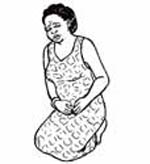 Figure 3.4 Pain in the abdomen may be a sign of endometritis.
Figure 3.4 Pain in the abdomen may be a sign of endometritis. - Anaemia: Whether it is due to blood loss during pregnancy, labour and delivery, or due to nutritional deficiency, anaemia is a well known risk factor for endometritis and other types of puerperal infection.
- Traumatic delivery: (e.g. assisted by forceps, or by Caesarean section)
- Postpartum haemorrhage.
STIs are described in Study Session 31 of the Communicable Diseases Module; UTIs are covered in Study Session 18 of the Antenatal Care Module.
Signs of endometritis
A woman with endometritis typically has a fever of 38°C or higher, a rapid pulse and pain (tenderness) when you palpate the abdomen (Figure 3.4). Some women may also develop a yellowish, curd-like vaginal discharge which has a bad odour, whereas others have a little odourless discharge. In short, to assess the mother for uterine infection, ask if she has:
- History of fever or if she feels hot. Measure her temperature and she has a fever if it is equal to or greater than 38°C.
- Lower abdominal pain.
- Foul-smelling, curd-like discharge from her vagina.
![]() If the mother has even one of the above findings, assume she has endometritis and refer her urgently to the nearest hospital or health centre.
If the mother has even one of the above findings, assume she has endometritis and refer her urgently to the nearest hospital or health centre.
If you suspect a woman in the puerperium may have endometritis when you do your early postnatal visits, it is important that you refer her quickly for further treatment. If she has low blood pressure (diastolic less than 60 mmHg), you may begin an IV infusion of Normal Saline. Keep her lying flat with her legs lifted up by putting pillows underneath her knees (shock position), before transporting her to a health facility.
Which of the risk factors for developing endometritis can you, personally, do most about?
Ensuring the highest standards of hygiene and cleanliness during delivery; and avoiding, where possible, repeated vaginal examinations of the mother.
3.2.2 Urinary tract infections
Another common cause of pain and fever in the puerperium is a urinary tract infection (UTI). A woman with a UTI complains of urine coming too frequently, a burning sensation when she passes urine, and the urge to urinate very often. When you gently press on her abdomen overlying the pelvis she will have pain. This woman needs referral for treatment with antibiotics.
UTI is common during pregnancy and the puerperium because of:
- urinary retention due to urinary tract obstruction in some women in late pregnancy;
- manipulation and trauma to the urethra during labour and delivery, which increases the risk of bacteria from the birth canal and rectum ascending into the bladder and from there to the kidneys.
3.2.3 Puerperal mastitis

Mastitis is painful inflammation of the breast due to bacterial infection (Figure 3.5). The bacteria most often causing mastitis, or a more serious breast abscess, are called Staphylococcus aureus. The main source of these bacteria is the suckling baby. Mastitis is more likely to develop during lactation than when the breast is not producing milk. Commonly, it results from milk remaining in the breast for long periods (incomplete emptying), because the baby is not suckling well, or from cracked nipples.
How might cracked nipples be a risk factor for mastitis?
Pain from the cracked nipples may make the mother reluctant to breast feed, so her breasts remain engorged with milk; also, bacteria from the baby’s mouth or from the mother’s skin can get into the breast through the cracked nipples.
Neglected, resistant, or recurrent infections of the breast can lead to the development of an abscess, a collection of pus within the breast. Pus is a yellowish-white, sticky fluid formed in infected tissue, consisting of bacteria, white blood cells, cellular debris and dying tissue. Women with mastitis often experience pain, fever, chills and muscle aches over the body. The breast will look red, hot and is very painful to touch. When the examination reveals a tender, hard mass with overlying redness, a breast abscess is likely.
If you make a diagnosis of mastitis or breast abscess, give pain relief with paracetamol, supporting the breast with brassieres or anything that can be wrapped around the chest, and refer the woman to the health centre and/or nearest hospital for antibiotic treatment.
![]() Refer women with mastitis or breast abscess.
Refer women with mastitis or breast abscess.
When you counsel a woman with a breast infection, NEVER advise her to stop feeding the baby from the infected breast. Emptying the breast by letting the baby suckle the milk will help to reduce the problem and the pain. Therefore, encourage breastfeeding unless pus is coming through the nipple. However, breastfeeding is not advised if the cause of breast infection is suspected to be tuberculosis (TB), which is characterised by long-standing evidence of infection with healing (scarring) and new infection in the same breast.
3.2.4 Wound infection
Wound infections in the puerperium usually affect torn tissues in the perineum, infection of an episiotomy (an incision made to widen the vaginal opening to let the baby pass through), or a surgical wound in the abdomen after a caesarean birth conducted at a health facility.
In general, wound infections become apparent on the third or fourth postpartum day and are diagnosed on the basis of erythema (reddening of the area of infection), and the tissue overlying the affected area thickens, gets warm and is painful to touch. It may drain yellowish pus from the wound site, and may occur with or without fever.
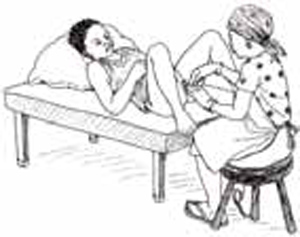
Treatment of perineal wound infections includes relieving pain with paracetamol, and bathing with warm water in which one teaspoon of salt has been dissolved for every litre of water. If there is pus coming from a wound on the perineum, further drainage of the pus can be achieved by compressing the area with a cloth soaked in warm salty water (Figure 3.6).
In the case of a woman who also has fever and chills, and you suspect there is pus which is not draining out of the wound, you should refer her to the next higher health facility so that she can be treated with antibiotics. If she has an abscess, it may need to be drained surgically. Most patients respond quickly to the antibiotics once the wound is drained. Antibiotics are generally continued until after the patient has no fever for 24-48 hours.
Abdominal wound infections are generally treated at a hospital, so refer such women to the next higher health facility.
3.3 Screening for postpartum hypertension
Diastolic blood pressure is measured when the heart relaxes between heartbeats.
The hallmark of pregnancy-induced hypertension is high blood pressure, usually a diastolic blood pressure more than 90 mmHg. You learned how to take the mother’s blood pressure in the Antenatal Care Module, Study Session 9, and about hypertensive disorders of pregnancy in Study Session 19. Here we are concerned about hypertension that begins or returns in the puerperium. In order to screen for this you should ask the mother about the following symptoms:
- Severe headache, with or without visual disturbances (blurring of vision), and sometimes with nausea and vomiting.
- Convulsions/fits in the most severe cases (eclampsia). Make sure that you know the local terminology for a convulsion. It can be explained as an abnormal and uncontrollable rhythmic movement of the arms and legs, with or without losing consciousness.
- Swelling (oedema) of hands and feet, or especially the face.
- Severe pain in the upper part of the abdomen.
You should do a dipstick urine test (as you learned in Study Session 9 of the Antenatal Care Module). When urine is tested with a dipstick for the presence of protein, a woman with hypertension is likely to test positive. The positive values on the dipstick are graded from +1 up to +3 and more. If any one of the above findings is present, suspect pregnancy-induced hypertension and refer the woman urgently to the nearest health facility. Remember that postpartum hypertension can develop in any woman, even one who had normal blood pressure and was symptom-free during pregnancy, labour and delivery.
3.4 Deep vein thrombosis (DVT)
Deep vein thrombosis (DVT) — a blood clot, almost always in one of the deep veins in the legs — is a rare complication during the puerperium. However, when it occurs it can be rapidly fatal if the clot breaks away from the vein in the leg and travels to the heart, lungs or brain, blocking vital blood vessels.
The chance of developing a DVT is more common during pregnancy than in the non-pregnant state, and the risk increases during the puerperium. Why deep veins in the legs develop clots (thrombosis) is not exactly known. However, the risk is much higher when the postnatal woman spends most of the time in bed and doesn’t walk about much for several days after the birth. In most parts of Ethiopia, the local custom is for postnatal women to remain in bed, with no activity except a short walk to use the latrine. So it is important for you to identify the clinical features of DVT, make a diagnosis and refer her to a hospital as early as possible. Box 3.2 shows the common clinical features of DVT.
Box 3.2 Clinical features of deep vein thrombosis (DVT)
- Pain in one leg only: usually sudden onset, persistent and aching type of pain.
- Tenderness: the area is painful when you touch it.
- Swelling: the affected leg is swollen with greater than 2 cm difference in circumference compared to the other (healthy) leg. The swelling may be in the calf or the thigh.
- Palpable cord: you may feel a cord-like structure deep in the swollen leg.
- Change in limb colour: the affected leg appears a little bit red.
- Calf pain: she will feel pain when you try to do extreme extension at the ankle joint.
3.5 Psychiatric disorders in the postnatal period
Psychiatric disorders are relatively common after childbirth and may include postpartum ‘blues’, postpartum depression (PPD), and postpartum psychosis.
3.5.1 Postpartum ‘blues’ and postpartum depression

Hormone changes are thought to be the cause of postpartum blues, a mild, transient, self-limiting disorder (it resolves on its own), which commonly arises during the first few days after delivery, and lasts up to two weeks. It is characterised by bouts of sadness, crying, anxiety, irritation, restlessness, mood swings, headache, confusion, forgetfulness, and insomnia. It rarely has much effect on the woman’s ability to function, or care for her baby. Providing loving support, care and education has been shown to have a positive effect on recovery (Figure 3.7).
![]() Refer women who are seriously depressed after childbirth.
Refer women who are seriously depressed after childbirth.
But if a women develops a serious postpartum depression (persistent sadness, low mood, difficulty in finding motivation to do anything), it will greatly affect her ability to complete the normal activities associated with daily living. Cases of depression need attention from trained mental health professionals for supportive care and reassurance, so refer the woman as soon as you can. The role of the patient’s family is also very important in the course of treatment. Women with high levels of depression are less likely to initiate breastfeeding soon after the birth, and their babies are more likely to have episodes of illness such as diarrhoea.
Can you suggest why the baby might be affected in this way?
If breastfeeding is not commenced successfully the woman may bottle-feed the baby with formula milk, which carries a greater risk of infection to the baby from unclean bottles. A depressed mother may also not take notice of health education messages about preventing infection in her newborn.
If two or more of the following symptoms occur during the first two weeks of the puerperium, refer the mother:
- Inappropriate guilt or negative feelings towards herself
- Cries easily
- Decreased interest or pleasure
- Feels tired and agitated all the time
- Disturbed sleep, sleeping too much or sleeping too little
- Diminished ability to think or concentrate
- Marked loss of appetite.
There may also be episodes of postpartum psychosis, marked by delusions or hallucinations – seeing or believing things that are not real. We return to this more serious problem in Study Session 5. You will learn a lot more about mental health issues, including postnatal depression and psychosis, in the Module on Non-Communicable Diseases, Emergency Care and Mental Health.
Summary of Study Session 3
In Study Session 3, you have learned that:
- Although the most critical period to develop postpartum haemorrhage is in the third and fourth stages of labour, you should continue being vigilant during the puerperium and counsel the mother to report any active vaginal bleeding.
- The commonest causes of late PPH are endometritis, poor uterine contraction, retained placenta and sloughing of the placental bed.
- Any amount of active vaginal bleeding after 24 hours of delivery should be taken as a serious complication and the woman should be referred.
- The commonest types of puerperal infection are endometritis, mastitis, urinary tract infection and wound infection, all of which are usually accompanied by fever.
- Risk factors for postnatal endometritis are prolonged labour, prolonged PROM, repeated vaginal examination, pre-existing lower reproductive tract infection, retained placenta, and traumatic delivery including caesarean section or forceps.
- In a woman who develops puerperal mastitis, breastfeeding is encouraged.
- Postpartum hypertension characterised by high blood pressure, oedema, visual disturbances and (in eclampsia) convulsions, can develop in a woman who had normal blood pressure and was symptom-free during pregnancy, labour and delivery.
- Deep vein thrombosis is characterised by a painful and swollen leg, and more commonly occurs in women who remain in bed for several days after the birth.
- Some women may develop mental health problems, the commonest of which is short-term, mild postpartum blues. Some women may develop serious depression which needs care and treatment at a higher level facility.
Self-Assessment Questions (SAQs) for Study Session 3
Now that you have completed this study session, you can assess how well you have achieved its Learning Outcomes by answering the questions below. Write your answers in your Study Diary and discuss them with your Tutor at the next Study Support Meeting. You can check your answers with the Notes on the Self-Assessment Questions at the end of this Module.
SAQ 3.1 (tests Learning Outcomes 3.1, 3.2 and 3.5)
You are talking to one of your co-health workers about the complications that can occur in the course of the puerperium. She has only just started her health worker training and is curious about the following terms and what their key symptoms are. What might you say to her about each of the following?
- a.Late postpartum haemorrhage.
- b.Puerperal sepsis and fever.
- c.Mastitis.
- d.Postpartum hypertension.
- e.Postpartum depression.
Answer
- a.Late postpartum haemorrhage (PPH) is heavy vaginal bleeding during the first week and up to six weeks after delivery. PPH can be life threatening and must be referred immediately. Most common causes include infection (endometritis) of the inner wall of the uterus, failure of the uterus to contract properly, sloughing (peeling away) of the placental bed, or bits of the placenta remaining in the uterus. A less common cause is molar pregnancy.
- b.Puerperal sepsis is a widespread bacterial infection of the reproductive tract following childbirth. It can mostly be prevented by good hygiene during delivery. Fever indicates the possibility of sepsis, but it could also be due to urinary tract infection or infected wounds, HIV, malaria, typhoid, tetanus, meningitis, pneumonia, etc.
- c.A hot red painful breast indicates mastitis, an inflammation of the breast due to bacterial infection. Women lactating are at a higher risk of puerperal mastitis if the baby does not suckle well and the breast is not emptied of milk. An abscess is another risk from breast infection, when pus collects in the infected tissue.
- d.Postpartum hypertension is excessively high blood pressure in the postnatal period. Key symptoms are severe headache, convulsions (eclampsia), swelling, severe abdominal pain, and protein in the urine. It is life-threatening and must be referred immediately.
- e.Postpartum depression is more serious than postpartum blues. The ‘blues’ are a mild sense of sadness, anxiety or confusion that many women experience after giving birth and which normally passes. Women with postpartum depression (persistent sadness and low mood with little motivation) should be referred.
SAQ 3.2 (tests Learning Outcome 3.3)
Complete the empty boxes in Table 3.1, referring to complications in the puerperium.
| Symptom | Sign | Possible diagnosis | Action |
|---|---|---|---|
| Vaginal bleeding on postpartum day seven | Uterus at the level mid-way between umbilicus and pelvis | ||
| Urinary traction infection (UTI) | Encourage fluid intake by mouth and refer | ||
| Pain over the breast and fever | Breast painful to touch, hot and red | ||
| Pain in the perineum | Torn perineum with yellowish discharge, painful to touch |
Answer
The completed Table 3.1 will look as follows:
| Symptom | Sign | Possible diagnosis | Action |
|---|---|---|---|
| Vaginal bleeding on postpartum day seven | Uterus at the level mid-way between umbilicus and pelvis | Endometritis | Start an IV infusion and refer |
| Urinary frequency and urgency | Pain in the pelvis overlying the bladder | Urinary tract infection (UTI) | Encourage fluid intake by mouth and refer |
| Pain over the breast and fever | Breast painful to touch, hot and red | Mastitis, possibly breast abscess | Give a pain killer and refer |
| Pain in the perineum | Torn perineum with yellowish discharge, painful to touch | Infected wound | Salt bath, warm compresses, paracetamol for pain relief and possibly refer for antibiotics |
SAQ 3.3 (tests Learning Outcome 3.4)
You are visiting a mother called Lakesh who had her baby seven days ago. The last time you saw her she was lying in bed. This time she gets up to greet you and you notice that she is limping. You ask her if she has hurt herself. She mentions a sudden ache in one of her legs. What would you suspect and what would you do about it?
Answer
You should immediately remember that the risk of deep vein thrombosis (DVT) is higher if the postnatal woman spends most of her time in bed, as Lakesh has been doing. You would quickly check if any or all of the clinical features of DVT as set out in Box 3.2 also applied. If the signs lead you to suspect that Lakesh has a DVT, you would refer her to a higher-level health facility as quickly as possible.
SAQ 3.4 (tests Learning Outcome 3.5)
Another mother called Almaz is in the first postpartum week; she feels persistently guilty and negative towards herself, cries easily and feels tired and agitated. What might she be suffering from? What other symptoms would you ask her about, to confirm your diagnosis?
Answer
The likely diagnosis for Almaz’s condition is postpartum depression. To check your diagnosis, you would ask her about the following symptoms:
- Decreased interest or pleasure
- Disturbed sleep, sleeping too much or sleeping too little
- Diminished ability to think or concentrate
- Marked loss of appetite.