Use 'Print preview' to check the number of pages and printer settings.
Print functionality varies between browsers.
Printable page generated Tuesday, 9 June 2026, 11:03 PM
Antenatal Care Module: 8. Diagnosing Pregnancy and Learning a Pregnant Woman’s History
Study Session 8 Diagnosing Pregnancy and Learning a Pregnant Woman’s History
Introduction
This study session begins by providing you with the knowledge to diagnose when a woman is pregnant. You will learn to distinguish between the possible, the probable, and the positive (or sure) signs and symptoms of pregnancy. A symptom is an indication of a condition (such as pregnancy), or a disease or disorder, that is noticed by the affected person and which they can tell you about either spontaneously, or if you ask the right questions. By contrast, a sign is an indication that only a trained health professional would notice, or be able to detect by conducting a test.
To give good care to a pregnant woman, you also need to find out about her general health and any past pregnancies and births she may have had, and what this pregnancy has been like so far. These details are called a health history. The process of gathering all the information and recording it using clear, accessible questions is called history taking. In this study session you will learn how to ask focused questions about a pregnant woman’s health history. This knowledge will help you give correct and individualised advice to make this pregnancy and birth as safe as possible. You will also recognise the importance of maintaining the woman’s trust by keeping what she says to you confidential.
Learning Outcomes for Study Session 8
When you have studied this session, you should be able to:
8.1 Define and use correctly all of the key words printed in bold. (SAQs 8.1 and 8.4)
8.2 Say why it is important to gain the trust and confidence of a woman who comes to you for antenatal care, and give an example of how you can keep or lose her trust. (SAQ 8.1)
8.3 Distinguish between the possible, probable and positive signs of pregnancy, and decide whether a woman is possibly or probably pregnant, based on fictional case studies. (SAQ 8.2)
8.4 Ask clear, accessible questions to help you get information about possible pregnancy symptoms, or common risk factors that might affect the health of a pregnant woman or her baby. (SAQs 8.1 and 8.5)
8.5 Identify the serious risk factors that would make it advisable for a woman to give birth in a health facility rather than at home. (SAQs 8.3 and 8.4)
8.1 Gaining a woman’s trust in antenatal care
In order to make a good diagnosis of whether a woman is pregnant, or learn about her health history as part of her antenatal care, you must first gain her trust, and make her feel comfortable to talk to you about her personal details. Begin by introducing yourself and asking her respectfully to talk about herself and her health history. At first, she may not be willing to do this. If she feels shy about her body or about sex, it may be difficult for her to tell you things that you need to know about her health. Try to help her relax and trust you by listening carefully, answering her questions in language that she understands, keeping what she tells you private, and treating her with respect.
What could happen if you tell others what she has said to you about her personal history?
She could lose trust in you as a health professional. She may be less willing to talk honestly to you the next time you see her.
How could her loss of trust in you lead to a greater risk for her health or that of her baby?
She may not tell you important information about her pregnancy that could help you to identify possible risk factors before they become serious. She might even miss antenatal appointments because she doesn’t trust you.
You will be writing down what you learn about each pregnant woman in her antenatal record card (Figure 8.1).
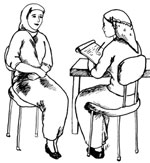
This information may be needed later in the pregnancy, during labour and delivery, or after the baby is born (the postnatal period). Reassure her that you won’t let anyone except other health professionals see the notes you have made about her.
First we will suggest the kinds of questions you could ask to help identify whether a woman is pregnant. Then we will explain what other information you will need to ask her about. This is so you can identify any risk factors she may have, and look after her effectively during the pregnancy.
8.2 Finding out if a woman is pregnant
The indications of pregnancy are generally classified into three groups:
- The possible symptoms: changes in her body that a woman can identify for herself and tell you about, which may mean she is pregnant, but they could also be caused by something else. You only have the woman’s subjective report on which to base your diagnosis. However, at Health Post level, the possible symptoms are often all the evidence that is available to you in the first three to six months.
- The probable signs and symptoms: some of these indicators are reported by the woman, but you can also see them for yourself. There is also a pregnancy test that you may be able to conduct, or that could be done at the next level health facility.
- The positive signs: these are absolute proof of pregnancy, based on objective findings.
8.2.1 Possible symptoms of pregnancy
The possible symptoms commonly reported by women in the early stages of pregnancy are sometimes also called ‘presumptive signs’ because pregnancy is often ‘presumed’ by the health professional on the basis of these subjective reports. But it is important to remember that they are only possible indicators of pregnancy.
Missing a menstrual period (amenorrhoea)
Amenorrhoea is pronounced ‘ay men oh ree ah’.
Missing a menstrual period is often the first symptom that women notice when they become pregnant. If the woman tells you that she has missed a menstrual period (amenorrhoea), or stopped menstruating altogether for some months, it is a fairly good indicator of conception in women who usually have regular menstrual cycles. Other possible causes of amenorrhoea are poor nutrition, emotional troubles, or the menopause (change of life) in older women.
Breast changes
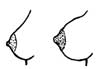
Pregnant women may report feelings of breast tenderness, fullness, tingling and enlargement and darkening of the areola (the darker circle of tissue around the nipple). During early pregnancy, the glands of the areola enlarge as a result of hormonal stimulation, and the breasts gradually get bigger to prepare to make milk for the baby. But note that breasts often get bigger just before the monthly menstruation in women who are not pregnant.
Nausea and vomiting
This common symptom occurs in approximately 50% of pregnancies during the first three months. It is usually most severe in the morning, which is why this feeling is often called morning sickness. But it can occur at any time and may be stimulated by cooking odours and spicy smells. Some pregnant women feel nauseous all day. Other possible causes of this symptom are illness or parasites. Severe, frequent vomiting is a danger symptom because the woman can lose weight rapidly. You will learn more about this in Study Session 12.
Tiredness
Women in early pregnancy may report feeling tired and sleepy during the day, and wanting to rest more often than usual when doing their work. Other possible causes are anaemia (see Box 8.1), poor nutrition, emotional troubles, or too much heavy physical work.
Box 8.1 Anaemia
Anaemia is a blood condition that can make a person feel tired all the time. The blood contains red cells which carry oxygen around the body, delivering it to the muscles and organs where they use it to make energy. A person with anaemia doesn’t have enough red blood cells, so their body is short of oxygen and it can’t make enough energy for normal activity. There are several causes of anaemia, but the most common is shortage of iron in the diet. Iron is needed to make new red blood cells. Anaemia causes problems in pregnancy and birth, but it can be prevented by eating enough foods with protein and iron in them. Pregnant women need a lot of iron so they are routinely given iron tablets. You will learn about nutrition in pregnancy in Study Session 14. The diagnosis and treatment of anaemia is covered in Study Session 18.
Frequent urination
Pregnant women often report needing to urinate more frequently particularly during the first three months and the last one or two months of pregnancy. Other possible causes of this symptom are stress, a bladder infection, or diabetes (blood sugar disease). You will learn about diagnosing diabetes in Study Session 9, and bladder infections in Study Session 18.
Quickening
Most pregnant women start to feel their baby moving very lightly inside them before they are half-way through the pregnancy. This feeling is known as the baby ‘quickening’. Women who have had a baby before are sensitive to these tiny movements sooner than women who are pregnant for the first time. The first perception of fetal movement usually occurs at 18–20 weeks of pregnancy in primigravidas (women who are pregnant for the first time), but it can be as early as 14–16 weeks in multigravidas (women who have had more than one pregnancy). Another possible cause of this symptom is gas in the belly.
Chloasma (or the ‘mask of pregnancy’)
Chloasma is pronounced ‘klo az mah’.
Darkening of the skin over the forehead, bridge of the nose, or cheekbones, is called chloasma. It is most marked in women with dark complexions (Figure 8.2). Darker patches may also appear on the breast and the belly, especially along the mid-line below the navel. Signs of chloasma usually occur after 16 weeks gestation, (four months of pregnancy) and are intensified by exposure to sunlight, but these changes in the skin are not reliable indicators of pregnancy.
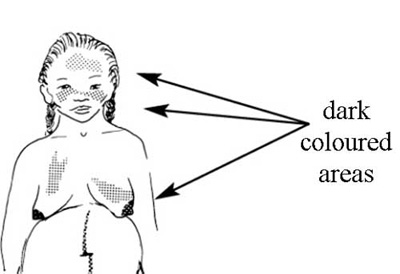
Could you conclude that a woman was definitely pregnant if she had all of the above symptoms?
You could not be certain that she is pregnant, because some normal bodily changes or health problems have the same manifestations as these possible symptoms of pregnancy.
8.2.2 Probable signs and symptoms of pregnancy
These are more reliable than the possible symptoms, but they are not certain indicators of pregnancy.
Abdominal enlargement
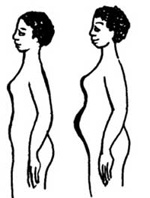
There is progressive enlargement of the abdomen (belly) from 7 to 28 weeks of pregnancy. At 16 to 22 weeks, growth may appear more rapid as the uterus rises higher into the abdomen.
Can you suggest other possible causes of abdominal enlargement?
The most obvious is that the woman is just getting fatter. But you should also consider whether she could have a cancer, or another type of growth in her belly.
Pregnancy test for human chorionic gonadotropin (HCG)
Chorionic is pronounced ‘korr ee onn ik’. Gonadotropin is pronounced ‘gonn add oh troh pinn’.
This hormone is produced by a part of the embryo only 8 days after conception, and by the placenta throughout pregnancy. It can be detected by chemical tests that can usually only be done at higher-level health facilities. Pregnancy testing kits may be purchased from some pharmacies, but they are expensive.
The hormone can be detected in the mother’s blood and urine eight to ten days after conception, or 40 days after the last menstrual period. When people refer to a ‘pregnancy test’, the urine test for HCG is usually what they mean. Although it gives a good indication of pregnancy in most cases, the testing kits may give a false result, especially if they have not been stored properly, or are out of date. Also there are some disease conditions that result in secretion of HCG.
Painless uterine contractions
As the uterus enlarges, it becomes globular (round) and often rotates to the right. Painless uterine contractions are felt as tightening or pressure. They usually begin at about 28 weeks’ gestation and increase in regularity. These contractions usually disappear with walking or exercise, whereas true labour contractions become more strong and powerful.
8.2.3 Positive signs of pregnancy
A positive diagnosis of pregnancy can be made on the basis of these signs, which are sometimes called ‘sure’ signs. They cannot generally be detected until after the first 3 months of pregnancy.
Fetal heart tones (FHTs)
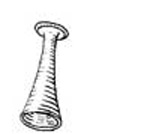
The normal fetal heart rate is 120-160 beats per minute. The heartbeat may be detected from 18-20 weeks’ gestation by placing a fetoscope (Figure 8.3) on the woman’s belly and listening. You will learn how to do this in Study Session 11 and your practical skills training. Hospitals sometimes have a machine called a hand-held Doppler that can detect fetal heart tones as early as 10 weeks’ gestation.
Palpation of the fetus
You should be able to feel (palpate with your hands) fetal movements through the mother’s abdominal wall at about 18 weeks of pregnancy, and after 22 weeks the fetal outline can be felt. You will learn how to do this in Study Sessions 10 and 11 and your practical skills training.
Ultrasound examination
Ultrasound examination (or sonography) is one of the most useful technical aids in diagnosing and monitoring pregnancy, but it can only be done in a health facility with the right equipment. Sound waves that are so high you cannot hear them are passed through the mother’s abdomen by the machine and they ‘bounce’ back off the baby. A computer turns these sound waves into an image of the fetal outline; the placenta and umbilical cord can also be seen. Fetal wellbeing can be monitored by ultrasound as the pregnancy progresses.
Which of the signs and symptoms of pregnancy in Sections 8.2.1 to 8.2.3 can you use in your kebele to help you diagnose pregnancy at the community level?
You can base your diagnosis on a combination of the possible symptoms that women tell you about (amenorrhoea, breast changes, nausea and vomiting, especially morning sickness, frequent urination, tiredness in the daytime, quickening of the fetus, and chloasma); and the probable signs and symptoms of abdominal enlargement and the woman experiencing painless uterine contractions. The positive signs that you can detect at community level at 18 to 22 weeks’ gestation are hearing fetal heart tones with a fetoscope, and palpating the fetus through the mother’s abdominal wall.
Activity 8.1 Asking questions about possible symptoms of pregnancy
In your Study Diary, write down the questions you would ask a woman if you are trying to find out if she is possibly pregnant. Remember to use respectful language and words that she will understand.
Discuss your questions with your Tutor at your next Study Support Meeting.
This activity relates to Self-Assessment Question 8.5 at the end of this study session.
8.3 Identifying possible risk factors in pregnancy

Let’s assume you have decided that a woman is probably pregnant, and that you need to take her health history in order to plan her antenatal care. An important aim of history taking is to identify whether she has any risk factors that could lead to complications during the pregnancy, or at labour and delivery, or in the postnatal period. Asking clearly focused questions will help you do this.

8.3.1 How old is she?
Pregnancy can cause problems for women of any age. But very young women and much older women tend to have more problems.
Girls who become pregnant before they are 17 years old may not have finished growing themselves. A girl’s pelvis might not be grown enough to give birth normally. Girls are more likely to have other problems too — like pre-eclampsia (see Box 8.2), long labours, and babies born too early. Girls who get pregnant when they are very young can be wonderful and caring mothers, but many of them will need extra advice and support.
It may be safer for older women and very young women to give birth in a well-equipped health facility rather than at home.
Older mothers may also have more problems in pregnancy and birth.
Box 8.2 Pre-eclampsia and eclampsia
Pre-eclampsia is a serious condition characterised by high blood pressure (hypertension), swelling of the hands, feet and even the face, and significant amounts of protein in the urine (proteinuria). It usually develops in the last 3 months of pregnancy. Women with this condition feel very unwell, often reporting severe headaches, nausea and vomiting.
![]() If you suspect a pregnant woman may be developing pre-eclampsia you should refer her to the nearest health facility immediately.
If you suspect a pregnant woman may be developing pre-eclampsia you should refer her to the nearest health facility immediately.
If untreated, pre-eclampsia can progress to eclampsia, in which all of the above symptoms worsen and the woman develops mental confusion, visual disturbances and convulsions (fits). Eclampsia is life-threatening for the woman and her unborn baby.
Eclampsia, pre-eclampsia, and other types of diseases due to high blood pressure, are known as hypertensive disorders of pregnancy; they are discussed in detail in Study Session 19.
8.3.2 How many children has she had?
Women who have already had one or two babies, and whose children were born alive and healthy, usually have the fewest problems giving birth. Other women may have more problems. First births are often more difficult than later births. Watch carefully for danger signs and have transportation available for emergencies.
![]() For these reasons, it may be safer for a woman who is having her first baby, or who has had five or more babies already, to give birth in a health facility.
For these reasons, it may be safer for a woman who is having her first baby, or who has had five or more babies already, to give birth in a health facility.
8.3.3 Has she had any miscarriages?
Some women have one miscarriage after another, and you may not know why. Refer her to the nearest health facility to find the cause, and to help her carry this pregnancy all the way through.
A miscarriage (spontaneous abortion) is when a pregnancy ends before the woman is 28 weeks’ pregnant, while the baby is still too small to live outside the mother without very specialised hospital intensive care. Spontaneous abortion is common and often happens before the woman even knows she is pregnant.
It is usually difficult to know why a miscarriage happens, but some causes of miscarriage are preventable. Malaria, sexually transmitted infections, injury, violence and stress can all cause a pregnancy to end spontaneously. Sometimes miscarriages happen because a woman has been near poisons or toxic chemicals. For example, women who work on farms often breathe or handle pesticides, and they tend to have more miscarriages than women who are not exposed to chemicals. Some miscarriages can be prevented by treating women for illness or infection, or by helping them to avoid exposure to chemicals or violence.
8.3.4 Has she ever had an abortion?
A woman who was sick, injured, or bled heavily after any kind of abortion, may have scars in her uterus that could cause problems in this pregnancy or birth. It is probably safer for her to give birth in a hospital.
If a person, or the woman herself, does something to her body to end a pregnancy, this is called an abortion. Where abortion is legal and available, a woman can have a safe abortion that will not usually endanger her future pregnancies.
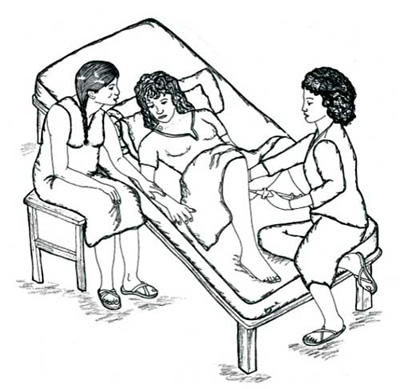
In places where abortion is illegal, a woman trying to end a pregnancy may harm herself, or turn to someone who does not give abortions safely (Figure 8.4). Unsafe abortions can cause heavy bleeding, serious infection, infertility, or even death. Study Session 20 will teach you how to help a woman after an unsafe abortion.
8.3.5 Has she had any problems with past pregnancies or births?
If a woman has had problems with past pregnancies or births, she may have problems with this birth too. Ask the mother to tell you the story of each of her past pregnancies and births. Let her tell you everything: the good and bad. Then ask the following questions to learn more about problems in past pregnancies, and what to be prepared for during this one. Write down what you learn. All these problems are explained more fully in other study sessions in this Module.
Was she tired or weak or anaemic?
Extreme tiredness or weakness in pregnancy is usually caused by anaemia (see Box 8.1 earlier). If she had anaemia in another pregnancy, she is likely to have it again this time.
Did she have high blood pressure, swelling or convulsions?
If she had high blood pressure in a past pregnancy, she is likely to get it again. High blood pressure can be a sign of pre-eclampsia (see Box 8.2 earlier). Check her blood pressure and other signs of pre-eclampsia regularly and be prepared to refer her to a hospital if it develops.
![]() If she had convulsions in a past pregnancy or birth, she probably had eclampsia (Box 8.2), and she should definitely give birth in a hospital.
If she had convulsions in a past pregnancy or birth, she probably had eclampsia (Box 8.2), and she should definitely give birth in a hospital.
Did she have diabetes?
If she had diabetes (too much sugar in the blood) in a past pregnancy, she is more likely to get it again. When blood sugar is too high, some of it gets into the urine when the blood is filtered in the kidneys. You should be able to test a pregnant woman’s urine to see if there is sugar in it. (We teach you how to do this in Study Session 9.) A more reliable test can be done at a health facility. Diabetes can lead to miscarriage, or other problems with the mother or baby after birth.
Did she have a very long labour or a long pushing stage?
Was her labour longer than 24 hours for a first baby, or longer than 12 hours for other babies? Did she push for more than two hours? Was the baby in a difficult position or very big? Was she very afraid? Ask if her long labour caused problems for her or her baby. If that birth was safe for her and the baby was OK, then she will probably not have a problem with this birth. If that birth was difficult, ask her if she knows why the labour was long. Did she have anaemia?
Did she have fistula?
If she had a long labour, did it cause a fistula (an abnormal opening communicating between the vagina, and either the urinary bladder, or the rectum, or the urethra, or the ureter)? This is more likely to happen in women who had the harmful traditional practice of female genital mutilation when they were children. Urine or stools pass through the fistula into the vagina and leak out continuously, unless the fistula is closed by a surgical operation.
![]() Past history of a fistula means she should definitely have this birth in a hospital.
Past history of a fistula means she should definitely have this birth in a hospital.
Did she have a very short labour (less than 3 hours)?
If the mother had a very short labour in the past, make sure that she and her family know what to do if you do not get there in time, and they cannot get her to a health facility. You can teach the family how to deliver a baby in an emergency. You will learn how to do this in the next Module, Labour and Delivery Care.
Did she have an early birth?
If she had a baby born more than a month early, ask her if she had a discharge from her vagina. This could be a symptom of a vaginal infection, which can lead to early births. Be ready in case this baby is early too, and watch for signs of labour, described in the next Module, Labour and Delivery Care.
Did she have a small baby (less than 2.5 kilograms or 5 pounds)?
Find out if the baby was born early (it is normal for early babies to be small). If the baby was small but it came on time, ask the mother if she had anaemia (Box 8.1), high blood pressure, or pre-eclampsia (Box 8.2). Also ask if she had enough to eat, or if she smoked cigarettes, or used drugs. Any of these things could have made the previous baby small.
Check the size of her abdomen to see if this baby is growing normally. (You will learn how to do this in Study Session 11.) If you think this baby may be very small for its gestational age, the mother should give birth in a hospital, because small babies can develop more health problems than normal weight babies. (The Module on Postnatal Care will explain why, and what you can do to help.)
Did she have a big baby (over 4 kilograms or 9 pounds)?
Ask if the birth was difficult. If it was not, this birth will probably be OK too. But having a large baby may be a sign that the mother has diabetes. Check carefully to see if this baby seems big too. Test her urine for sugar, and if possible have the mother tested for diabetes in a health facility.
Can you explain why the baby may grow large if the mother has diabetes?
We said earlier that diabetes in the mother causes too much sugar in her blood. The baby is fed by nutrients from her blood, so it gets too much sugar and may become fat.
Did she have heavy bleeding before or after the birth?
If she bled a lot in a past pregnancy or birth, it is more likely to happen again. Ask her to tell you as much as she can remember about her bleeding. Did she need medical help? Was she anaemic afterwards? Was she too weak to stand? The answers to these questions will help you prepare for what may happen at this birth. Be ready to treat her for heavy bleeding after the birth. The Module on Labour and Delivery Care will explain how to do this.
![]() If possible, a woman who bled heavily before should have this baby in a hospital.
If possible, a woman who bled heavily before should have this baby in a hospital.
Did she have any problems with the placenta (afterbirth)?
It is better if a woman who had a retained placenta after a previous birth gives birth in a hospital next time.
If the woman’s placenta did not come out easily in a past birth, she may have the same problem again. Tell her to watch out for signs of bleeding during this pregnancy, and to seek help from a health professional immediately if it happens.
Did she have a fever or infection of the vagina or uterus?
This birth may be fine, but if she had an infection of the vagina or uterus during or after a previous birth, she has more risk of infection again this time. Be sure to check her for signs of vaginal infection. (Study Session 9 explains how to do this.)
Was she very sad (depressed) after the birth?
Postnatal depression is a serious health problem and she must be referred to the next level health facility.
If a woman became depressed after a past birth, it may happen again. Be prepared to help if this happens. (Counselling is covered in Study Session 14.)
Did the baby get sick or die before, during or after the birth?
If you think there may be a risk to her next baby, refer her to the nearest health facility.
Find out everything you can about the circumstances of the baby’s sickness or death. If the woman was seen by health professionals at the time, what did they tell her had caused it? Does she have her own ideas about what happened, and why?
Did her baby have birth defects?
Some birth defects just happen and no one knows why. Others run in the family. Ask about the type of birth defect and if anyone else in her or the baby’s father’s family has that birth defect. The next baby may have the same problems. Some defects are caused by illnesses like herpes or rubella. If the woman had herpes or rubella in a past pregnancy, reassure her that these infections will probably not cause birth defects in this pregnancy. Pregnant women should try to avoid contact with people who are sick. Other causes of birth defects are exposure to toxic chemicals, drugs or medicines, or they may be due to poor nutrition during the pregnancy. Eating a healthy diet in pregnancy is covered in Study Session 14.
Did she have caesarean surgery (birth by operation)?
In caesarean surgery a doctor cuts open the woman’s belly and uterus to get the baby out. Sometimes a caesarean surgery is done because the baby does not fit through the mother’s pelvis. Sometimes it is done because the baby is in danger and must be born very quickly. After the baby is out, the doctor sews the uterus and belly closed. This leaves one scar on the uterus and a second scar on the belly (Figure 8.5).
![]() It is safest for a woman who has had a previous caesarean to give birth in a hospital again next time.
It is safest for a woman who has had a previous caesarean to give birth in a hospital again next time.
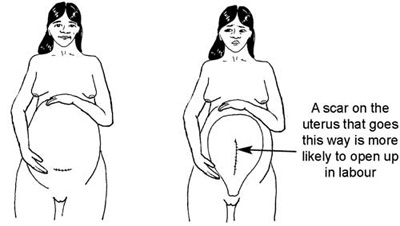
Most women can have a safe vaginal birth even if they had a caesarean birth with a previous baby. But there is a very small chance that the scar on the uterus may tear open (rupture) during labour. If this happens, the woman will bleed inside and she and her baby could die.
8.3.6 Does she have any other health problems?
Most women are in good health and are able to give birth without risk to themselves or their babies. However, it is an important part of your role as a health professional to identify women who are at higher risk because they have a current or past health problem. If a pregnant woman is sick with any of the following problems, now or in the past, she should get medical help to plan for her needs during pregnancy, and decide if she should give birth in a hospital:
- Diabetes
- HIV/AIDS
- Bladder or kidney infection
- Malaria
- Fever over 37.5°C (100.4°F) for more than two days, or frequent fevers
- High blood pressure
- Pre-eclampsia or eclampsia
- Liver disease (hepatitis, especially hepatitis B)
- Heart problems
- Untreated tuberculosis (TB)
- Deformity of the hips or lower back.
8.3.7 Questions of your own
You probably have some questions of your own that you want to ask the pregnant women you meet, but that we did not include in this study session. For example, if there is hepatitis B in your community, you may want to ask the woman if she has hepatitis B, or tell her how to prevent it. Think about the information you need to know in order to give her good antenatal care, and prepare for labour, delivery and the postnatal period.
Later in this module, Study Session 13 will explain the detailed schedule of four antenatal visits recommended for focused antenatal care (FANC), and the guidelines on what to cover in each visit. You will learn how to make clear, systematic notes on the integrated care card that you will complete every time you visit a pregnant woman, and during her labour, delivery and postnatally. But first you need to know how to examine her and her baby, as the next study sessions describe.
Summary of Study Session 8
In Study Session 8, you have learned that:
- It is important to maintain the trust of the woman when you question her about her health history; keep your notes confidential and don’t tell anyone else what she says.
- The questions you ask should be respectful and in accessible language the woman can understand.
- Making a pregnancy diagnosis is based on a combination of possible symptoms reported by the woman, and probable and positive signs and symptoms that you observe yourself, or which can be confirmed by a physical examination or chemical test.
- The most commonly reported possible symptoms of early pregnancy are stopping monthly bleeding; breast changes; nausea and vomiting, especially in the morning; feeling tired during the day; urinating more often; quickening (feeling light movements of the baby); and chloasma.
- The probable signs and symptoms of pregnancy are abdominal enlargement; a positive pregnancy test for the hormone HCG; and painless uterine contractions. The positive (sure) signs are detection of fetal heart tones; palpation of the fetus; and visual confirmation by ultrasound examination, where facilities exist.
- Very young or older women, first-time mothers, and women who have had many previous births are more likely to experience antenatal problems, and should generally be referred to a health facility for labour and delivery.
- It is important to ask the woman clearly focused questions to identify other risk factors, such as, previous miscarriage or abortion; very large or small babies at birth; a prolonged or very short labour; a fistula; caesarian surgery or heavy bleeding before or after the birth; retained placenta; postnatal depression; a baby who died or had birth defects; or a history of medical conditions such as high blood pressure, diabetes, anaemia, pre-eclampsia or eclampsia, infections, and heart, kidney or liver problems.
Self-Assessment Questions (SAQs) for Study Session 8
Now that you have completed this study session, you can assess how well you have achieved its Learning Outcomes by answering the questions that follow Case Study 8.1. Write your answers in your Study Diary and discuss them with your Tutor at the next Study Support Meeting. You can check your answers with the Notes on the Self-Assessment Questions at the end of this Module.
Case Study 8.1 Is Mrs X pregnant?
Mrs X is 39 years old and has been married for 15 years. She has one child who was born 10 years ago and she is hoping very much that at last she is pregnant again. Mrs X says she and her husband have not used contraception and she doesn’t think she has had any miscarriages in that time. She hasn’t had her monthly bleeding for the past nine weeks. When you ask her about any changes in her body since her last menstrual period, she says she hasn’t noticed anything, but she has been feeling nauseous when she first gets up in the morning and she is more tired than usual. Mrs X tells you that her first baby was born after a labour of 30 hours and he weighed 4 kilograms. She also remembers that she was given iron tablets to take, but she doesn’t know why.
SAQ 8.1 (tests Learning Outcomes 8.1, 8.2 and 8.4)
- a.What is wrong with asking Mrs X ‘In your previous pregnancy, did you have pre-eclampsia’?
- b.How could asking the question in those words damage her trust in you?
- c.Rewrite this question to avoid causing the problems you identified.
Answer
- a.Someone who is not a health professional is unlikely to know what ‘pre-eclampsia’ means, so she won’t understand the question. She might say ‘no’ because she doesn’t want you to think she is ignorant. You could miss learning vital information about her risk factors if your questions are not accessible.
- b.She may worry that you will think she is stupid because she doesn’t know this medical term. This may make her uncomfortable about sharing personal information with you.
- c.We don’t know exactly how you rewrote the question (there are various equally good ways of saying it), but you might have used words like this:
‘In your previous pregnancy, did a health professional ever tell you that your blood pressure was high, or that you had protein in your urine? Did you ever experience bad headaches, nausea or vomiting, and swelling of your feet, hands or face?’
SAQ 8.2 (tests Learning Outcome 8.3)
- a.What are the possible symptoms of pregnancy in Mrs X’s case study?
- b.Is there anything in her history that suggests she may not be pregnant?
- c.How could she find out quickly whether she probably is pregnant?
Answer
- a.Mrs X reports three possible symptoms of pregnancy: amenorrhoea (no period for nine weeks); nausea in the mornings; and abnormal tiredness during the day.
- b.She has wanted another baby for the past ten years, but despite not using contraception she has not conceived, so she may not be pregnant now.
- c.The quickest way to find out if she is pregnant would be to go to the nearest health facility, where they could do a pregnancy test on her urine to see if it contains the hormone HCG, which is produced by the embryo and placenta. This test is not conclusive, but it is a probable sign of pregnancy.
SAQ 8.3 (tests Learning Outcome 8.5)
If Mrs X’s pregnancy is confirmed, do any of the features of her history suggest that she should be advised to give birth in a health facility this time? Explain why or why not.
Answer
If Mrs X is pregnant, she should be advised to give birth in a health facility this time, because of her age (she is an older mother at 39 years); she had a long first labour (over 24 hours); and her first baby was large (4 kg). All three risk factors make it more likely that she will have difficulties in delivering her second baby.
SAQ 8.4 (tests Learning Outcomes 8.1 and 8.5)
Explain why Mrs X was given iron tablets during her previous pregnancy. Is this a sign that she had a serious risk factor at that time?
Answer
Mrs X was given iron tablets during her first pregnancy as a routine precaution against her developing anaemia (shortage of red blood cells). Iron boosts the supply of red blood cells to carry oxygen around her body and that of the growing baby. All pregnant women should ideally be given iron tablets, so this is not a sign of a serious risk factor in Mrs X’s case.
SAQ 8.5 (tests Learning Outcome 8.4)
What questions did you write in your Study Diary when you completed Activity 8.1? Did you take care to use language that women in your community can understand?
Answer
We can’t predict exactly what questions you wrote in your Study Diary, or what words you used, so your questions could be a bit different from ours (below), and still be equally good. The important point is that the language you used should be understandable by the women in your community. You should ask questions such as the following:
- When was your last monthly bleeding? Have you missed a month yet?
- Have your breasts got any larger recently, or do they feel tender?
- Have you felt sick, especially in the mornings when you wake up?
- Have you felt unusually tired or sleepy during the day?
- Have you needed to pee (pass water) more than usual?
- Have you felt any light movements in your belly?
- Has your belly got any bigger lately?
