Use 'Print preview' to check the number of pages and printer settings.
Print functionality varies between browsers.
Printable page generated Thursday, 14 May 2026, 8:19 PM
Antenatal Care Module: 19. Hypertensive Disorders of Pregnancy
Study Session 19 Hypertensive Disorders of Pregnancy
Introduction
Hypertensive disorders of pregnancy are one of the three leading causes of maternal morbidity and mortality (together with haemorrhage and infection). The contribution of hypertension (high blood pressure) to mortality and morbidity of the fetus and newborn is also immense. Hypertensive disorders may complicate up to 10% of all pregnancies, with the highest proportion occurring in women who are pregnant for the first time (primigravida). Hypertension is usually defined as blood pressure above 140/90 mmHg, where the top number is the systolic pressure and the bottom number is the diastolic pressure.
Blood pressure is measured in millimetres of mercury (mmHg) because the original instruments contained a column of mercury.
Do you remember what systolic and diastolic pressure refer to?
The systolic pressure is the pressure of blood in the blood vessels at the moment when the heart contracts. The diastolic pressure is measured when the heart relaxes between beats.

A major purpose of your antenatal care service is to make pregnant women aware of the danger symptoms of hypertensive disorders, to check their blood pressure at every antenatal visit (you learned how to do this in Study Session 9), and to make a timely diagnosis of hypertension and refer affected women as early as possible.
In this study session you will learn about the changes in the woman’s body as a result of hypertension and how this affects the mother and the fetus, the classifications of hypertension, the common risk factors for developing it, how to diagnose the different types and what actions to take in order to prevent worsening complications and even death.
Learning Outcomes for Study Session 19
After studying this session you should be able to:
19.1 Define and use correctly all of the key words printed in bold. (SAQs 19.1, 19.2 and 19.3)
19.2 Briefly describe what happens in blood vessels and body fluids in women with hypertension, and how this can damage the fetus. (SAQs 19.1 and 19.2)
19.3 Define the different types of hypertensive disorders of pregnancy. (SAQ 19.2 and 19.3)
19.4 List the common risk factors for developing pregnancy-related hypertension. (SAQ 19.3)
19.5 Describe the common clinical features of severe pre-eclampsia. (SAQ 19.3)
19.6 Identify the common maternal and fetal/neonatal complications of hypertensive disorders of pregnancy. (SAQ 19.3)
19.7 Provide basic supportive treatment and facilitate early referral, in particular for women with severe hypertensive disorders of pregnancy. (SAQ 19.3)
19.1 How does hypertension affect pregnancy?
The underlying cause of hypertension related to pregnancy remains unclear. However, hypertension is known to contribute to disorders in different parts of the body; in particular, it affects the brain and spinal cord, the heart and blood vessels, the blood, the kidneys and the liver.
19.1.1 Effects on blood vessels and body fluids
A well-known phenomenon in a woman who develops hypertension during pregnancy is that the muscular walls of the blood vessels all over her body contract, so the space inside the vessels becomes smaller. (The technical name for this is generalised vasoconstriction.) The constriction causes high blood pressure in the blood vessels, and this is one reason why fluid from the blood is pushed out through the vessel walls and collects in the woman’s tissues.
What is the name for the swelling due to fluid collecting in the tissues and where is the swelling most often visible in pregnant women with hypertension? (You learned about this in Study Sessions 7 and 8, particularly Box 8.2.)
The swelling is called oedema and is a warning sign of hypertension in pregnancy. It is most often see in the lower legs, ankles and feet; also the hands, and in the most severe cases in the face and back.
19.1.2 Effects of maternal hypertension on the fetus
Any form of hypertension during pregnancy has a significant effect on fetal growth and survival. This happens because of the marked reduction in the mother’s blood volume, which will in turn reduce the blood supply from the endometrial arteries into the placenta. The endometrial arteries bring the mother’s blood into the placenta, delivering oxygen from her lungs and nutrients from her digestive system to the fetus. (You can see them if you look back at Figure 5.5 in Study Session 5.)
If the maternal blood flow into the placenta is reduced, what effect will this have on fetal development?
The transfer of oxygen, nutrients and fluids to the baby will be reduced, so it will not develop normally. Fetal growth is likely to be restricted (hypertension during pregnancy is one of the common causes of intra-uterine growth restriction, IUGR).
The amount of amniotic fluid surrounding the fetus will also be much less than normal, because the blood flow to the baby’s kidneys is reduced, so it makes less urine. In late pregnancy, most of the amniotic fluid comes from the baby’s urine. The fetus may die due to deficiency of oxygen and nutrients, or due to significant reduction of amniotic fluid. If the fetus lives very long in the uterus with a reduced oxygen supply, the growing brain is very likely to be dangerously affected. As a result, if the baby is born alive and survives early childhood, mental retardation can appear when it is older.
The fetus may also die because the placenta gets aged too early and the blood supply is inadequate, so there can be early separation of the placenta from the wall of the uterus. (Early detachment is called placental abruption and you will learn all about it in Study Session 21. Preterm labour may begin spontaneously (Study Session 17), and the mother’s life can also be at risk due to severe placental abruption where much blood may be lost.
19.1.3 Common complications of severe pre-eclampsia for the mother
Complications of any type of hypertensive disorder for the mother are highly related to the generalised vasoconstriction and body fluid redistribution (more outside the blood vessels and less inside the vessels). These phenomena result in:
- Inadequate blood supply to her vital organs (brain, heart) and less vital organs for short survival (kidneys, gastrointestinal tract including liver, skeletal muscles and skin).
- Fluid accumulating in her organs (liver, brain, abdominal cavity, eyes, lungs), which swell and can even rupture.
- Narrow or constricted blood vessels, which contributes to blood cell damage, particularly platelets (essential for blood clotting if there is a tear or wound in the tissues), and red blood cells.
If a significant proportion of the woman’s red blood cells are damaged, what condition will she develop?
She will develop anaemia.
19.1.4 Summarising maternal and fetal complications of severe pre-eclampsia
Asphyxia is pronounced ‘ass-fix-ee-ah’.
‘Acute’ refers to a condition that begins suddenly and rapidly becomes very serious.
| Maternal complications | Fetal complications |
|---|---|
| Eclampsia | Placental abruption |
| Intracranial haemorrhage (bleeding inside the skull) | Intrauterine asphyxia (severe shortage of oxygen in the uterus) |
| Anaemia | IUGR (intrauterine growth restriction) |
| Low platelet count, poor blood clotting and risk of bleeding | Premature delivery |
| Acute kidney failure | IUFD (intrauterine fetal death) |
| Acute liver failure, maybe even liver rupture | Respiratory distress after birth(early neonatal asphyxia) |
| Fluid in the lungs (pulmonary oedema) | Mental retardation |
| Heart failure | |
| Temporary total blindness |
19.2 Classification of hypertension during pregnancy
Hypertension during pregnancy can be a new development, or a continuation or worsening of hypertension that existed before the pregnancy. If the hypertension is diagnosed before pregnancy or during the first 20 weeks of gestation, or if the hypertension persists for six weeks after the baby is born, it is defined as chronic hypertension.
‘Chronic’ describes a condition that has been going on for a long time.
The reason for classifying hypertension during pregnancy is to enable you to decide what actions to take in each case. Some types (e.g. mild pre-eclampsia and gestational hypertension — see Table 19.2 below) have fewer and less severe complications for the mother and the fetus: other types (e.g. severe pre-eclampsia and eclampsia) can have fatal complications unless managed quickly.
19.2.1 Classification of pre-eclampsia
Pre-eclampsia is the commonest type of hypertensive disorder of pregnancy and the focus of much of the discussion in this section (see Table 19.2). It usually occurs in the second half of pregnancy (after 20 weeks of gestation, but most commonly after 28 weeks). The appearance of protein in the woman’s urine (proteinuria) is a danger sign. Significant proteinura is defined as a positive urine dipstick test for protein with a result greater than or equal to +2 on the scale supplied with the dipsticks.
Proteinuria is pronounced ‘proh-teen-you-ree-ah’.
You will learn about these symptoms of severity in Section 19.4 later.
| Type | Raised blood pressure (measured twice, 6 hours apart) | Proteinuria | Symptoms of severity |
|---|---|---|---|
| Gestational hypertension (develops during pregnancy, resolves afterwards) | Above 140/90 mmHg | No significant proteinuria | None |
| Mild pre-eclampsia | Between 140/90 and 160/110 mmHg | No significant proteinuria | None |
| Severe pre-eclampsia | Greater than or equal to 160/110 mmHg | With or without significant proteinura (urine dipstick test result greater than or equal to +2) | Headache, blurred vision, epigastric burning pain, decreased urine output, decreased or absent fetal kick |
| Superimposed pre-eclampsia | Higher than before the pregnancy in a known chronic hypertensive woman | Significant or worsening proteinuria | With or without symptoms of severity |
19.2.2 Diagnostic signs of eclampsia
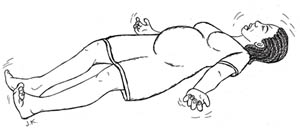
Eclampsia is the most severe type of hypertensive disorder. The diagnosis is made when a woman with pre-eclampsia (most commonly), or any other type of hypertensive disorder, develops convulsions (fits or seizures, Figure 19.1) or coma (complete loss of consciousness). The convulsion looks like the seizure you might have witnessed in a person with epilepsy (in Amharic: Yemitil Beshita). You will learn more about this type of convulsion later in this study session.
19.3 Risk factors for pre-eclampsia/eclampsia
In the majority of cases, the occurrence of pre-eclampsia or eclampsia is unpredictable and the cause is unknown. However, there are some risk factors which are known to be associated with hypertensive disorders of pregnancy (Box 19.1).
Box 19.1 Common risk factors for hypertensive disorders in pregnant women
- First time pregnancy before the age of 20 years or after 35 years
- Multiple pregnancy (twins or more)
- Family history of pre-eclampsia/eclampsia in close female relatives
- History of pre-eclampsia/eclampsia in the previous pregnancy
- Diabetes currently
- Obesity currently (woman is very overweight for her height)
- Kidney disease currently.
Knowing these risk factors will help you to:
- Anticipate the possibility of a hypertensive disorder and its complications developing before they actually happen.
- Offer counselling to the woman and her partner and family about the danger symptoms of severe pre-eclampsia/eclampsia, so they can take action quickly if needed.
- Make antenatal care visits more frequently in late pregnancy to women with known risk factors.
Equally important, you need to know that any woman (regardless of age and number of previous deliveries) can develop a hypertensive disorder in any pregnancy. Therefore, although it is good to anticipate its occurrence in those who have one of the risk factors, you should assume that all pregnant women have the potential to develop hypertension.
19.4 Clinical features of severe pre-eclampsia.
As you saw in Table 19.2, mild pre-eclampsia is an incidental finding of raised blood pressure in a woman who doesn’t have any other hypertensive symptoms. However, a woman with severe pre-eclampsia can have one or more complaints of severe symptoms. From observations and research studies, the following are the common clinical features.
19.4.1 Headache
Although there are many causes of headache during pregnancy, till proved otherwise, you should first consider that a headache could be due to the severe form of hypertension. Brain oedema (swelling due to fluid collecting around the brain) and increased pressure inside the skull (the medical name for the skull is the cranium, so doctors call this intracranial pressure) are the major reasons for the headache in severe pre-eclampsia.
19.4.2 Blurred vision/visual disturbance
Blurred vision and visual disturbances are also because of increased intracranial pressure, coupled with oedema in the brain and in the retina (the structure at the back of the eyeball).
19.4.3 Epigastric pain
Oedema in the liver can become very painful because the liver is covered by a capsule, which becomes tense and painful when the liver accumulates too much fluid in its tissues. The liver lies behind the epigastric area of the abdomen, which you learned to identify in Study Session 15 (look back at Figure 15.4). Other causes of epigastric pain are rare during pregnancy, so the message is: first think of hypertension in a pregnant woman (particularly after 28 weeks of gestation) complaining of epigastric pain.
19.4.4 Decreased urine output
Urine production decreases very significantly in severe types of pregnancy-related hypertension. The reduction in maternal blood volume (described in Section 19.1.1) results in markedly reduced blood flow to the kidneys, and as a result, there will be a significant decrease in urine output. The woman may stop producing urine altogether.
19.4.5 Decreased or absent fetal kick
This happens because the fetus receives a reduced supply of oxygen and nutrients due to the decreased blood flow through the placenta, as described above.
19.4.6 Generalised (pathologic) oedema
Generalised oedema is characterised by the widespread development of oedema in the woman’s back, abdomen, hands and face. The oedema is considered pathologic if the mother’s weight gain per week is above 1.0 kg. The normal weight gain per week during pregnancy is in the range of 0.25 kg to 0.75 kg (average 0.5 kg).
19.5 Clinical features of eclampsia
Eclampsia occurs when the woman hasn’t been able to get adequate treatment when she had severe pre-eclampsia. It is the most life-threatening complication of severe pre-eclampsia. It can occur before labour, during labour and after delivery. Sometimes, eclampsia can occur as long as 24 hours after the delivery, even in women who gave birth with normal blood pressure and without any danger symptoms before and during labour. Therefore, if a woman comes to you with a history of convulsion, after a normal labour and delivery and even some time at home, the first clinical problem you need to consider is eclampsia. But you should also know that there are other medical causes of convulsion, such as blood sugar being too low or too high (hypo or hyperglycaemia), malaria affecting the brain, bacterial infection in the brain (e.g. meningitis), stroke, drugs, or poisoning.
As you learned above, the diagnosis of eclampsia is made when the clinical features of pre-eclampsia are present, plus:
- Convulsion/fits
- Coma in the absence of other causes.
The convulsion in eclampsia is usually sudden in onset, but in some cases there may be warning signs and symptoms that make the occurrence of eclampsia inevitable (see Box 19.2).
Box 19.2 Warning signs and symptoms that eclampsia is developing
- Intractable/severe headache
- Severe epigastric pain
- Markedly blurred vision or total visual loss (temporary)
- Lethargic or very irritable
- Disoriented about the time, people and places in her environment
- Disconnected with the environment
- Shows some abnormal behaviour.
19.5.1 Convulsions in eclampsia
The convulsion in eclampsia is similar to the seizure in people with epilepsy. Like an epileptic fit, it has four phases:
The quiet stage
The typical feature of the first stage is a period of quiet (it may not take more than 20 seconds) when the person has generalised weak muscles, stiffness and twitch, and staring eyes.
The tonic stage
This may last up to 30 seconds and is characterised by a severe form of generalised muscle spasms, where the muscles of the legs and hands contract very severely and may seem as strong as a dry stick. During the tonic stage, the woman stops breathing and becomes short of oxygen. There is also rolling of the eyes where you can see the upper part of the sclera (the white part of the eye).
The clonic stage
The third stage may take up to 2 minutes and is classically a jerky movement of the whole body as a result of vigorous muscle contraction and relaxation. At this stage, the woman can breathe and she will also salivate and urinate spontaneously.
The coma stage
After the clonic stage is over, in typical cases the woman becomes deeply unconscious for an uncertain period of time. However, a woman can be comatose even from the outset (i.e. without even a single convulsion). The duration of the coma state is dependent on:
- The number of previous convulsions: The higher the number, the longer the duration of coma, which may even end in death. Having a history of more than ten convulsions is one of the poor outcome indicators. Therefore, the earlier the convulsion episodes are controlled, the better the prognosis for the mother and the baby.
- Severity of brain oedema: The space between the skull and the brain is very limited. Thus, even a minimal increase in the mother’s brain size due to oedema or haemorrhage will have a serious effect on the brain cells, because the pressure on the brain (the intracranial pressure) rises so high.
- Extent of intracranial haemorrhage (see below in this session): As already described for brain oedema, any bleeding in the intracranial space will increase the intracranial pressure on the brain cells. Additionally, it may aggravate further bleeding and can create a vicious cycle.
- Associated hypoglycaemia (low blood sugar level): Each convulsion requires energy. This is because, during the tonic-clonic stages, almost all the skeletal muscles contract and relax many times. Frequent convulsion means consumption of much energy, which comes from stored sugars in the blood, liver and tissues. The woman with eclampsia cannot replace the sugars used by her muscles quickly enough, so she develops very low blood sugar (severe hypoglycemia), which in turn may manifest in coma. Because her blood sugar is low, the woman with eclampsia invariably will be getting some energy from proteins in her muscles to keep her alive. Breaking down proteins produces ketone bodies that can be used as an energy source and some will appear in her urine. You can test for the presence of ketone bodies with a dipstick.
19.6 What can you do if you diagnose a hypertensive disorder in a pregnant woman?
Your primary role in the management of hypertensive disorders of pregnancy is early identification of warning signs and symptoms, and immediate referral to a hospital or health centre. If possible ensure rapid transportation and reception of the woman at the higher health facility. Your actions should be based on your clinical diagnosis and the severity of the hypertension.
19.6.1 Actions if pre-eclampsia is not severe
Pregnant women diagnosed to have:
- mild pre-eclampsia,
- chronic hypertension
- gestational hypertension
should be referred without any intervention by you, preferably on the day of diagnosis.
Why do you think referral is necessary, even though the hypertension is not severe?
This is because sometimes the mild form of hypertension may progress to the severe type in a very short period of time.
19.6.2 Persuading affected women to go for medical treatment
You should offer counselling to the woman and her family about the danger of maternal and fetal complications and the advantage of getting specialist medical treatment urgently. In cases of eclampsia, people in many parts of rural Ethiopia believe that convulsions/fits are related to an evil spirit. A pregnant woman who has had a fit in these cultures may not want to go to a health facility, because she may prefer to go to the holy water, to a priest or other religious leader, or to local healers. You have a very important role to make sure that the woman and her family understand that the fits are caused by the very high blood pressure she is experiencing. Reassure her that the convulsions will stop progressively after the baby is delivered.
19.6.3 Supportive pre-referral treatment for severe pre-eclampsia
Your second role is providing supportive treatment to avoid worse complications before the woman reaches the health facility. When your clinical diagnosis is as defined in Table 19.2 earlier:
- severe pre-eclampsia
- superimposed severe pre-eclampsia
you should be able to prevent the occurrence of eclampsia by taking the supportive actions in Box 19.2 below.
Box 19.2 Actions to prevent superimposed and severe pre-eclampsia progressing to eclampsia
- Make the referral to the higher health facility as soon as possible.
- Communicate with the receiving hospital or health centre to alert the medical team that a pregnant woman with severe pre-eclampsia is coming for urgent treatment.
- Reassure the woman and her family that when she arrives at the health facility, the doctor will give her drugs to reduce her high blood pressure (anti-hypertensive drugs) and to prevent her from developing convulsions (anti-convulsant drugs).
- While transport is being arranged, insert an intravenous (IV) line into a vein in the woman’s hand or arm, as you will learn to do in Study Session 22 of this Module and in your practical training sessions. Connect the IV line to a bag containing at least 1 litre of IV fluid: either Normal Saline (N/S) or Ringer Lactate (R/L). Never give dextrose in water IV fluid (D/W).
19.6.4 Emergency referral for eclampsia
If you discover a pregnant woman with eclampsia, you should take the actions already described in Box 19.2. Refer her urgently unless she is already in advanced labour — in this case you should deliver the baby and refer her and the baby to a hospital as soon as possible after the birth.
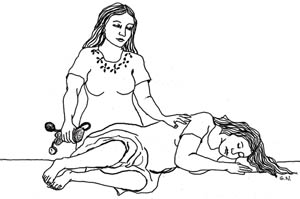
When you transport a woman with eclampsia to the health facility, make sure she is lying on her side with her airway open (Figure 15.2). Don’t let her lie on her back because she may find it difficult to breathe if she has another fit. Lying on her side also means that if she vomits during a fit, she is less likely to breathe the vomit into her lungs.
In the next study session you will learn about another potentially life-threatening situation: abortion and early pregnancy bleeding.
Summary of Study Session 19
In Study Session 19, you learned that:
- Hypertensive disorders of pregnancy are one of the common causes of maternal and perinatal morbidity and mortality.
- Generalised constriction of blood vessels is a fundamental phenomenon of pregnancy-related hypertension. It brings about a marked reduction in the woman’s blood volume, as fluids leave the blood vessels and accumulate in the tissues. Oedema occurs in different tissues and organs (including the brain, liver and kidneys), and leads to a significant reduction in blood supply to different parts of the mother’s body, and to the placenta.
- Known risk factors for pregnancy related hypertension include: being primigravida before the age of 20 years or after 35 years, multiple pregnancies, personal or family history of pre-eclampsia or eclampsia, having diabetes or kidney disease, or being obese.
- Pre-eclampsia (raised blood pressure + significant proteinuria) is the most common type of hypertension during pregnancy. Severe pre-eclampsia is characterised by clinical manifestations such as headache, visual disturbance, epigastric pain, decreased urine output, decreased fetal kick and development of generalised oedema.
- Eclampsia is diagnosed when the pregnant woman develops convulsion or coma in the absence of other causes. It is the leading cause of maternal and fetal death among all types of hypertensive disorders of pregnancy.
- In classical cases, eclampsia has four stages: quiet, tonic, clonic and coma stages.
- The coma stage can be long if there is recurrent convulsion, significant brain oedema, much intracranial haemorrhage or associated hypoglycaemia.
- The very common complications of severe pre-eclampsia include eclampsia, anaemia, low platelet count, multiple and acute failure of organs (kidneys, liver, heart, lungs, and eyes).
- The fetal complications include placental abruption, intrauterine and early neonatal asphyxia (due to low oxygen levels in the blood), intrauterine growth restriction (IUGR) and intrauterine fetal death (IUFD).
- In the management of hypertensive disorders of pregnancy, your primary role is facilitating early referral.
Self-Assessment Questions (SAQs) for Study Session 19
Now that you have completed this study session, you can assess how well you have achieved its Learning Outcomes by answering these questions. Write your answers in your Study Diary and discuss them with your Tutor at the next Study Support Meeting. You can check your answers with the Notes on the Self-Assessment Questions at the end of this Module.
SAQ 19.1 (tests Learning Outcomes 19.1 and 19.2)
Which of the following statements is false? In each case, explain what is incorrect.
A When the muscular walls of the blood vessels all over a woman’s body contract, the space inside the vessels becomes larger so her blood pressure falls.
B Hypertension during pregnancy reduces the blood supply from the endometrial arteries in the mother’s uterus to the fetus via the placenta.
C Hypertension reduces the amount of amniotic fluid surrounding the fetus, because the blood flow to the baby’s kidneys is reduced so it makes less urine.
D Fetal growth is not restricted in a pregnant woman with hypertension.
Answer
A is false. When the muscular walls of the blood vessels all over a woman’s body contract, the space inside the vessels becomes smaller so her blood pressure rises.
B is true. Hypertension during pregnancy reduces the blood supply from the endometrial arteries in the mother’s uterus to the fetus via the placenta.
C is true. Hypertension reduces the amount of amniotic fluid surrounding the fetus, because the blood flow to the baby’s kidneys is reduce so it makes less urine. In late pregnancy, most of the amniotic fluid comes from the baby’s urine.
D is false. Fetal growth is very likely to be restricted in a pregnant woman with hypertension, because the transfer of oxygen, nutrients and fluids to the baby via blood from the placenta is reduced.
SAQ 19.2 (tests Learning Outcomes 19.1 and 19.3)
Complete Table 19.3 with the measurements you would expect to find in women classified with the types of hypertension shown in the left-hand column.
| Type | Raised blood pressure | Proteinuria | Symptoms of severity |
|---|---|---|---|
| Gestational hypertension |
|
|
|
| Mild pre-eclampsia |
|
|
|
| Severe pre-eclampsia |
|
|
|
| Superimposed pre-eclampsia |
|
|
|
Answer
The completed version of Table 19.3 appears below.
| Type | Raised blood pressure | Proteinuria | Symptoms of severity |
|---|---|---|---|
| Gestational hypertension | Above 140/90 mmHg | No significant proteinuria | None |
| Mild pre-eclampsia | Between 140/90 and 160/110 mmHg | No significant proteinuria | None |
| Severe pre-eclampsia | Greater than or equal to 160/110 mmHg | With or without significant proteinura (urine dipstick test result greater than or equal to +2) | Headache, blurred vision, epigastric burning pain, decreased urine output, decreased or absent fetal kick |
| Superimposed pre-eclampsia | Higher than before the pregnancy in a known chronic hypertensive woman | Significant or worsening proteinuria | With or without symptoms of severity |
Read the following case study and then answer the questions that follow it.
Case Study 19.1 Zewditu’s story
Zewditu is a 37-year-old primigravida woman who is pregnant with twins. She is very overweight for her height. She was in good health until she reached gestational week 22, when she began to complain of headaches and swollen feet and ankles.
SAQ 19.3 (tests Learning Outcomes 19.1, 19.2, 19.3, 19.4, 19.5 and 19.6)
- a.Does Zewditu have any of the common risk factors for hypertension? If yes, what are they?
- b.Does she have any of the clinical features of hypertension? If yes, what are they and what is the underlying cause?
- c.What complications could affect Zewditu’s baby if she has untreated hypertension?
- d.What action should you take in Zewditu’s case and why?
Answer
- a.Zewditu has three of the common risk factors for hypertension: she is having her first baby after the age of 35 years; she is expecting twins; and she is obese.
- b.She has two clinical features of hypertension: headaches and swollen feet/ankles. Both are caused by oedema (swelling due to fluid collecting in the tissues). The headaches are due to oedema around the brain, and the swollen feet and ankles are due to oedema in the tissues of the lower limbs. The underlying cause of the oedema is because the high blood pressure is pushing fluid from the blood out through the vessel walls and into the surrounding tissues.
- c.The complications that could affect Zeditu’s baby if she is not treated quickly are: placental abruption, intrauterine asphyxia, intrauterine growth restriction, intrauterine fetal death, or mental retardation in later life.
- d.The first action is to measure her blood pressure and test her urine for the presence of protein. Even if the results are close to normal, she should be referred without any intervention from you to a higher health facility for further assessment, preferably on the day of the assessment. This is because even if her hypertension is currently mild, it may progress to severe pre-eclampsia in a very short period of time.