Use 'Print preview' to check the number of pages and printer settings.
Print functionality varies between browsers.
Printable page generated Sunday, 26 April 2026, 10:36 AM
Duty of care
Introduction
Welcome to Section 4 of the Introducing practical healthcare course where you will be introduced to the duty of care you are responsible for as a healthcare assistant. When completed you will have the opportunity to obtain a ‘Duty of care’ SPN badge. This section will take approximately 2.5 hours to complete.
In this section, you will consider your duty of care and legislation, including situations at work that should be reported. You will look into how, as a healthcare assistant, you always need to be accountable for your actions. This section will also consider the concept of whistleblowing, or knowing what action to take if you become aware of poor practice in your workplace.
Another aspect of your role as a healthcare assistant might be to deal with comments and complaints from patients. You will find out how to handle incidents, errors and near misses, and how you would normally go about reporting these within your role. It is important to maintain equality and diversity, and to understand inclusion and stereotypes. You will learn about the differences between these terms within this section.
Learning outcomes
By completing this section and the associated quiz, you will be able to:
report any concerns or worries you may have about what happens in your workplace
demonstrate your understanding of equality and diversity.
1 Duty of care
Caring for patients brings with it important legal responsibilities, called your ‘duty of care’. This means promoting wellbeing and making sure that all those receiving care and support in your workplace are kept safe from harm, abuse and injury. Under duty of care you must report any concerns or worries you may have about what happens in your workplace, and there are effective and responsible ways in which individual members of staff or staff groups can – and should – challenge unsafe practices.
These might be:
- poor or unsafe working conditions
- equipment that isn’t working or is missing
- not having the right training for the job
- abuse of patients or staff
- substance misuse (alcohol or drugs)
- food storage, cooking or handling
- violence or bullying.
Remember, duty of care and public interest are not issues you can opt out of. If you believe that safe practice is at risk then you must highlight your concerns with the appropriate manager (you will look at this in more depth in Section 4.3 Whistleblowing).
2 Accountability
As a healthcare assistant you are responsible for the quality of your work and the decisions that you make. Being accountable means that you have to take responsibility for the consequences of your actions and behaviour at all times, even when you are very junior and new to a job. If your actions lead to poor-quality or unsafe care you can be held to account or even disciplined.
You should be careful not to undertake any care which you are not able to do, or for which you have not yet received the specific training. You should only carry out tasks for which you have knowledge and skill (that is, that you are competent to do). You must recognise and acknowledge the limits of your abilities, and if you are asked to do anything that you are not able to do you should tell your supervisor straight away. These are important points and are embedded in the Code of Conduct for healthcare workers in England, along with making sure you can answer for your actions or omissions (Skills for Care/Skills for Health, 2013). The following points on being accountable (from Section 1 of the Code of Conduct) are relevant to the healthcare assistant role.
You must:
- be honest with yourself and others about what you can do, recognise your abilities and the limitations of your competence, and only carry out or delegate those tasks agreed in your job description and for which you are competent
- be able to justify and be accountable for your actions or your omissions – what you fail to do
- always ask your supervisor or employer for guidance if you do not feel able or adequately prepared to carry out any aspect of your work, or if you are unsure how to effectively deliver a task
- tell your supervisor or employer about any issues that might affect your ability to do your job competently and safely. If you do not feel competent to carry out an activity, you must report this
- comply with your employer’s agreed ways of working.
3 Whistleblowing
If you think there may be some form of wrongdoing or misconduct in your workplace, you need to raise your concerns about it: this is known as whistleblowing, or ‘raising concerns’ in the NHS. Under the Public Interest Disclosure Act (1998) workers have a right to ‘blow the whistle’ if management instructions are conflicting with their duty to act in the public interest.
Examples might include where you believe that healthcare practices or equipment are dangerously unsafe; where there is abuse of patients or staff; substance misuse (alcohol or drugs); violence or bullying; or there has been serious misuse of funds or resources (for example fraud or waste).
Next, Gail will describe her understanding of whistleblowing and how it might arise for a healthcare assistant working in a hospital setting.
Transcript: Whistleblowing
Every employer should have a whistleblowing procedure in place to facilitate the disclosure of this kind of sensitive information, which may be along the lines of the following process issued by the UNISON union:
Steps to raising a concern:
- know how to raise a concern
- find out who is affected
- gather evidence
- put your concerns in writing
- specify what outcome you are seeking
- ask for a written response
- seek trade union support if necessary
If you are concerned about something and thinking of talking to someone about it, get support: this could be from your trade union, the appropriate person in your workplace or a ‘whistleblowing guardian’.
The following statements have been taken from healthcare assistants who are thinking about raising an issue within their workplace. While reading them, think about what you might do in each situation.
Activity 1
Health Education England have published a video on raising concerns in healthcare. Watch the video now and try to place yourself in the shoes of the people who had to report wrongdoing. Would you have the courage to report failures in the system where you work?
Transcript: Raising concerns: speaking up about patient safety
[MUSIC PLAYING]
[BEEPING]
[MUSIC PLAYING]
The film you have just seen was made with the purpose of supporting healthcare professionals at all levels, ensuring they feel empowered to both raise and respond to concerns. In it you saw a range of scenarios that you could encounter where patient safety may be put at risk. Challenging behaviours or seeking advice may not always be easy, but it is important that you know who you would speak to in order to raise your concerns. The film also signposts to regulatory bodies, unions and independent advice websites where you can find more information on speaking out.
4 Handling comments and complaints
All healthcare organisations will have a procedure in place to collect and monitor patients’ complaints. Formal complaints will provide valuable feedback and evidence to your managers and employers regarding any problems with the quality and delivery of care and give them important information to help improve services. There may be times when it is helpful to remind a frustrated patient or relative about their right to make a complaint, as this means that the problem is formally noted. If a patient complains about their care or support to you, it is important that it is followed up quickly and in a positive way. As Skills for Care (2015d) advises, patients should be told that their concern or complaint will be taken seriously and that they will be kept involved in the process and informed as much as they would like to be. In a person-centred way, reassure them that they will receive help and support and explain that they can also have an advocate to work on their behalf if they wish in taking action on their behalf.
5 Dealing with incidents, errors and near misses
Patients should always be protected from harm, but mistakes do occasionally happen through things like lack of knowledge, poor communication or sharing of information, stress, failure to take proper care (negligence) or being distracted. They may be:
- incidents or adverse events due to actions (or lack of actions) that have led to unexpected harm which should have been preventable
- errors or doing something in the wrong way
- or near misses whereby a situation which could have harmed an individual was avoided by chance or purpose.
Any of these could occur in your workplace and it’s really important that you recognise when such an incident occurs and know what action to take. In the next audio clip Gail talks about possible incidents that could occur in healthcare settings.
Transcript: Reporting of incidents in the workplace
Like Gail, your workplace will have a form which you should complete to record the facts of the incident, accident or near miss. Doing this will help to reduce the same mistakes recurring in the future. You should complete the form as soon as possible after the event and make your manager aware straight away. (Skills for Care 2015e)
6 Equality and diversity
As a healthcare assistant, you will need to be aware of and understand issues of equality and diversity, and how negative attitudes such as stereotyping and discrimination lead people to perceive individuals or groups as being different. Discrimination can arise from both personal attitudes and behaviours, but also in the way services are organised and delivered. For example, a care plan that is only written in English in small font is an organisational arrangement that excludes those who cannot read, do not read English or have poor eyesight.
Equality and inclusion are basic human rights, and equality is about making sure that everyone is given equal opportunity according to their needs. This might mean giving information in different formats (for example Braille for a blind person) or making sure there is access to a building for an individual in a wheelchair. The consequences of discrimination, especially in older age, can be wide-ranging. Long-term discrimination can lead to poor physical and mental health provision, to inequity in access to services, and to low self-esteem and frustration.
Activity 2
Now you will watch a video which explains the definitions of equality, diversity, prejudice and discrimination – which can be direct or indirect – and makes the point that a fair society is an equal and diverse one.
When you have watched it, write down some examples of stereotyping and prejudice, and think of an alternative response. Think about how to avoid these behaviours occurring in your workplace. Consider your own attitudes and those of your colleagues, and the patients you are caring for. Have you overheard prejudiced statements? Have you challenged them?
Transcript: Equality, diversity, prejudice and discrimination
What is equality and diversity?
Equality and diversity – what does it mean?
Equality is ensuring individuals or groups are treated fairly in order to promote an equal society.
Everyone should have an equal opportunity regardless of their race, gender, disability, religion, age, or sexual orientation.
Everyone should have an equal opportunity regardless of their race, gender, disability, religion, age, sexual orientation.
Equality is not about being politically correct or telling people what they can and can’t say, it’s about treating others how you would want to be treated.
Diversity is about recognising individual as well as group differences and placing a positive value on diversity.
Diversity is about recognising individual as well as group differences and placing a positive value on diversity.
Diversity is everything that is different about everybody.
Different Individuals Valuing Each Other Regardless of Skin, Intellect, Talent or Years.
Diversity is any and all aspects of difference whether these are visible or invisible.
The aim of diversity is to enrich the organisational culture and the working environment.
Diversity is a set of conscious practices that is more than just acknowledging or tolerating difference.
Prejudice and discrimination:
Prejudice broadly describes negative feelings and attitudes people have about others that have no rational basis.
Discrimination generally describes actions people take on the basis of their prejudices.
Discrimination is illegal and can come in the form of Direct and Indirect.
Direct discrimination is when you treat someone less favourably than others because of their group, for example;
Refusing to employ someone solely because of their disability.
Indirect discrimination is when you put a rule or arrangement in place that apply to everyone, but put some people in an unfair disadvantage.
For example: specifying that employees must not wear anything on their heads – this may discriminate against someone with religious beliefs.
All this works towards building a society where no one Is held back because of who they are or where they come from.
And please remember a fair society is an equal and diverse one.
Comment
Were you able to think of some examples and responses? It may be that racism (for example) can be difficult to talk about in your team, and that you wouldn’t feel confident to challenge prejudice, but if staff feel unable to talk about stereotyping and prejudice, they will not be able to challenge it when it is directed against patients. The key to avoiding stereotyping and prejudice in the workplace is to have a flexible and open workplace culture. This openness and honesty will make it easier for care workers to share their concerns and find solutions to racist behaviour. Remember that one of the 6 C’s is courage, and be courageous in challenging or confrontational situations that you know are not right and that do not promote the wellbeing of all individuals, and always respect diversity by providing person-centred care.
Stereotyping and prejudice can lead to discrimination, which can result in inappropriate and poor-quality care, and should always be challenged.
7 Safeguarding
7.1 Safeguarding adults
Safeguarding is about protecting people from harm and abuse, and everyone involved in the safeguarding process needs to be clear about their roles and responsibilities. You are responsible for safe practice at all times and for protecting people from harm and abuse, and your actions should not cause harm or abuse to patients. Training in safeguarding adults should be provided by your employer, so that you are aware of your workplace’s safeguarding policies and procedures and are clear about what you should do if you suspect abuse (or if abuse is disclosed to you). You should be aware of the different types of abuse and able to recognise the signs. These are not always easy to see as abuse is often subtle and hidden.
7.2 Safeguarding children
Wherever you work, and even if your role is only with adults, you need to have a basic understanding and awareness of safeguarding children. A visiting family might raise your concern and you need to know what action to take. In other words ῾child protection and safeguarding is everyone’s responsibility: it is not only childcare workers that have a duty to promote the welfare of children and protect them from harm᾿ (Skills for Care, 2015c).
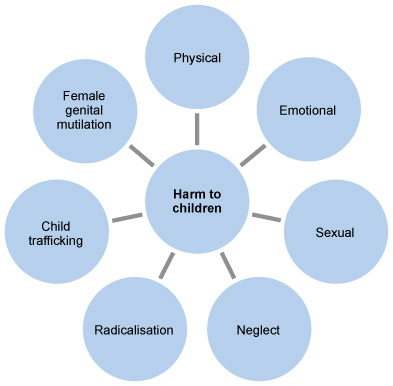
The following diagram outlines the types of abuse and neglect to look out for:
As with safeguarding adults, you should be aware of your workplace’s child protection policies and procedures, and be clear about what you should do if you suspect a child is being or has been abused. You must understand what action to take if you suspect child abuse or neglect is taking place, including who you should report to in the first instance. As a healthcare assistant it is likely that your policy will say you should speak first to your line manager.
Activity 3
If you are currently working with adults or children, find out where your workplace safeguarding policies are kept, and make sure you know what actions you should take if you are concerned about an adult or child’s safety.
If you are not yet working in such a role, do a search on the internet for safeguarding policies. Many organisations’ policies are available there to view.
What you have learned in Section 4
- Caring for patients brings important legal responsibilities, called your ‘duty of care’.
- Being accountable means that you have to take responsibility for the consequences of your actions and behaviour.
- You have a responsibility to report your concerns.
- If a patient complains about their care or support it is important that it is followed up quickly and in a positive way.
- Incidents, accidents and near misses in the workplace must be recorded.
- It is important for healthcare workers to recognise people’s cultural, religious and other preferences, but equally important that they try to avoid making assumptions based on stereotypes rather than knowledge of the individual.
- Safeguarding adults and children is everyone’s business.
Section 4 quiz
Well done, you have now reached the end of Section 4 of the Introducing practical healthcare, and it is time to attempt the assessment questions. This is designed to be a fun activity to help consolidate your learning.
There are only five questions, and if you get at least four correct answers you will be able to download your badge for the ‘Duty of care’ section (plus you get more than one try!).
- I would like to try the Section 4 quiz to get my badge.
If you are studying this course using one of the alternative formats, please note that you will need to go online to take this quiz.
I’ve finished this section. What next?
You can now choose to move on to Taking my learning further where you can reflect on what you have learned, obtain your Statement of Participation for the course and find suggestions of other places you might like to visit.
If you have not done so already, you might like to visit one of the other sections so you can continue collecting your badges.
We would love to know what you thought of the course and how you plan to use what you have learned. Your feedback is anonymous and will help us to improve our offer.
- Take our Open University end-of-course survey.
References
Acknowledgements
This free course was written by Joanne Thomas (consultant for the Open University) and Emma Lipscombe (Learning and Workforce Development Officer for UNISON), with contributions from Ruth Beretta (staff tutor for the Open University).
Except for third party materials and otherwise stated (see terms and conditions), this content is made available under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 Licence.
The material acknowledged below is Proprietary and used under licence (not subject to Creative Commons Licence). Grateful acknowledgement is made to the following sources for permission to reproduce material in this free course:
Every effort has been made to contact copyright owners. If any have been inadvertently overlooked, the publishers will be pleased to make the necessary arrangements at the first opportunity.
Figures
Figure 1: © The Open University
Figure 2: adapted from from Skills for Care (2015) Workbook 11, Safeguarding Children © The Open University
Audios
‘Whistleblowing’ including transcript: courtesy Unison (https://www.unison.org.uk/)
‘Reporting of incidents in the workplace’ including transcript: courtesy Unison (https://www.unison.org.uk/)
Videos
Video ‘Raising concerns: speaking up about patient safety’ including transcript: NHS Health Education, England (https://hee.nhs.uk/ http://www.nationalarchives.gov.uk/ doc/ open-government-licence/ version/ 3/)
Video ‘Equality, diversity, prejudice and discrimination’ transcript only: © http://www.xrtraining.com/