Imaging in medicine
Use 'Print preview' to check the number of pages and printer settings.
Print functionality varies between browsers.
Printable page generated Friday, 26 April 2024, 7:16 PM
Imaging in medicine
Introduction
This course is about the scientific basis of medical imaging. Imaging techniques have long been part of the physician's diagnostic repertoire. Their use has been developed from simple X-ray measurements in the Accident and Emergency Unit to a range of subtle investigations of both the structure and functional status of targeted organs, including the brain. Medical imaging is at the heart of contemporary medical practice.
This OpenLearn course provides a sample of postgraduate study in Science.
Learning outcomes
By the end of this free course you should be able to:
explain the underlying scientific principles of the major medical imaging techniques
explain the mode of operation of the major medical imaging techniques
understand the advantages and disadvantages of the major imaging techniques.
1 Current imaging techniques
A grainy Polaroid of the child in a mother's womb – an X-ray of a tibia fractured in a traffic accident – a report on a brain scan anxiously awaited. Very few of us have not had some connection with the techniques and practices of medical imaging. Often, these contacts are in periods of personal drama in which the medical images chart our physical status, the management of a condition and, in some cases, our future.
Imaging is a central feature of contemporary medicine. Along with chemically based techniques of analysis, it provides the clinician with ways of extending investigations that go beyond external observation and interview.
The video clip below will introduce the major imaging modalities in current use in hospitals. These are:
X-rays, including computed tomography (CT)
ultrasound
magnetic resonance imaging (MRI)
radionuclide imaging
The view offered in the clip is that of the underlying science, from the physical scientist's perspective, rather than that of the medical clinician.
Activity 1
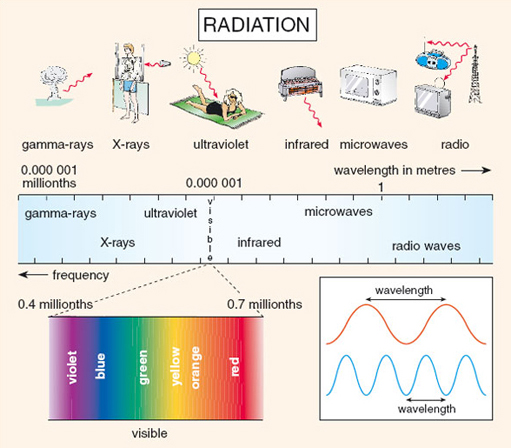
As you watch the video clip, keep in mind the electro-magnetic spectrum shown in Figure 1 below and try to place the electromagnetic energy of each modality on the spectrum.
Click to view the introduction clip presented by Liz Parvin [7 minutes 50 seconds]
Transcript: Introduction clip presented by Liz Parvin
Answer
X-rays and CT use X-ray part of the electromagnetic spectrum.
Medical ultrasound uses sound waves rather than electromagnetic radiation. The frequency of the sound waves is usually between 1 and 15MHz.
Magnetic resonance images uses radio waves (usually around 50–150MHz).
Radionuclide imaging (not actually shown in the video clip, but mentioned by Alan Davis) uses gamma radiation.
2 X-ray imaging
2.1 Introduction
X-ray imaging is probably the best known and most widely used of the imaging techniques we will cover. Not only are X-rays the longest established means of producing images of the internal structure of the body, but X-ray imaging is also the workhorse technique for all radiology departments.
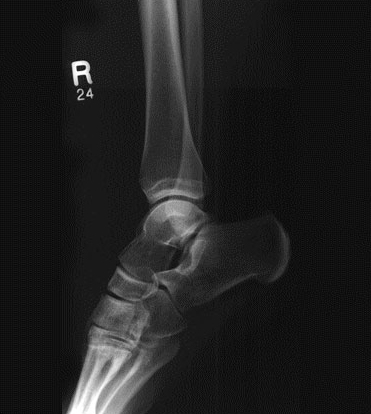
Figure 2
X-rays are high-energy electromagnetic radiation; those used for diagnostic imaging typically have photon energies between 20 and 120 keV.
In X-ray imaging, a beam of X-rays is passed through the patient and detected on the opposite side. As the X-rays pass through the body some are either absorbed or scattered. This attenuation depends on the thickness of the material and on its attenuation coefficient. The equation that describes the reduction in intensity is
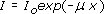
where I0 and I are the intensity before and after passing through material of thickness x and μ is the attenuation coefficient.
Bone has a much higher attenuation coefficient than soft tissue, which in turn has a higher coefficient than air. This means that, if a patient is placed in a uniform beam of X-rays, radiation that has passed through soft tissue will have a higher intensity at the detector than radiation that has passed through bone. Hence the image will show good contrast between bone and soft tissue and, similarly, between soft tissue and lungs. X-ray images usually show the high attenuation material (e.g. bone) as white and the low attenuation material as black.
Watch the video clip below which shows Alan having X-rays of his skull taken by a radiographer, following his arrival by ambulance to the Accident and Emergency Department with a possible head injury and skull fracture.
Click to view the clip about planar x-ray images [2 minutes 45 seconds]
Transcript: Planar x-ray images
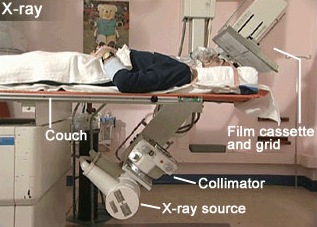
Figure 3 shows the X-ray unit used to image Alan's skull. It's main components – the x-ray source, collimator, patient couch, and film and cassette holder – are labelled.
2.2 Components of an X-ray unit
2.2.1 X-ray source
X-rays are produced when energetic electrons strike a metal target. The X-ray source consists of an evacuated tube containing a cathode, from which the electrons are emitted, and an anode, which supports the target material where the X-rays are produced. Only about 1 per cent of the energy used is emitted as X-rays – the remainder is dissipated as heat in the anode. In most systems the anode is rotated so that the electrons strike only a small portion at any one time and the rest of the anode can cool. The X-rays are emitted from the tube via a radio-translucent exit window.
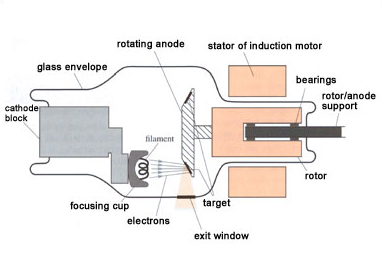
Figure 4
Some of the X-rays are given off at an energy that depends on the nature of the target material. These are known as characteristic radiation (see Figure 5). There is also a broad spectrum of radiation known as bremsstrahlung (braking radiation); it is this radiation that is used in most diagnostic procedures (see Figure 5). However, both types contribute to the radiation dose given to the patient.
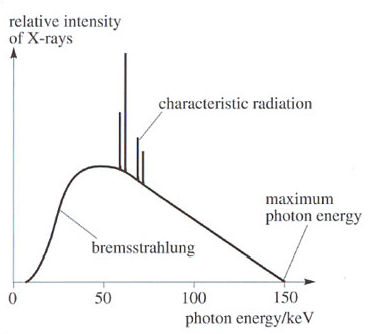
The maximum photon energy is determined by the voltage applied to the tube (known as kVp). The peak of the X-ray spectrum is at about half of this energy. kVp values vary between about 20 kV for very thin body parts and 120 kV for a pelvic X-ray. Filters can be placed in front of the exit window to eliminate low-energy X-rays that do not contribute to the final image.
2.2.2 Collimator
The dimensions of the emerging X-ray beam can be altered by the collimator. This helps to ensure that only the region of interest is exposed to the X-rays.
2.2.3 Couch
The couch or patient trolley must be radio-translucent (i.e. it allows through most of the X-rays). Nonetheless there is some interaction between the couch and the X-rays and this can be a cause of scattered radiation.
2.2.4 Film cassette and grid
As the X-rays pass through the patient some of them will be scattered and will therefore not follow the expected line through the patient. If these reach the detector they will blur the image. Some of the scattered radiation can be removed by a grid, usually oscillating, placed between the patient and the detector.
Analogue imaging systems use either film alone (rarely) or a combination of a film and fluorescent material (phosphor). The phosphor fluoresces and produces visible light which is recorded by the film. The film is then developed.
Digital imaging systems use a variety of methods to record the intensity for each pixel in the image. This can then be displayed on a VDU or printed out on film.
Activity 2
See if you can answer the following questions. Please think about your answer before clicking to reveal the answer.
What happens to most of the electrons which strike the anode in the X-ray source, and approximately what percentage of electrons produce X-rays?
Answer
Most of the electrons produce heat, only 1 per cent of the electrons produce X-rays.
Activity 3
Why is a grid place in front of the film?
Answer
The grid reduces the amount of scattered X-rays which reach the film, thus producing a clearer or sharper image.
Activity 4
Can you think of some advantages and disadvantages of X-ray imaging?
Answer
The advantages of X-ray imaging are:
X-ray images are relatively cheap to produce;
images can be acquired quickly and are particularly useful for a rapid initial assessment;
X-ray images are readily accessible.
The disadvantages are:
ionizing radiation dose;
2-D image of a 3-D object;
contrast can be poor.
The disadvantage of planar X-ray imaging, producing a two dimensional representation of a three dimensional object, is overcome by computed tomography (CT) imaging.
3 Computed tomography
The aim of computed tomography (CT) is to produce an image of a slice of the body. (The Greek word ‘tomos’ means slice.) This is achieved by rotating a thin, fan-shaped beam of X-rays around the patient and measuring the intensity on the opposite side of the patient with a very large number of detectors.
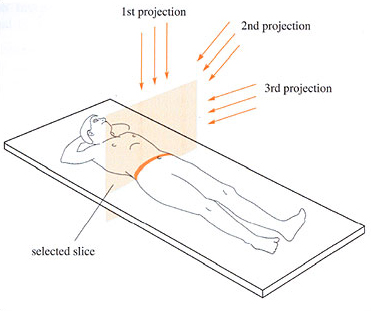
Figure 6
The following video clip shows Alan having a CT scan of his head to see if he has a base of skull fracture. Listen and watch the video clip carefully, with the following questions in mind:
Activity 5
What are the main differences between the skull X-rays and CT images produced of Alan?
What colour do the skull bone and brain tissue appear on the CT images and why?
How does the video say a two dimensional ‘slice’ is produced through the body?
Click to view the clip about computed tomography [2 minutes 47 seconds]
Transcript: Computed Tomography (CT)
Answer
The skull X-rays showed ‘projections’ of Alan's skull (a 3D object represented in 2D) and the brain tissue could not be seen. The CT slices show the skull and internal brain tissue as a series of ‘slices’, and therefore, in much more detail.
The skull bone appears white and the brain tissue grey. This is because the skull attenuates X-rays to a greater extent than the brain tissue, and just like a planar X-ray the more a tissue attenuates X-rays, the whiter it will appear in the final image.
The X-ray source is rotated around the patient and the intensity recorded on the opposite side of the patient. Using data from a large number of angles a computer reconstruction can produce a two-dimensional map of the tissues in a slice of the body.
Let's look at the answer to the final question in more detail. First we will consider exactly how the X-ray source rotates around the patient.
In modern scanners the source and the detectors rotate around the patient at more than one revolution per second. In the older scanners the couch was moved after one rotation and the subsequent rotation had to be in the opposite direction to avoid twisting the cables (called ‘stop and go’ by Dr Klaus Klingenbeck in the following video clip). However, with the introduction of slip-rings it became possible to keep the source and detectors rotating continuously and to move the couch at the same time. This means that the X-ray source describes a helix around the patient and a set of data covering the complete volume of the patient can be collected. This is known as spiral (or helical) scanning and has the advantage that the data for the entire thorax or other section of the body can be collected in one breath hold. More recently, multislice scanners, in which there is more than one arc of detectors, allow even faster data collection.
Click to view part 1 of the clip about X-rays and CT [2 minutes 1 second]
Transcript: X-rays and CT - part 1
Now let's consider how a ‘slice’ through the patient can be reconstructed by the transmission data obtained at a large number of different angles, using a technique called ‘filtered back projection’. The following video clip will look at the transmission data from simple objects and how back projection, and finally filtered back projection, are used to reconstruct the original object from the transmission data. This clip introduces some complex topics – you only need a general overview of how CT image reconstructions work.
Click to view part 2 of the clip about X-rays and CT [8 minutes 36 seconds]
Transcript: X-rays and CT - part 2
Activity 6
Now that you understand more about the CT imaging equipment and the images it produces, take a little time to consider what you think the advantages and disadvantages of this technique would be.
Answer
The advantages of CT imaging are:
excellent resolution and contrast;
choice of tomographic or 3D-images available;
relatively fast (compared with MRI);
contrast medium can be used.
The disadvantages are:
larger dose of ionizing radiation than most planar X-ray procedures;
equipment is costly and therefore not available at all hospitals;
slower and more complex to undertake than most planar X-ray procedures.
4 Magnetic resonance imaging
Magnetic resonance imaging (MRI) is one of the newest techniques available for imaging in hospitals. It is a tomographic technique (i.e. it takes ‘slices’ through the body) based on the phenomenon of nuclear magnetic resonance (NMR). Technically it is a complex technique, but some understanding can be gained using qualitative arguments.
X-rays are not used, but instead the patient is placed in a ‘strong’ magnetic field (around 30 000 times as strong as the Earth's magnetic field). The nuclei of hydrogen atoms (protons) like many other nuclei have a special property called nuclear spin. This means that in some respects they behave like tiny bar magnets, and in a static magnetic field they have just two possible orientations; either aligned with, or against, the magnetic field (see Figures 7 and 8 below). More protons align with the magnetic field, as this requires less energy. So, within the patient the net magnetisation within the tissues is aligned parallel to the applied magnetic field.

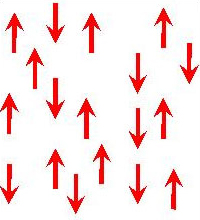
Figure 8
Transitions away from this parallel state can be brought about by the application of a radiofrequency (rf) field, typically in the region of 20 to 100 MHz for many MRI scanners. The frequency required, which is referred to as the resonant or Larmor frequency, depends linearly on the strength of the static magnetic field. The rf field is applied in the form of a pulse of short (microseconds) duration. The signal detected by the scanner is the component of the net magnetisation vector perpendicular to the applied magnetic field.
The signals are detected using specially designed and shaped radiofrequency coils (or antena), for example for heads, knees, etc. The fact that these coils can be placed immediately adjacent to an area of interest makes an important contribution to the quality of the final image.
In the following video clip a head coil is used. As you are watching the video, pay particular attention to the main differences in image appearance between MRI and CT.
Click to view the clip about magnetic resonance imaging [3 minutes 24 seconds]
Transcript: Magnetic Resonance Imaging (MRI)
Activity 7
Take a moment to consider what you think are the main difference between MRI and CT images.
Answer
MRI can be used to ‘slice’ the body in any direction. As well as producing ‘axial’ images, it can also produce sagittal or coronal images (or any plane in between.) The contrast can be changed in MRI images producing what were called T1, T2, or proton density weighted images. The contrast in CT images is fixed, depending on the attenuation coefficient.
We will now look at T1, T2 and proton density weighting in a bit more detail. Once the net magnetisation has been excited away from its position parallel with the magnetic field by the rf pulse, it moves or ‘relaxes’ back to its original state. The times taken for this relaxation are governed by T1 and T2 time constants. These T1 and T2 values vary for different types of tissue.
MR images are formed using a series of rf pulses in a carefully timed sequence. By varying the timings of these pulse sequences the final images can highlight the differences in T1 or T2. (It is also possible to set the timing within a pulse sequence so that the contrast is independent of both T1 and T2, and so depends on just proton density.)
T1-weighted images show tissues with a large value of T1 (e.g. water) as dark. In T2-weighted images tissues with a large value of T2 are bright. Water has a high T2 so shows up bright in a T2 image. This feature can be used to highlight disease. Figures 9 and 10, below, show T2- and T1-weighted MR images.
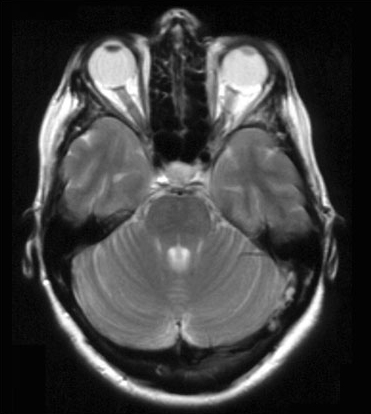
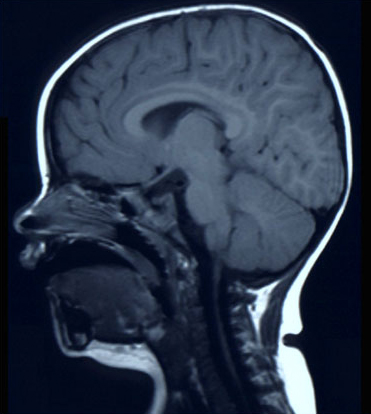
Activity 8
You may think that since MRI uses strong magnetic fields and rf waves, rather than X-rays, it is completely safe. Actually, two safety hazards were mentioned in the video clip. Can you remember what they were?
Answer
MRI scanners, magnetic fields and rf pulses can upset the operations of pacemakers. In addition, heating can occur in some metallic implants.
Another major hazard of MRI scanners not mentioned in the video is the ‘projectile effect’. Ferromagnetic materials experience strong forces in the static magnetic field and objects such as a bunch of keys or an oxygen cylinder can become lethal weapons.
The strength of the magnetic fields and the power levels for the radiofrequency irradiation are thought to be well below potentially damaging levels. However, as a precaution, MRI is not normally carried out during pregnancy.
Activity 9
Now that you understand more about MRI, take a little time to consider what you think the advantages and disadvantages of this technique would be.
Answer
The advantages of MRI are:
excellent spatial resolution;
excellent soft tissue discrimination (for example, white and grey matter in the brain can be distinguished);
no ionizing radiation;
slices can be taken in any direction.
The disadvantages are:
high cost of equipment and maintenance;
relatively slow;
not suitable for all patients (e.g. those with a heart pacemaker).
5 Ultrasound
Ultrasound imaging uses acoustic waves, rather than ionizing radiation, to form an image. The principle is rather like radar; a pulse of ultrasound (1–15 MHz) is sent out from the transducer and reflected from tissue boundaries. Measurement of the time taken for the pulse to return allows the distance to the reflecting boundary to be calculated.
The important parameter determining the amount of reflection is known as the acoustic impedance (Z) of the tissue and is the product of acoustic velocity and density.
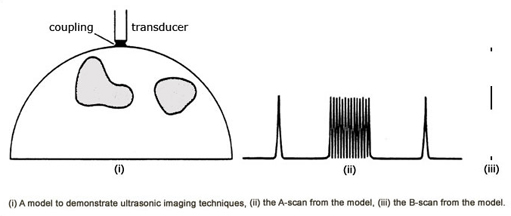
The appearance of the returning echoes can be displayed in two principal ways. Firstly the amplitude of the echo can be shown as a vertical displacement against a horizontal time axis, which takes the appearance of a profile such as that typical of a mountain range. This is known as A (amplitude) mode.
The alternative is to show the echo intensity as dots of varying brightness and this is known as B (brightness) mode. 2D imaging uses a large number of adjacent B-mode lines to form the final image, a B-scan.
In a third mode, called M (movement) mode, a single line of a B-scan is chosen and the position of the reflecting boundaries is plotted as a function of time. A moving boundary will show up as a wavy trace. The shape of this trace can be indicative of critical features such as the operation of cardiac valves.
Activity 10
Look at these ultrasound images of a fetus, and the liver and kidneys. Do you think it was obtained using A-mode, B-mode or M-mode ultrasound imaging?
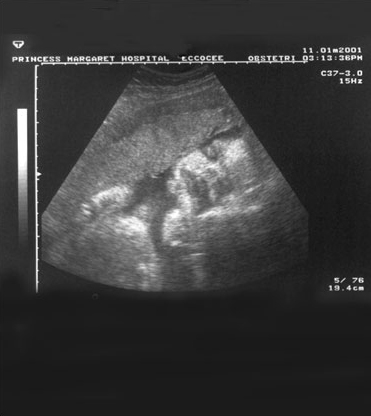
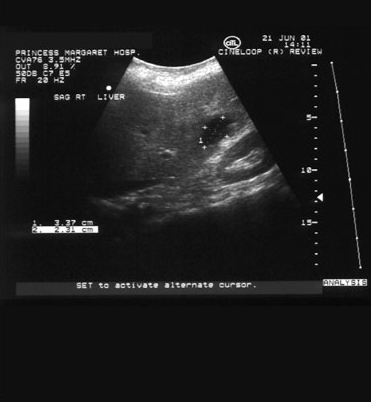
Answer
They are both B-mode images. This is the type of ultrasound image we are all most familiar with.
Activity 11
Watch the following video clip.
Click to view clip about ultrasound [5 minutes 24 seconds]
Transcript: Ultrasound
What advantages of ultrasound imaging are mentioned?
In addition to B-mode imaging, which other forms of ultrasound imaging are shown?
Answer
Ultrasound imaging is quick, cost effective, has virtually no known hazards and is acceptable to most patients.
M-mode, colour flow Doppler and flow velocity/time image.
We will now look in a little more detail at the ultrasound transducer. Design of transducers is complex but they rely on the piezo-electric effect. When a voltage is applied across piezo-electric materials they change shape. If an a.c. voltage is used then the crystal vibrates at the same frequency and sound is produced.
The process also works in reverse – sound incident on the crystal gives rise to an a.c. voltage. Thus the same crystal can be used to transmit and receive.
Each transducer will be designed for use at a particular frequency. In general a higher frequency gives better resolution but lower penetration. So for large patients, or deep structures, the frequency will have to be low – perhaps 3 MHz; for small structures, such as the eye, frequencies can be much higher (e.g. 12 MHz). Some transducers are designed to transmit at one frequency and receive at another, allowing detection of the second harmonic reflections.
Transducers can be designed for use externally or via body orifices such as the vagina (for uterine imaging), or the oesophagus (for heart imaging).
6 Radionuclide imaging
6.1 Introduction
Radionuclide imaging is a very valuable way of examining the function of an organ, as opposed to the more structural images obtained by other methods such as X-ray and CT.
The basic principles of radionuclide imaging are as follows:
a radioactive substance, usually combined with a biologically active compound, is injected into the patient;
this targets a particular organ or tissue type;
the radiation emitted is detected and used to form an image of, or the function of, that organ.
The most common radioactive substances used emit gamma rays (usually in the energy range 100–300 keV). More than 95 per cent of all gamma camera imaging techniques use technetium-99m (Tc-99m). This radionuclide is particularly useful because:
it produces only gamma rays (by isomeric transition);
the gamma rays have an appropriate energy of 140 keV;
the physical half-life of Tc-99m is about 6 hours, so injection and imaging can take place in a reasonable period of time but the patient does not remain radioactive for a long period;
it can readily be combined with biologically active substances to form a variety of radiopharmaceuticals.
Tc-99m is produced by the beta decay of molybdenum-99 by the reaction:
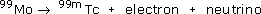
6.2 Producing the radioactive substance (elution)
In the radiopharmacy Tc-99m is produced in a generator.
Mo-99, a product of the fission of uranium, is isolated from a nuclear reactor and absorbed on to an alumina column in the generator. When a saline solution is passed over the column, ion exchange results in the production of sodium pertechnetate. This can then be chemically manipulated to form a variety of compounds. The removal of the technetium by the passage of saline is known as elution.
Conveniently, the optimum interval between elutions is 24 hours. As the half-life of Mo-99 is 66 hours the generator itself can be used for approximately one week. It is then returned to the supplier and replaced with a new one.
Activity 12
Click on the video clip to watch the elution process. Why do you think protective clothing needs to be worn?
Click to view part 1 of the clip about radionuclide imaging [2 minutes 26 seconds]
Transcript: Radionuclide Introduction
Answer
The pharmaceutical will be injected directly into the patient, so it must be produced in completely sterile conditions. The suit and mask are worn to prevent germs from the person reaching the eluate.
6.2.1 Injecting the radioactive substance
The injection may be given immediately before the imaging process, or there may, for certain procedures, be a delay of several hours.
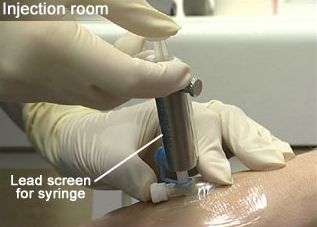
The patient's details and the dose being administered are carefully checked by two people before the injection is given. A lead-screened syringe is used to protect the staff from unnecessary radiation dose (see Figure 14).
6.3 How a gamma camera works
Activity 13
Before we look at a patient being imaged and some of the images which can be obtained using this technique, we will look in a bit more detail at how a gamma camera works. Watch the following video clip and note down the main components of the camera as you watch the clip.
Click to view part 2 of the clip about radionuclide imaging [1 minute 16 seconds]
Transcript: Positron emission tomography (PET)
Answer
The main components of a gamma camera are:
the sodium iodide crystal;
the collimator; and
the photomultiplier tubes.
Figure 15 shows the components of a gamma camera. Further detail on these components can be found below.
6.3.1 Collimator
Without a collimator, gamma rays from all directions would be collected by the crystal and no useful image could be obtained. Gamma rays cannot be focused by a lens but a collimator consisting of a series of holes in a lead plate can be used to select the direction of the rays falling on the crystal. Most collimators in use today are parallel hole collimators. A parallel hole collimator is shown schematically in Figure 16.
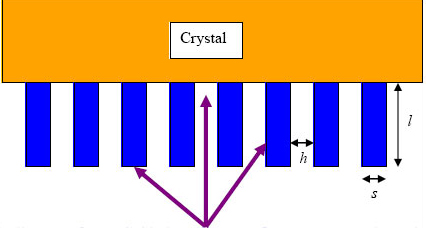
Figure 16
The resolution and sensitivity of a collimator depend on a number of factors including:
hole size (h);
the thickness of the septa (s), the lead between the holes;
the length of the holes (l);
the energy of the gamma rays.
Different collimators are selected for different procedures – e.g. Low Energy High Resolution.
6.3.2 Crystal
Almost all modern gamma cameras use (thallium-doped) sodium iodide (NaI) as the scintillation crystal. A gamma photon interacts with the crystal to produce many photons of visible light.
Sodium iodide is hygroscopic so cannot be left exposed to the air. The front surface is coated with a low atomic number metal that allows the gamma photons to pass through. The rear surface is covered with a transparent coating so that the visible photons can pass through to the photomultiplier tubes.
6.3.3 Photomultiplier tubes and detection circuitry
The visible photons are collected by an array of photomultiplier tubes behind the crystal. These convert each visible photon to an electron and then multiply the number of electrons sufficiently to give a voltage pulse. Because the number of visible photons is proportional to the energy of the incoming gamma ray, the height of the pulse depends on this energy. This gives a method of counting the numbers of gamma photons at different energies that reach the crystal.
A resistive network connected to the photomultiplier tubes gives information on the spatial position (x,y) of each incoming gamma ray. The so-called ‘z coordinate’ corresponds to the pulse height and therefore the energy of the gamma ray.
6.4 Taking the image
Activity 14
Now watch this video clip of a patients lungs being imaged, called a VQ (ventilation quotient) scan. What are the two different types of acquisitions used called? What radioactive substance is used for each acquisition, and why?
Click to view clip about planar scans [2 minutes 21 seconds]
Transcript: Planar scans
Answer
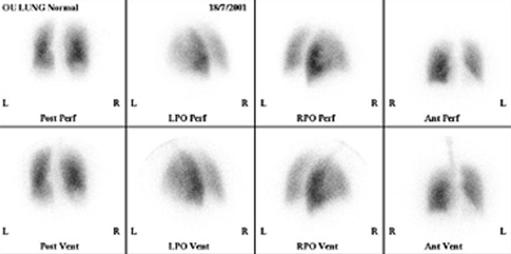
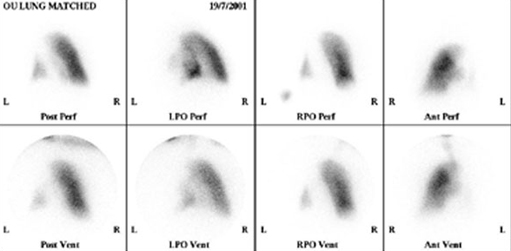
The two different scans mentioned were a perfusion and ventilation scan, to look at the blood supply and air supply to the lungs, respectively. In order to do this simultaneously two different radionuclides that have different gamma ray energies are used. This is a valuable diagnostic test for a pulmonary embolism (a blood clot in the lungs).
To image the perfusion the patient is given an injection of technetium-99m (gamma energy 140 keV, half-life 6 hours) combined with macro-aggregated albumin (MAA). The ‘large’ particles of MAA tend to lodge in the very small capillaries of the lungs and therefore give a good indication of where there is, or is not, a good blood supply.
The ventilation can be imaged by asking the patient to breathe a mixture of air and krypton-81. This is produced from a generator containing the parent radionuclide, rubidium-81. As the patient is breathing the krypton-81, it shows which areas of the lungs the gas reaches, and therefore, which areas are ventilated.
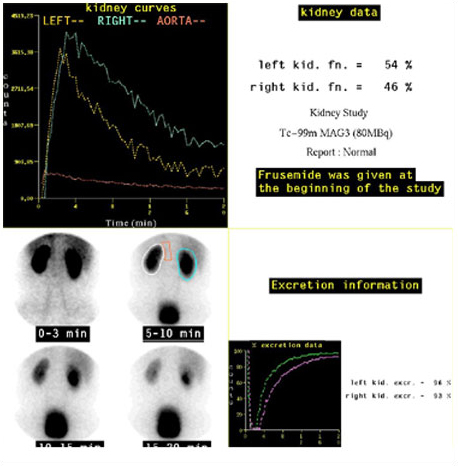
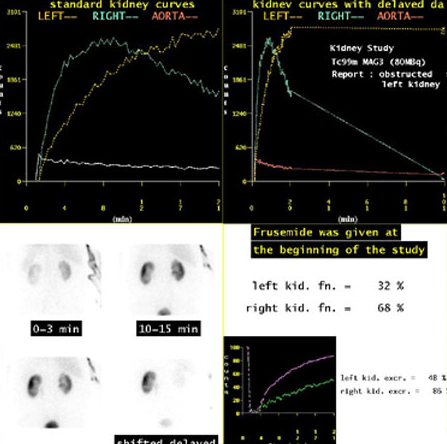
Another widely used procedure is a dynamic renogram. In this case the radionuclide imaged is one that is taken up and excreted by the kidneys. Successive images are collected over a period of time (e.g. every 15 seconds for 20 minutes) and can then be analysed to compare the function of the kidneys.
Activity 15
Now watch this final video clip on radionuclide images, on the single photon emission computed tomography (SPECT) imaging technique. The sequence shows cardiac (heart) images being obtained. How does SPECT produce slices through the body?
Click to view clip about SPECT [3 minutes 23 seconds]
Transcript: SPECT
Answer
Data is collected from a large number of directions by rotating one or more camera heads around the body. Then, tomographic images can be reconstructed, by filtered back projection, using a similar process to CT. The speed of rotation is much slower than that used in CT – the whole process taking at least 10 minutes.
Images of a normally perfused heart muscle (myocardium), and a heart with an inferior and lateral wall defect are shown below.
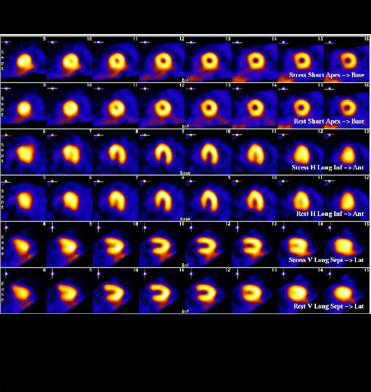
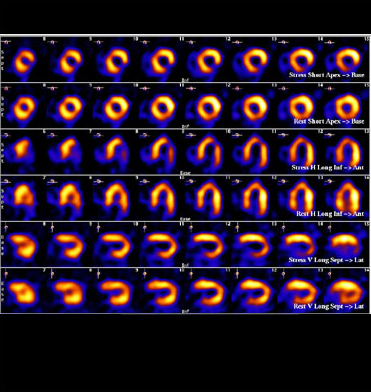
Activity 16
Take a moment to consider what you think the advantages and disadvantages of radionuclide imaging would be compared with ultrasound, MRI, CT and X-rays.
Answer
The advantages of radionuclide scans are:
demonstration of functional information that often cannot be obtained in other ways;
wide variety of organs can be imaged;
tomographic and 3-D images available (SPECT).
The disadvantages are:
poor resolution;
radiation dose to the patient;
slow and labour intensive;
specialised radiopharmacy and scanners are not readily available at all hospitals.
7 Conclusion
Activity 17
Perhaps you are asking yourself why there are so many different imaging modalities. Is there not one that will do everything that is required? The answer, at the moment, is ‘No’. With most of the imaging techniques, we considered their advantages and disadvantages. Watch the following video clip, and note down what items the clinician should be considering when deciding which imaging technique to use.
Click to view concluding clip [2 minutes 14 seconds]
Transcript: Conclusion
Answer
Risk
What are the risks associated with the technique?
Are there particular risks for this patient?
Are there risks for the staff?
Do the benefits of a correct diagnosis outweigh the risks?
Speed
Is a fast initial diagnosis important?
Is the procedure very lengthy, and so not suitable for some patients?
Image quality
Will the image show the required information?
What resolution will be achieved and will it be sufficient?
Does the image show function or structure?
Cost
Is the technique too costly to use for a routine preliminary diagnosis?
We hope that you wish to learn more about the science behind these imaging techniques, and others that were not covered here. To do this you will need to enrol on the S809 Imaging in medicine course.
Acknowledgements
This extract is taken from S809 © 2005 The Open University.
Course image: Liz West in Flickr made available under Creative Commons Attribution 2.0 Licence.
All written material contained within this course originated at the Open University.
Don't miss out:
If reading this text has inspired you to learn more, you may be interested in joining the millions of people who discover our free learning resources and qualifications by visiting The Open University - www.open.edu/ openlearn/ free-courses
Copyright © 2016 The Open University