10.4.3 Secondary prevention: emergency care for a woman in shock
![]() A woman in shock needs help fast. You must treat her quickly to save her life.
A woman in shock needs help fast. You must treat her quickly to save her life.
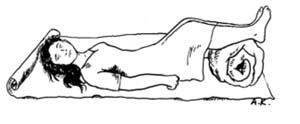
Shock is an inevitable consequence of a ruptured uterus. So you refer her quickly to the nearest health facility with the necessary emergency care services. On the way, have the woman lie with her feet higher than her head, and her head turned to one side (Figure 10.2). Keep her warm and calm.
If you have been trained to do so, begin to give her intravenous fluids. You learned how to do this in the Antenatal Care Module, Study Session 22, and in your practical skills training. If she is conscious, she can drink water or rehydration fluids (oral rehydration salts, ORS). If she is not conscious, do not give her anything by mouth - no medicines, drink or food.
Other important preparations that you should already have put in place are to:
- Ensure that your antenatal advice explained clearly to the woman the importance of having skilled help when she goes into labour
- Persuade the woman’s family and her community to make a plan in advance for possible emergencies, including transport and financial support
- Make sure that you are well versed and skilled in making an early diagnosis and conducting pre-referral emergency procedures
- Make sure the woman goes to the health facility accompanied by at least two fit adult persons who can be potential blood donors, and go with her if you can.
Finally, try to reduce the possibility of any delay, which can mean the difference between life and death. The reasons why so many Ethiopian women die of a ruptured uterus are reluctance to seek skilled help at birth and then delay in seeking medical help following a rupture; further delay in getting treatment because of distance to a health facility; or lack of equipment and appropriately trained personnel when the woman arrives for emergency care.
If you remember all these points you will have the best possible chance of ensuring that the woman is quickly referred to the most appropriate facility for emergency intervention and care.
10.4.2 Primary prevention: getting to a health facility for emergency care before uterine rupture
