If we’re looking for silver linings to the pandemic, we might consider the fact that carers have become visible to the rest of the country in a way that they never were before. Through the pandemic, we have all come to recognise and appreciate the enormous value of carers, both paid and unpaid, and the pressures they face, to the extent of applauding them and other key workers in our millions every week.
Before the pandemic hit, the number of those providing unpaid care for family, friends or neighbours had risen to about 9 million people (1 in 7 of us), saving the UK £132 billion a yearIn contrast to their relative invisibility, the statistics about carers are harder to ignore. Even before the pandemic hit, the number of those providing unpaid care for family, friends or neighbours had risen to about 9 million people (1 in 7 of us), saving the UK £132 billion a year – the cost of a second NHS. Research published during Carers’ Week in June shows that an extra 4.5 million people have been added to that number during the pandemic.
Although we’ve come to appreciate carers more over the last few months, this will count for little in the long run if it does not publicly drive a move to do what we can to ensure that carers receive the best possible support and information, both now and once the pandemic is behind us. The question of how to make sure that this happens is far too big for one short article to answer and needs serious political action. However, one way forward is to use the extensive evidence base about carer support. In other words, start with what has been proven to work.
The National Institute for Health and Care Excellence, or NICE as it is more widely known, produces evidence-based guidance and advice for health, public health and social care practitioners. Unlike the navigation through the scientific uncertainties generated by the new coronavirus infection, NICE guidelines are produced following a very thorough, systematic and painstaking analysis of all available good quality scientific evidence in a given area. The heart of a guideline is a set of practical recommendations agreed by a committee of experts, including people with lived experience, and checked and rechecked with a wide range of people and organisations who will be affected by the eventual product. A NICE guideline is, therefore, about as close as we can get to “following the science” in a considered, rigorous and above all practical manner.
On 22 January 2020, NICE published its guideline on Support for Adult Carers. The timing could mean that it has slipped under the radar for many as the Covid-19 pandemic started to take hold just a few weeks later. The guideline contains 103 recommendations (see https://www.nice.org.uk/guidance/ng150) and is designed to:
“improve the lives of carers by helping health and social care practitioners identify people who are caring for someone and give them the right information and support. It covers carers’ assessments, practical, emotional and social support and training, and support for carers providing end of life care.”
The recommendations can be implemented by anyone working with carers in order to ensure that the support they need is not just delivered but actively enhanced, both during the pandemic and as services adjust to post-pandemic life. Examples are:
Ensuring that all support is underpinned by basic principles such as:
- Ensuring that all support is underpinned by basic principles such as:
- working with carers as expert partners, not just passive recipients of service
- ensuring that carers’ legal rights to information and support are respected
- recognising the diversity of carers
- accompanying written information with personal discussion
- recognising that carers’ needs change over time and providing information and advice that is relevant to their needs at the time.
- Using every opportunity to identify carers. If you don’t know who is a carer to start with, you can’t make sure that they get the information and support to which they are entitled. Many of the services that might be expected to identify who is in this position are temporarily less accessible than they were (e.g. GP surgeries). The guideline can help across people working in the NHS, local authority and third sector apply creativity in thinking how we can find people who may need help. Anybody helping someone recover from Covid-19 in the community could pick up if there’s someone in the household in a caring role.
- Practical recommendations that will help ensure the effectiveness of support services. These include various forms of social and community support for carers which can be adapted for a changed world. For example, although the evidence strongly supports the value of peer support, it has been almost impossible to meet in person during the pandemic and many carers appear understandably nervous about returning to face-to-face support groups even once the lockdown is relaxed. The recommendations are equally applicable to online and socially distanced peer support adaptations that achieve similar outcomes.
- A set of tools to help people put the recommendations into practice. One of these is a “Baseline assessment tool” that gives organisations a framework for identifying:
- which recommendations are most relevant to them
- how their current services measure up to those recommendations
- the risks they run in not following a recommendation, and
- how services might be improved.
This tool provides an important reference point when adapting services, allowing us to move with thought and care to ensure that quality is maintained and that resources are used as effectively as possible. Whether you work or volunteer for an organisation or are a carer yourself, this tool can promote a systematic approach to ensuring that what happens is based on firm evidence of what works.
- An “Into practice guide” accompanies every NICE guideline, summarised in the diagram below.
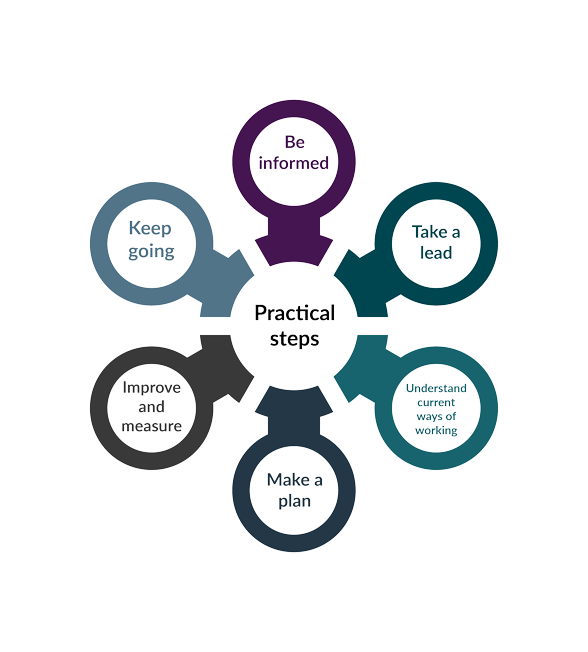
This tool sets out “the most common steps taken when putting evidence-based guidance into practice. You can follow them exactly or take a more flexible approach. Each step has tips and actions to help you get started: pick and choose what suits your project.” Again, this applies equally whether you are adapting services in an emergency or ensuring that they are future-proof.
This work was undertaken by The National Guideline Alliance which received funding from the National Institute for Health and Care Excellence. The views expressed in this publication are those of the authors and not necessarily those of NICE.
Authors: Phil Taverner, Mary Larkin, Jitka Vseteckova, Nichola Kentzer, Jo Horne, Martin Penson, Martin Robb, Alex Berry, Melinda Spencer, Abigail Methley.




Rate and Review
Rate this article
Review this article
Log into OpenLearn to leave reviews and join in the conversation.
Article reviews