4.8 Antigens and the specific recognition of pathogens
Every type of pathogen has at least one (often many more) unique molecules known as antigens in their structure. In addition to the PAMPs (pathogen-associated molecular patterns) shared by many different pathogens, each type of pathogen also has its own unique distinctive antigens. Each individual T cell and B cell (the leukocytes responsible for adaptive immunity) is programmed to recognise just one specific antigen, so it follows that each T or B cell can usually recognise only one type of pathogen, or at most two or three closely related pathogens that have very similar antigens. Recognition of an antigen by these adaptive leukocytes triggers an immune response against only those pathogens with that antigen in their structure. The political slogan ‘One person, one vote’ springs to mind as an analogy for ‘One adaptive leukocyte, one target’!
We haven’t yet answered the question of how T cells and B cells recognise antigens. Each of these leukocytes carries receptor molecules (often abbreviated to ‘receptors’) on its outer cell membrane. Receptors are very large molecules containing hundreds or even thousands of atoms. As a consequence, they fold up into very complex 3D shapes with many troughs, crevices, humps and hollows, creating a molecular landscape that is unique for each receptor molecule.
A particular type of receptor molecule on the surface of a T cell or B cell can only recognise an antigen that has a 3D shape which is the ‘mirror-image’ of this receptor, so the two molecules can fit together like a key in a lock. In fact, the contact area between the receptor and the antigen involves only a tiny part of each molecule (Figure 9), but this is enough to hold them together long enough to trigger changes in the leukocyte.
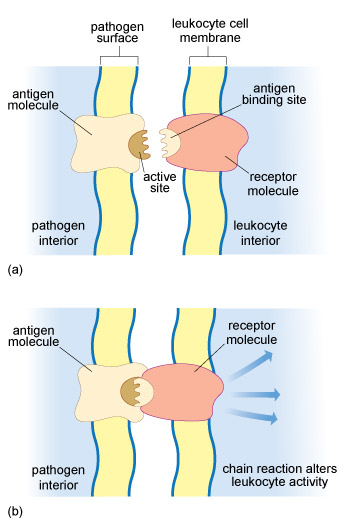
Each T cell and B cell carries many identical copies of a single antigen receptor, so an individual T or B cell can only bind to pathogens that display the corresponding antigen. For example, a T or B cell with receptor molecules that fit an antigen found only in the structure of malaria protists is unable to recognise any other pathogen as a target for an adaptive immune response – it cannot bind to the antigens of (for example) TB bacteria or polio viruses.
At least 10 million different antigen receptors, each with a unique 3D shape, are necessary to recognise all the pathogens an individual may encounter in a lifetime. How this vast array of antigen receptors is generated by T and B cells, each of which carry just one antigen receptor shape, is beyond the scope of this course, but our survival depends on this marvellous phenomenon.
By contrast, the leukocytes responsible for innate immunity have receptor molecules that recognise PAMPs, which many different pathogens have in common. This is why innate leukocytes have a non-specific response to infection – in a sense, all pathogens ‘look alike’ to them, so they are incapable of forming a ‘memory’ of having encountered a pathogen before.
We said earlier that we would explain the different actions of T cells and B cells in the adaptive immune response to infection. We start by considering B cells in the next section, which produce proteins called antibodies.
