5 Coeliac disease
For some people, the symptoms of IBS relate to undiagnosed coeliac disease (pronounced see – lee–ac). It is estimated that 1% of the British population has the condition. Coeliac UK states: ‘only 24% who have the condition have been diagnosed which means there are currently nearly half a million people who have coeliac disease but don’t yet know.’
This increases to a one in ten chance of having this condition if a first-degree family member (such as mother, father, sister or brother) also has the condition.
There are a variety of symptoms which include bloating, diarrhoea, nausea, wind, constipation, tiredness, sudden or unexpected weight loss (but not in all cases), hair loss and anaemia.
So how does coeliac disease differ from IBS?
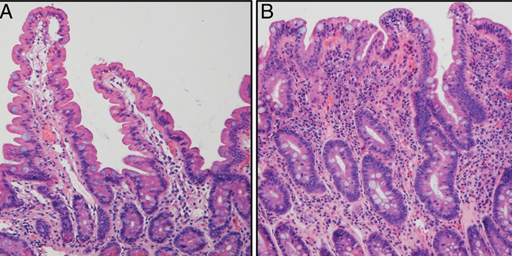
In section 1.5 we looked at the immune response to an allergen. Imagine if that beneficial immune response resulted in the body attacking its own healthy cells. This is what happens with coeliac disease. The allergen is gluten, which sets off an autoimmune response that attacks the villi in the small intestine (Week 2, section 3.1, Figure 10) and flattens them (Figure 9). Autoimmune means the immune response occurs with the body’s own tissues, cells, or cell components.
Activity 4 Consequences of flat villi
Make a list of how flattening the villi could affect what is absorbed from the food we eat. Click ‘Save’ when you are satisfied with what you have written.
Answer
Your list might include:
- the body is unable to absorb all of the nutrients from food properly, causing malabsorption
- water cannot be absorbed, so dehydration occurs
- there may be diarrhoea.
It can be useful to know which part of the digestive system absorbs which nutrients. Do you remember we looked at where the nutrients are absorbed in Week 2, section 3.1?
The lack of surface area means that nutrients may not be absorbed in sufficient amounts. For example, water-soluble vitamins, vitamin B12, bile salts, amino acids and simple peptides, as well as water and sodium. This can cause malnutrition.
In 2015, the National Institute for Health and Care Excellence (NICE) produced guidelines for the recognition, assessment and treatment of coeliac disease.
- A diagnosis of coeliac disease in adults is from a blood test to check for antibodies and a biopsy. (For children, a biopsy is only done if required.) But the person needs to be eating gluten (found in wheat, barley and rye) at the time of the test.
- The only treatment is a gluten-free diet for life.
- Even the smallest amount of gluten can cause an autoimmune reaction.
- There should be an annual review where blood antibodies are checked. Also a DEXA scan which can identify bone density, because bone health is affected with poorly controlled coeliac disease.
As you can see, this condition requires the maintenance of a gluten-free diet. Some essential foods are available on prescription and a team of health professionals is needed to support people who have coeliac disease.
Activity 5 Finding foods that are gluten free
Look in your kitchen cupboards and see which foods have the gluten-free symbol (Figure 10).

As you can see, many foods contain gluten, some of which are obvious, but some you may not realise, because the factory may contaminate products with traces of gluten. Gluten-free is only gluten-free if prepared in gluten-free, non-contaminated areas.
Can you imagine what it must be like following a strict diet such as gluten-free? Well, that is what a person diagnosed with coeliac disease does every day. It is hard even though some basic foods are available on prescription.
You may be able to be careful at home, but what about eating out? Coeliac UK has been working with caterers. If accredited, they can use the symbol developed by Coeliac UK, showing that the restaurant meets the gluten-free standard (Figure 11).

