2.4 Stomach ulcers
Stomach acid is produced by some special cells in the stomach wall. But why doesn’t the acid attack the stomach wall and coagulate the proteins in the cells of the stomach wall?
The answer is that the stomach wall also produces a thick lining of sticky mucus, which generally keeps the acid away. But sometimes this barrier does not work, the acid gets through and an inflamed and sore patch called an ulcer develops in the stomach wall.
Until the mid-twentieth century, it was thought that stress, a poor diet or both caused stomach ulcers. Eating a lot of spicy foods was also considered a possible cause. However, changes in diet and lifestyle rarely made any difference. Then it was suggested that ulcers were caused by excess acid in the stomach. A drug called ranitidine, which blocked acid production, was commonly prescribed. In the 1980s, ranitidine was the world’s number one drug, with several billion pounds being spent on it annually. But it did not cure the problem – as soon as people stopped taking it, the ulcers came back.
But things were changing. In the late 1950s, Dr James Likoudis, working in a small town in Greece, diagnosed himself with an ulcer. He successfully treated himself, and subsequently several of his patients, with a mix of antibiotics. However, his work was not well received by the medical establishment and it was another 30 years before it was widely recognised that he was right. A common bacterium, found in about half of the world’s population, was the primary cause of most stomach ulcers. It doesn’t have a common name but its scientific name is Helicobacter pylori, or H. pylori for short.
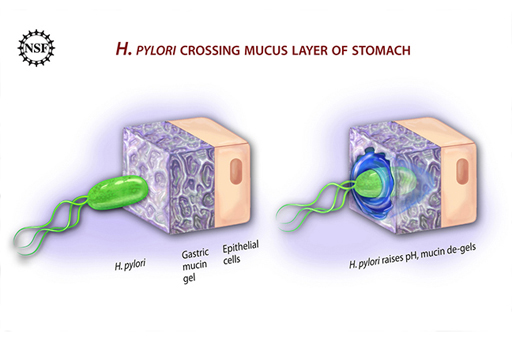
The pioneering work on the role of H. pylori in causing stomach ulcers was done by two Australian scientists, Barry Marshall and Robin Warren in the 1980s. To convince the scientific world of their hypothesis that H. pylori caused stomach ulcers, Marshall deliberately infected himself with a culture of the bacteria. As expected, his stomach became painful and inflamed until he took the right antibiotics. It appears that the bacteria can burrow through the lining of mucus that normally protects the stomach wall from damage. Ultimately, the stomach wall becomes inflamed (Figure 5).
Within a few years, the treatment of stomach ulcers was revolutionised. In 2005, Marshall and Warren were awarded the Nobel Prize in Physiology or Medicine for their discovery of the bacterium Helicobacter pylori and its role in gastritis and peptic ulcer disease.