Who are we?
We are cancer researchers working at The Open University. Our daily job involves identifying and testing new therapies and new diagnostic technologies for cancers. For this reason, we are regularly in contact with cancer charities and patient support groups. In the past few weeks, we have been in conversation with many of them and we have collected a series of cancer-related questions about the new coronavirus. We thought that it would be useful to publish evidence-based answers to these questions, to help cancer patients and their families navigate these unprecedented and challenging times.
What is COVID-19?
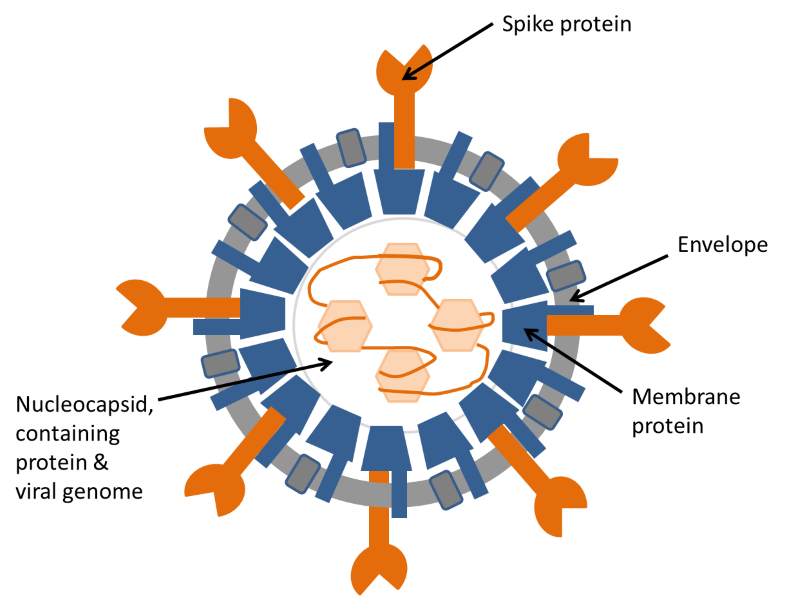
A cluster of pneumonia cases were observed in December 2019 in Wuhan, China. It became rapidly clear that these pneumonia cases were caused by a newly emergent virus. This virus belongs to β – coronaviruses family, a large class of viruses, which mainly infect bats, but can also infect other species, including humans. This newly discovered virus was named SARS-CoV-2 due to its similarities with a previously identified coronavirus (SARS-COV) that caused the outbreak of Severe Acute Respiratory Syndromes (SARS) in the early 2000s (for more information about what a virus is see this article on OpenLearn). SARS-CoV-2 causes the disease COVID-19. Compared with SARS, the new coronavirus SARS-CoV-2 seems to spread more easily within the population, but causes fewer deaths. This is based on evidence conducted in March 2020.
Most COVID-19 cases are thought to lead to asymptomatic, mild or moderate symptoms (fever, cough and fatigue). A small proportion of patients develop severe respiratory symptoms and might need hospitalisation or even assistance with breathing in intensive care units. In the UK, 26,771 people passed away from 687,369 patients that have tested positive for SARS-CoV-2 (numbers correct as of 30 April 2020), which suggest a mortality rate of 15%. Various studies are trying to understand why some patients have more severe symptoms than others. Unfortunately, there is currently no specific treatment for COVID-19; although many vaccines and antiviral drugs are in development or being repurposed, with some already being tested in clinical trials. For clarification, repurposed drugs are medicines that work for another disease but scientists discover they can be useful to treat different conditions. These drugs are very attractive because they have already been demonstrated to be safe for the human body, which helps to speed up the development of the treatment.
According to the Office for National Statistics, 86% of people who died with COVID-19 at the end of March 2020 had a pre-existing health condition. Within this group, certain health conditions have been identified as increasing the risk of developing severe COVID-19 (see this article on protecting extremely vulnerable people from COVID-19).
Are cancer patients at higher risk of becoming severely ill from COVID-19?
To answer this question, we have consulted several reports on COVID-19 epidemiology. Based on 481 patients who have died from COVID-19, the Italian Superior Institute of Health reported several diseases that were more frequently associated with COVID-19-related deaths.
| Underlying condition | Number of patients | Percentage (%) |
| Hypertension | 355 | 73.8 |
| Diabetes mellitus | 163 | 33.9 |
| Cardiovascular ischemia | 145 | 30.1 |
| Atrial fibrillation | 106 | 22 |
| Chronic renal failure | 97 | 20.2 |
| Cancer | 94 | 19.5 |
| Chronic Obstructive Pulmonary Disease | 66 | 13.7 |
| Dementia | 57 | 11.9 |
| Ictus | 54 | 11.2 |
| Chronic liver disease | 18 | 3.7 |
| Case rate fatality | 8,165 deaths from 80,539 cases | 10.1 |
Table 1. Number of COVID-19 patients that died with different underlying health conditions from an Italian study
In fact, 19.5% of patients who died from COVID-19 were cancer patients. This needs to be taken carefully because of the small number of people in the Italian survey. According to an early report from Wuhan cases, there is ~3.5-fold higher risk of experiencing severe effects of COVID-19 (e.g. needing intensive care unit (ICU) admission, mechanical ventilation or death) for patients with cancer when compared with those without cancer (see this article from the American Journal of Clinical Oncology).
Based on Wuhan´s experience, patients who were treated with chemotherapy or have undergone surgery immediately before contracting COVID-19 were at higher risk of developing severe COVID-19 symptoms.As this pandemic develops, more data will become available and this information will help to understand if specific cancer types and/or stages are more associated with severe COVID-19. Hopefully, this information will also help us to understand how to identify high-risk individuals and to prevent severe COVID-19 in cancer patients.
Based on the current evidence, the UK government has identified patients with certain health conditions as “extremely vulnerable”. For this group, the government has suggested “shielding”, which means self-isolating for at least 12 weeks to protect against exposure to SARS-CoV-2 (for Government advice on COVID-19 social distancing see their website).
Some people with cancer can be considered to fall into the vulnerable category based on the type of cancer and/or treatment they are undergoing. Based on Wuhan´s experience, patients who were treated with chemotherapy or have undergone surgery immediately before contracting COVID-19 were at higher risk of developing severe COVID-19 symptoms.
Cancer patients with particularly high risk of suffering severe symptoms of COVID-19 are:
- People with cancer who are undergoing active chemotherapy.
- People with lung cancer who are undergoing high dose radiotherapy.
- People with cancers of the blood or bone marrow such as leukaemia, lymphoma or myeloma who are at any stage of treatment.
- People having immunotherapy or other continuing antibody treatments for cancer.People having other targeted cancer treatments which can affect the immune system, such as protein kinase inhibitors or PARP inhibitors.
- People who have had bone marrow or stem cell transplants in the last 6 months, or who are still taking immunosuppression drugs.
In this series of articles we explore how COVID-19 impacts on cancer patients and their treatment. Read on to explore how COVID-19 affects cancer patients at different stages of their treatment...



Rate and Review
Rate this article
Review this article
Log into OpenLearn to leave reviews and join in the conversation.
Article reviews