2 Stress and the brain
Following on from the consideration of stressful life events, and in the knowledge that such events are often linked to the development of depression and anxiety, in this section we look more closely at the biological stress response and its effects on the brain.
The stress response evolved as a coordinated survival reaction to stimuli perceived to be threatening. There are two strands to the stress response. One elicits extremely rapid responses to cope with an emergency. This operates via the SNS and triggers the release of hormones such as adrenalin, which increases alertness. It also increases heart rate so that blood, and the oxygen and nutrients it carries, get to muscles used in running or fighting quickly.
The response is triggered in the first instance by the amygdala, which is of central importance in emotional perception and behaviour, and this can result in the detection of the potential threat and danger before we are consciously aware of it. Of course, in some cases, conscious consideration may convince us that there was no real threat! The amygdala releases CRF (corticotrophin-releasing factor) to stimulate the response from the SNS.
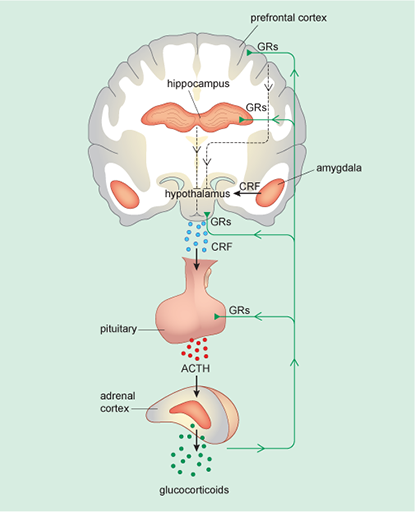
CRF release from the amygdala also triggers the second strand of the stress response – here the CRF signal from the amygdala goes to a brain region called the hypothalamus. The hypothalamus then itself releases CRF as a signal to the pituitary gland, which in turn releases a hormone ACTH (adrenocorticotrophic hormone) into the blood circulation. The main function of ACTH is to signal to the adrenal glands to begin releasing corticosteroids into the blood. This system is called the HPA (hypothalamic–pituitary–adrenal) axis (Figure 6).
If the response is effective (that is, the stressor disappears, or after conscious reflection is judged not to be a danger after all) then body and mind calm down: both the SNS response and the HPA axis become less active, allowing adrenalin levels, heart rate and cortisol levels to return to normal. However, if an external stressor remains, or if an individual continues to feel threatened, the stress response is prolonged and stress becomes chronic. Cortisol and corticosterone are examples of corticosteroids. These are also called glucocorticoids as they affect glucose metabolism.
The effects of prolonged activation of the HPA axis by stressors are of particular interest for understanding depression and anxiety, hence this strand of the stress response will be considered further .
The glucocorticoids produced as a result of HPA axis activity perform a vital function. They mobilise the body’s fat and other energy reserves for release into the bloodstream, where they are then available to sustain the high-energy needs of an individual should there be a prolonged struggle or flight. However, glucocorticoids are damaging to neurons and other cells if present for long periods and in high concentrations. Thus it is important that levels of glucocorticoids are brought back to normal or ‘baseline’ levels as soon as possible.
A mechanism exists to control the level of glucocorticoids and to switch off further production if it is too high. This mechanism involves the hypothalamus, the hippocampus and the prefrontal cortex (all of which are discussed in the related OpenLearn course Emotions and emotional disorders [Tip: hold Ctrl and click a link to open it in a new tab. (Hide tip)] ). Neurons in these brain areas carry special receptors called glucocorticoid receptors (GRs), to which glucocorticoids such as cortisol and corticosterone attach when they are released into the bloodstream. In Activity 6 you will see how glucocorticoid receptors play a crucial part in controlling the HPA axis and hence the stress response, and you will also see what happens when this control fails under conditions of chronic stress.
Figure 6 shows the HPA axis, its links to brain areas such as amygdala, the hippocampus and the prefrontal cortex, and the locations of the GRs.
Activity 5 Cortisol and its inhibitory effect
Where is cortisol produced, and on which part(s) of the HPA (hypothalamic–pituitary–adrenal) axis does it have an inhibitory effect?
Answer
Cortisol is produced by the adrenal cortex. It has an inhibitory effect on the pituitary gland and the hypothalamus. (Note: it also has an inhibitory effect on the hippocampus and the prefrontal cortex but these are not part of the HPA.)
