21.4.3 Mouth, throat and oesophagus problems
Mouth and throat problems are also common in HIV patients. Mouth and throat problems include sores at the corners of the mouth, and fungal infections of the oral mucosa and the oesophagus (the tube that connects the mouth and throat to the stomach). These problems are indicative of different WHO clinical stages (2 to 4), and you should refer PLHIV presenting these to the nearest health centre, with a degree of urgency related to the specific stage.
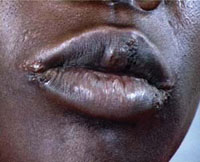
Angular chelitis: These are small chronic sores or cracks around the lips, often at the corners of the mouth (Figure 21.5). Angular chelitis occurs early in HIV infection, and is indicative of WHO clinical stage 2.
Recurrent mouth ulcers (aphtous ulcers): These are small sores or ulcers inside the mouth that appear repeatedly. Ulcers are painful, self-healing and can recur. They can also involve the gums and throat. Note that mouth ulcers are also common in people who are not HIV positive who, for example, have malnutrition. However, in PLHIV, the ulcers are usually severe, making food intake difficult.

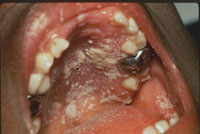
Oral thrush: Also known as oral candidiasis, this is an infection of the lining of the mouth caused by a fungus called candida (the same organism that causes oesophageal thrush which is decribed below, and vaginal candidiasis; see Study Session 31). Oral thrush is a sign of clinical stage 3, and is characterised by white patches (although at times they may appear red) that can be removed with an oral spatula (Figure 21.7).
Oesophageal thrush is a candida infection of the oesophagus. You can identify patients with oesophageal thrush by asking them whether they experience pain while swallowing. A patient who has white patches indicative of oral thrush, and who has severe pain on swallowing, may have oesophageal thrush. Oesophageal thrush is a serious infection, since it can prevent the patient from eating. The pain may be so intense that a patient is unable to swallow. Oesophageal thrush indicates a higher degree of immune suppression than oral thrush, and is a sign of clinical stage 4 (which requires an urgent referral to the nearest health centre).
Oral hairy leukoplakia appears as fine white patches (e.g. white vertical lines) on the side of the tongue, which are painless but cannot be removed. Oral hairy leukoplakia is different from oral thrush or oesophageal thrush in that it does not need to be treated. However, oral hairy leukoplakia (like oral thrush) is still a sign of clinical stage 3, and the patient should be referred to the health centre for health check-ups.
21.4.2 Skin problems
