25.1.1 Strategies for preventing sexual transmission of HIV
Sexual transmission accounts for the majority of HIV infection cases in Ethiopia. Remember from Study Session 20 that HIV can be transmitted via blood or sexual fluids (from a man’s penis or a woman’s vagina) through sexual intercourse, which includes vaginal, anal and oral sex. HIV infection may then occur when infected fluids come into contact with the internal linings of someone’s body (usually the vagina, mouth, or anus) through which the virus can enter the bloodstream. Thus, HIV-transmission prevention through the sexual route aims to avoid or reduce contact between blood and/or sexual fluids of an infected person and the internal linings of another person.
The most widely known strategies for prevention of HIV transmission through the sexual route are often known as the ‘ABC rules’:
- ‘A’ stands for ‘Abstinence’, which means refraining from premarital sexual intercourse.
- ‘B’ stands for ‘Be faithful’, which means maintaining faithful relationships with a long-term partner.
- ‘C’ stands for ‘proper use of Condoms’, which means correct and consistent use of condoms in sexual relations.

Abstinence
Abstinence in principle is the most effective way to prevent sexual HIV transmission, as there is no possibility of direct contact between infected blood and/or sexual fluids and another person’s body. Abstinence is therefore a valid option for individuals who do not have a regular sexual partner, or for PLHIV. However, many sexually active people may find difficulties in maintaining abstinence for long periods of time, making it an unrealistic choice. Moreover, the ‘A’ rule excludes the circumstances of forced sexual relations, as in the cases of rape and coercive marriage of young girls, which unfortunately still occur in Ethiopia.
Maintaining faithful relationships
For faithfulness (the ‘B’ rule of Being faithful) to be successful and minimise transmission of HIV, it is essential that both partners, or the multiple partners in polygamous relationships, know whether they are HIV negative before starting unprotected sexual intercourse. Without condoms there are no barriers for the transmission of HIV between partners. Unprotected sexual intercourse refers to all penetrative practices (through vagina, anus or mouth) performed without a condom. Thus, an important role for health workers such as you is to provide HIV counselling and testing to partners before marriage, or before starting faithful relationships (Study Session 24). It is important for them to realise that, if either of the partners has unprotected sex outside the relationship, it is not only they who are put at higher risk of HIV infection, but also their long-term partner.
In addition, remember that people who have recently been infected with HIV may test negative in the rapid HIV tests while they are in the ‘window period’, but they are still able to transmit HIV to others if they practise unprotected sex.
Based on your previous studies, why may some people test negative on a rapid HIV test during the first few months of infection?
Rapid HIV tests detect antibodies against HIV in the blood. The immune system of individuals recently infected by the virus may take a few months to produce enough antibodies to reach levels detected by HIV rapid tests. These individuals might test negative even though they are infected with HIV.
Therefore, it is important to advise individuals who are about to embark on a faithful relationship not to practise unprotected sexual intercourse before their negative HIV status is confirmed by two separate HIV rapid tests performed at least three months apart. Note also that if one or both partners is HIV positive, maintaining faithful relationships will not be sufficient to prevent HIV infection (this issue will be further discussed in Study Session 29).
Forced marriage of young girls, also known as child brides, may make them more vulnerable to HIV infection. Their future husbands may already be infected with HIV, especially if they are much older. In addition, it may be more difficult for young girls to negotiate sexual decisions with their partners such as maintaining faithful relationships, practicing safer sexual practices (see below) and/or demanding HIV testing.
Issues such as these are discussed in more detail in the Module on Adolescent and Youth Reproductive Health.
Safer sexual practices
As discussed above, abstinence and faithfulness to one’s partner(s) are viable alternatives for some individuals to actively reduce their risk of HIV infection. However, safer sexual practices (also know as safer sex) should be actively encouraged for all of your clients who have an active sexual life outside a faithful relationship. Safer sex includes non-penetrative sexual activities and the correct use of condoms. The goal of safer sex is to reduce the possibility of transmitting HIV by minimising exchange of blood or sexual fluids. Practising safer sexual practices also reduces the risk of other sexually transmitted infections or STIs (Study Session 31). Remember from Study Session 20 that the presence of STIs in an individual increases the likelihood of becoming infected by HIV, so safer sexual practices target HIV transmission both directly and indirectly.
The following four points should form the basis of the education you provide in your community about preventing the further spread of HIV:
1. Individuals with multiple partners increase their chances of contracting or spreading HIV (the higher the number of partners, the more likely it is that HIV will be transmitted from person to person). Being faithful to one partner, or multiple partners in a polygamous marriage, decreases the chances of transmitting or contracting HIV.
2. Non-penetrative sexual practices constitute an alternative way to satisfy sexual needs without being at risk of HIV infection. These alternative practices to sexual intercourse include hugging, kissing, rubbing and masturbation, which are all considered to have an extremely low risk of transmitting HIV infection.
What is the most common route of sexual transmission of HIV in Ethiopia? How can this be avoided?
Heterosexual sex is the most common route of HIV transmission in our country, that is anal and/or vaginal penetrative sex between two people of the opposite sex. There are also reports of anal transmission of HIV between men who have sex with men. Avoiding unprotected penetrative sex constitutes an important preventative measure for HIV infection.
3. If penetrative sexual intercourse is the preferred choice, advise clients on the correct and consistent use of condoms, and the importance of using them every time they have sex. Box 25.1 contains important points to remember about condom use that community members can be made aware of through health education or counselling sessions.
Box 25.1 Important points about condom use for safer sex practices
- Use only latex condoms.
- A new condom should be used for each sexual act.
- A damaged condom can allow HIV to be transmitted and should never be used.
- Many condoms have expiration dates and you should always check the package before use.
- Avoid damage to condoms by always using water-based lubricants. Oil-based lubricants, such as Vaseline or creams, can cause condoms to break and should not be used.
All sexually active individuals should be educated on the correct handling of condoms during and after sexual intercourse, as summarised in Box 25.2 and illustrated in Figure 25.1, which follows it.
Box 25.2 Instructions for using a condom during sexual intercourse
- Do not use an ‘out of date’ condom.
- Open the package carefully. Take care not to tear the condom, or damage it with your fingernails.
- Pinch the end of the condom and place it on the erect penis.
- Still pinching the end, unroll the condom right down the penis.
- If you want to use a lubricant, choose one that is water based. Oil-based lubricants can cause condoms to tear.
- After ejaculation, hold the condom and withdraw the penis before it becomes soft. Never re-use a condom.
- Wrap and dispose of the condom in the trash bin, not in a toilet.
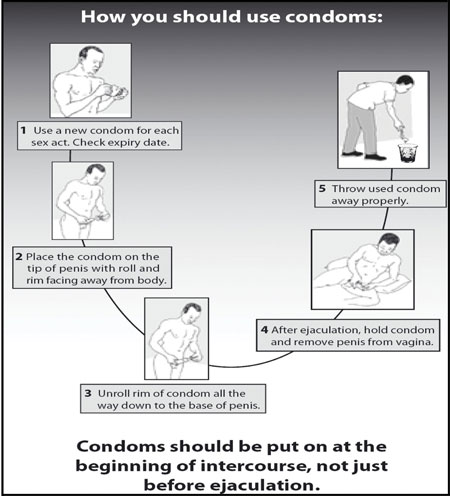
Confusion or misunderstandings on how to use condoms correctly are unnecessary risks for HIV transmission. Make sure that patients and clients have clearly understood these instructions.
4. Finally, safer sex practices should be practiced regularly and consistently, that means in every sexual encounter, to prevent HIV transmission effectively.
Do you think it would give added protection against HIV transmission to use a double condom (two condoms, one on top of another) during penetrative sex?
No. Even though you may think that using double condoms would give added protection against HIV infection, there is no evidence that using them is more effective than single condoms. Rather, the use of double condoms may lead to incorrect use of condoms and increased risk of HIV transmission.
25.1 General principles for preventing HIV infection
