34.2.1 Ascariasis
Like other faeco-oral diseases, you need to know the main features of ascariasis: its infectious agent, occurrence, modes of transmission, symptoms and signs, diagnosis and treatment. Prevention and control measures are similar to those for other faeco-oral diseases, described in earlier study sessions. However, ascariasis requires specific drug treatment based on its symptoms and signs.
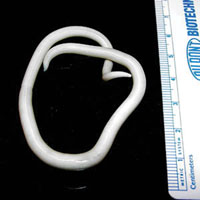
Ascariasis results from infection of the small intestine with a helminth parasite called Ascaris lumbricoides. It is the largest of the intestinal roundworms; mature worms can measure 15–35 cm in length (Figure 34.3). It is the commonest of all the faeco-oral diseases caused by parasitic helminths. It mainly affects children, particularly between three to eight years of age. In Ethiopia, around 37% of the population is estimated to be infected with Ascaris lumbricoides.
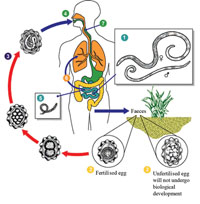
The complicated lifecycle of ascaris worms is shown in Figure 34.4 and is essential for their full development into egg-laying adults. In the descriptions that follow, the numbers relate to the numbers on each stage shown in Figure 34.4. Adult Ascaris lumbricoides worms in the intestines (1) lay eggs which pass out with the faeces (2). The eggs are transmitted faeco-orally by ingestion of contaminated food, water, etc. (stages 2 to 4). The eggs hatch and develop into larvae (immature stage) in the intestines (5). The larvae are carried in the bloodstream to the lungs, where they develop further (6). They migrate upwards from the lungs into the throat (7), where they are swallowed – returning once again to the person’s intestines. Male and female worms mate and the females lay eggs in the intestines (1), which pass out in the faeces (2), and are ingested by new hosts – beginning the lifecycle all over again.
Cases of ascariasis manifest with abdominal discomfort, and live worms may be seen in the stools, vomit or occasionally emerging from the nose. You can make a clinical diagnosis of ascariasis if the patient or the caregiver of a child tells you that long worms have passed with the stool or vomit, or if you are able to see the worms yourself. Eggs in the faeces are too small to see with your eyes, and although they can be identified by laboratory diagnosis of stool samples, there is no need to send samples for investigation or refer the patient – unless there are obvious signs of anaemia (see Box 34.1 in the discussion of hookworm infection later in this study session). You can treat mild cases yourself, and you should also give all children aged between two to five years routine treatment to kill intestinal worms, as described next.
Treatment for ascariasis and routine deworming
If you diagnose ascariasis, the treatment schedule is as given in Table 34.1. There are two drugs (albendazole and mebendazole), both available in either liquid or tablet form. However, even if there are no signs of worm infection, routine deworming is recommended for all children aged 24 months or older who have not been treated in the previous six months. Give every child that you see in this category the appropriate dose of albendazole or mebendazole every six months to treat intestinal worms. Chewable deworming tablets that taste good are available. For children who find swallowing a tablet difficult, you can crush it between two spoons and mix it with a little water to help them to take the dose. This regimen kills hookworms as well as ascaris worms.
![]() Do not give either albendazole or mebendazole to pregnant women who are in their first 14 weeks of pregnancy.
Do not give either albendazole or mebendazole to pregnant women who are in their first 14 weeks of pregnancy.
| Drug | Age 0 to 2 years | Age 2 to 5 years |
|---|---|---|
| Albendazole (400 mg tablet) | None | 1 tablet (400 mg) |
| Medendazole (100 mg or 500 mg tablets) | None | 1 x 500 mg tablet (or 5 x 100 mg tablets) |
| Mebendazole oral suspension (Figure 34.5) | 2.5 teaspoons (250 mg) | None |

34.2 Intestinal roundworms
