38.1.3 First aid and post-exposure prophylaxis for rabies
Wound care and anti-rabies treatment after a dog bite can reduce the occurrence of rabies in a bitten person by up to 90%. This is what you should do if someone is bitten by a dog in your kebele.
First aid
Immediately after a dog bite, you should thoroughly clean and flush the wound with soap and water, detergent, or a substance that kills viruses such as 70% alcohol, tincture of aqueous solution of iodine, or povidone iodine. Continue flushing the wound for at least 15 minutes. The wound should not be sutured (stitched) unless this is essential to stop heavy bleeding. If stitches are required, the wound should not be sutured until after post-exposure prophylaxis has occurred.
Post-exposure prophylaxis for rabies
If a person is bitten by a dog in countries where rabies is endemic, there is no way of being certain that the animal is free from rabies. The bitten person should be given post-exposure prophylaxis (details of the regimen are described below) as soon as possible after the bite. Every year, around 15 million people receive this treatment worldwide, preventing an estimated 327,000 human deaths from rabies.
What do you understand by the term ‘post-exposure prophylaxis’ and where have you met this term in an earlier part of this Module?
Post-exposure prophylaxis (or PEP) means giving preventive therapy very soon after a possible exposure to a life-threatening infectious agent; it is given without waiting for a test to see if the exposure has actually transmitted the infection, because delay could mean that the infection spreads through the person’s body. PEP is given after possible exposure to HIV, for example when a healthcare worker is splashed with blood or is pricked with a needle after injecting a patient with HIV/AIDS.
Post-exposure prophylaxis for HIV is described in Study Session 26 in Part 3 of this Module.
The WHO has published the guidelines in Table 38.1 for PEP following different levels of contact with a suspected rabid animal. Details of the vaccines and rabies immunoglobulin mentioned in the table will be described below.
| Contact category | Action |
|---|---|
| Category I: touching or feeding the animal, licks on intact skin (i.e. no exposure) | None |
| Category II: nibbling of uncovered skin, minor scratches or abrasions without bleeding
| Immediate vaccination and local treatment of the wound |
| Category III: single or multiple bites or scratches that break the skin; contamination of mucus membranes with saliva from licks | Immediate vaccination and administration of rabies immunoglobulin; local treatment of the wound |
Rabies vaccines
Two types of vaccines exist to protect people from rabies after a Category II or III exposure. The older type is made from nerve tissue infected with rabies virus and is given intramuscularly (IM). The newer type of vaccine is made from virus-infected cells grown (cultured) in the laboratory and is safer and more effective. The WHO recommends that the rabies cell-culture vaccine (rabies CCV) should be used in preference to the nerve tissue vaccine wherever possible. Rabies CCV can be given either by intramuscular injection, or intradermally (ID) into the upper arm (Figure 38.4). The intradermal route has been shown to be as safe and effective as the traditional intramuscular route, and is cheaper because it requires less vaccine.
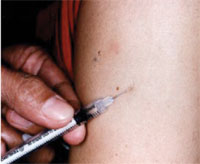
Modern cell-culture vaccines should be given in four or five doses: the dosage for each injection depends on the vaccine type and the route of administration (intramuscular dosages are 0.5 ml or 1.0 ml, whereas the intradermal dosage is only 0.1 ml). If you are referring someone to a health centre for rabies post-exposure prophylaxis, you should tell the patient and their family that it is essential to return at fixed intervals for repeat vaccinations in order to prevent rabies if they have been infected by the bite.
The intramuscular regimen is given at days 0, 3, 7, 14 and 28 after the exposure. The intradermal regimen is given at days 0, 3, 7, 28 and 90 after exposure. There is also a rabies vaccine which is administered at days 0, 7 and 28 days (IM), and rabies duck embryo vaccine, which is administered at day 0, 7 and 21 days (IM or ID). For both these vaccines, a booster dose is given after two to three years.
Rabies immunoglobulin
Specific protection in humans with Category III exposure (see Table 38.1) is provided by injecting a human or equine (horse) immunoglobulin at the site of the bite, as soon as possible after exposure to neutralise the virus. The term ‘immunoglobulin’ refers to a preparation of antibodies made either in humans or in horses who have been vaccinated against rabies. Antibodies from their blood which attack the rabies viruses are harvested and stabilised in an injectable liquid. As much as possible of the dose of rabies immunoglobulin is given into, or as near as possible to, the site of the bite. If there is any remaining in the syringe, it is injected at a different site to elicit active immunity. Human rabies immunoglobulin is given in a single dose of 20 international units (IU) per kilogram (kg) of the person’s body weight. Horse rabies immunoglobulin is cheaper, but less effective and more likely to produce adverse allergic reactions; it is given in a single dose of 40 IU/kg.
38.1.2 Clinical manifestations and diagnosis of rabies
